
Science Magazine – December 14, 2023: The new issue cover features The 2023 Breakthrough of the Year: Obesity meets its match – Blockbuster weight loss drugs show promise for a wider range of health benefits; Runners-Up: At last, modest headway against Alzheimer’s; and Breakdowns of the Year – What went wrong in the world of Science….
Obesity meets its match
Blockbuster weight loss drugs show promise for a wider range of health benefits
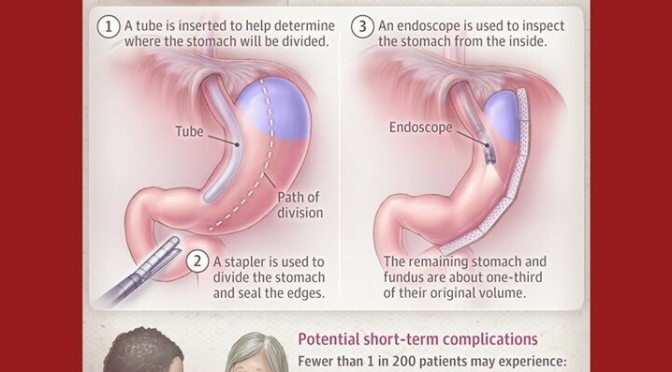
Obesity plays out as a private struggle and a public health crisis. In the United States, about 70% of adults are affected by excess weight, and in Europe that number is more than half. The stigma against fat can be crushing; its risks, life-threatening. Defined as a body mass index of at least 30, obesity is thought to power type 2 diabetes, heart disease, arthritis, fatty liver disease, and certain cancers.
At last, modest headway against Alzheimer’s
Medicine has had little to offer the tens of millions of people worldwide with Alzheimer’s disease, and the few approved treatments have only targeted symptoms. But in January, U.S. regulators greenlit the first drug that clearly, if modestly, slows cognitive decline by tackling the disease’s underlying biology; a second, related treatment is close behind. Neither comes close to a cure, and both have serious risks, but they offer new hope to patients and families.










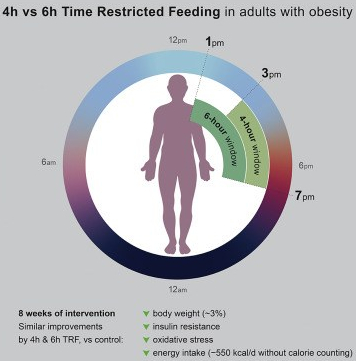 Two daily fasting diets, also known as time-restricted feeding diets, are effective for weight loss, according to a new study published by researchers from the University of Illinois at Chicago.
Two daily fasting diets, also known as time-restricted feeding diets, are effective for weight loss, according to a new study published by researchers from the University of Illinois at Chicago.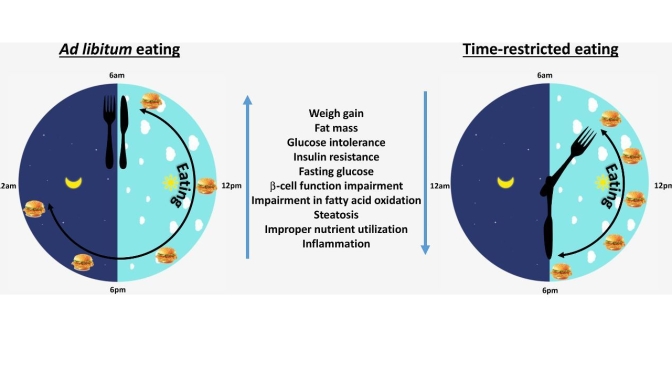
 …the beneficial effects of TRE are dose dependent, with greater reductions in body weight, fat mass, and improvement in glucose tolerance when a 9-h protocol was implemented versus 12 and 15 h. The optimal TRE time frame to recommend for people has not been tested. Clear improvements have been noted after 6-, 8-, 9-, and 10-h protocols. It is likely that the greater time restriction would result in greater weight losses, which may maximize the metabolic benefits.
…the beneficial effects of TRE are dose dependent, with greater reductions in body weight, fat mass, and improvement in glucose tolerance when a 9-h protocol was implemented versus 12 and 15 h. The optimal TRE time frame to recommend for people has not been tested. Clear improvements have been noted after 6-, 8-, 9-, and 10-h protocols. It is likely that the greater time restriction would result in greater weight losses, which may maximize the metabolic benefits.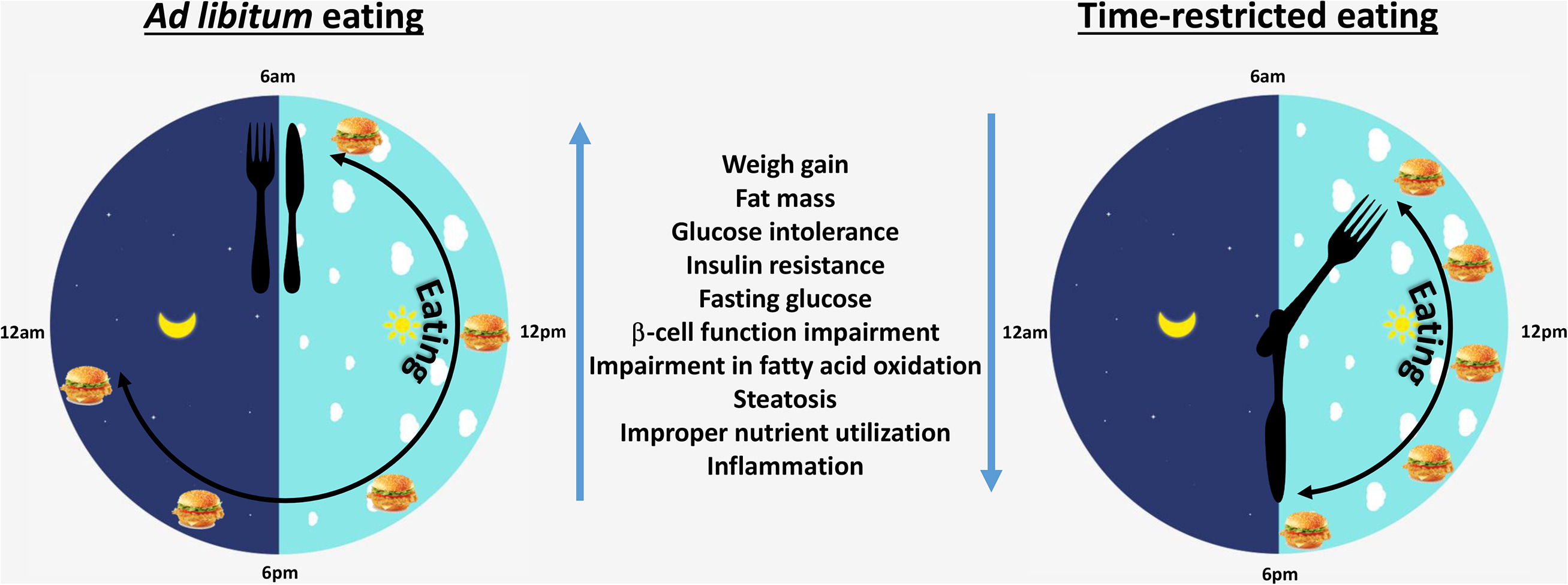




 Nathan Pritikin was a college dropout who became an entrepreneur. While doing research for the government during World War II, he observed that populations that had extremely limited food availability because of the war had substantially reduced mortality from cardiovascular disease—something unexpected at a time when cardiovascular disease was thought to be due to stress.
Nathan Pritikin was a college dropout who became an entrepreneur. While doing research for the government during World War II, he observed that populations that had extremely limited food availability because of the war had substantially reduced mortality from cardiovascular disease—something unexpected at a time when cardiovascular disease was thought to be due to stress. 
 “Maintaining weight loss can get easier over time. Over time, less intentional effort, though not no effort, is needed to be successful. After about two years, healthy eating habits become part of the routine. Healthy choices become more automatic the longer people continue to make them. They feel weird when they don’t.”
“Maintaining weight loss can get easier over time. Over time, less intentional effort, though not no effort, is needed to be successful. After about two years, healthy eating habits become part of the routine. Healthy choices become more automatic the longer people continue to make them. They feel weird when they don’t.”