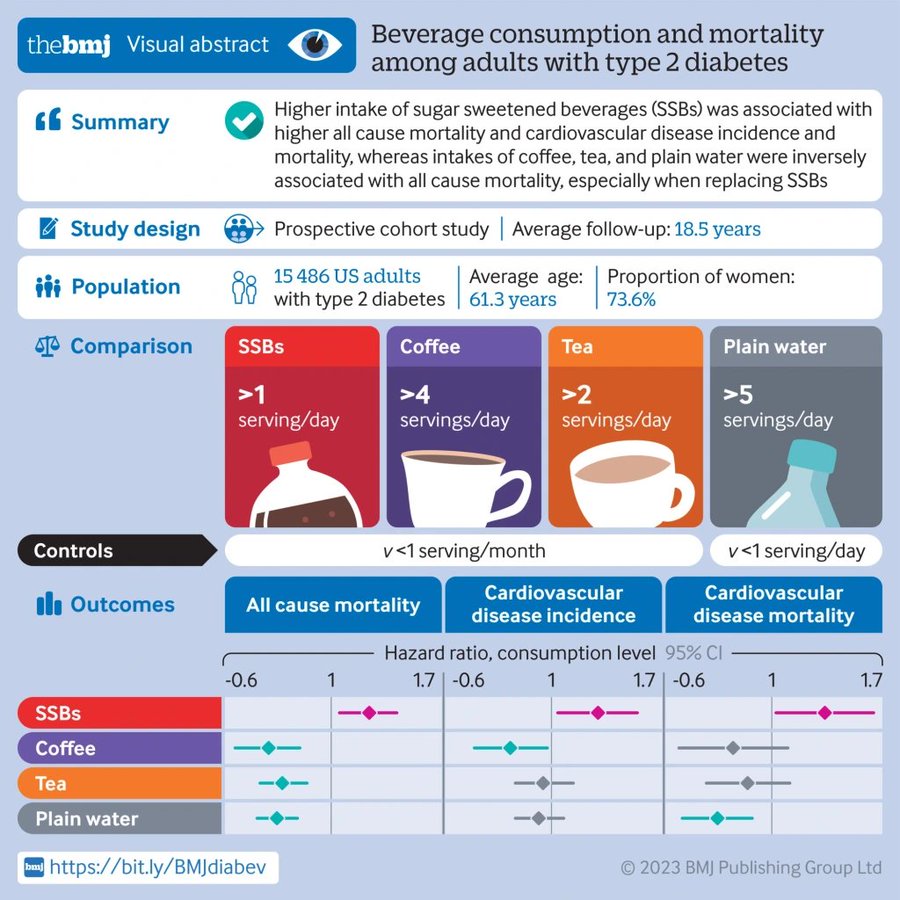
The BMJ (Published April 19, 2023) – Conclusions: Individual beverages showed divergent associations with all cause mortality and CVD outcomes among adults with type 2 diabetes. Higher intake of SSBs was associated with higher all cause mortality and CVD incidence and mortality, whereas intakes of coffee, tea, plain water, and low fat milk were inversely associated with all cause mortality. These findings emphasize the potential role of healthy choices of beverages in managing the risk of CVD and premature death overall in adults with type 2 diabetes.
Tag Archives: Studies
Studies: Alcohol Abuse Increases Chronic Pain
Scripps Research (April 21, 2023) – Chronic alcohol consumption may make people more sensitive to pain through two different molecular mechanisms—one driven by alcohol intake and one by alcohol withdrawal. That is one new conclusion by scientists at Scripps Research on the complex links between alcohol and pain.
The research, published in the British Journal of Pharmacology on April 12, 2023, also suggests potential new drug targets for treating alcohol-associated chronic pain and hypersensitivity.
“There is an urgent need to better understand the two-way street between chronic pain and alcohol dependence,” says senior author Marisa Roberto, PhD, the Schimmel Family Chair of Molecular Medicine, and a professor of neuroscience at Scripps Research. “Pain is both a widespread symptom in patients suffering from alcohol dependence, as well as a reason why people are driven to drink again.”
Alcohol use disorder (AUD), which encompasses the conditions commonly called alcohol abuse, alcohol dependence and alcohol addiction, affects 29.5 million people in the U.S. according to the 2021 National Survey on Drug Use and Health. Over time, AUD can trigger the development of numerous chronic diseases, including heart disease, stroke, liver disease and some cancers.
Aging: 34% Of The Elderly Feel ‘Socially Isolated’
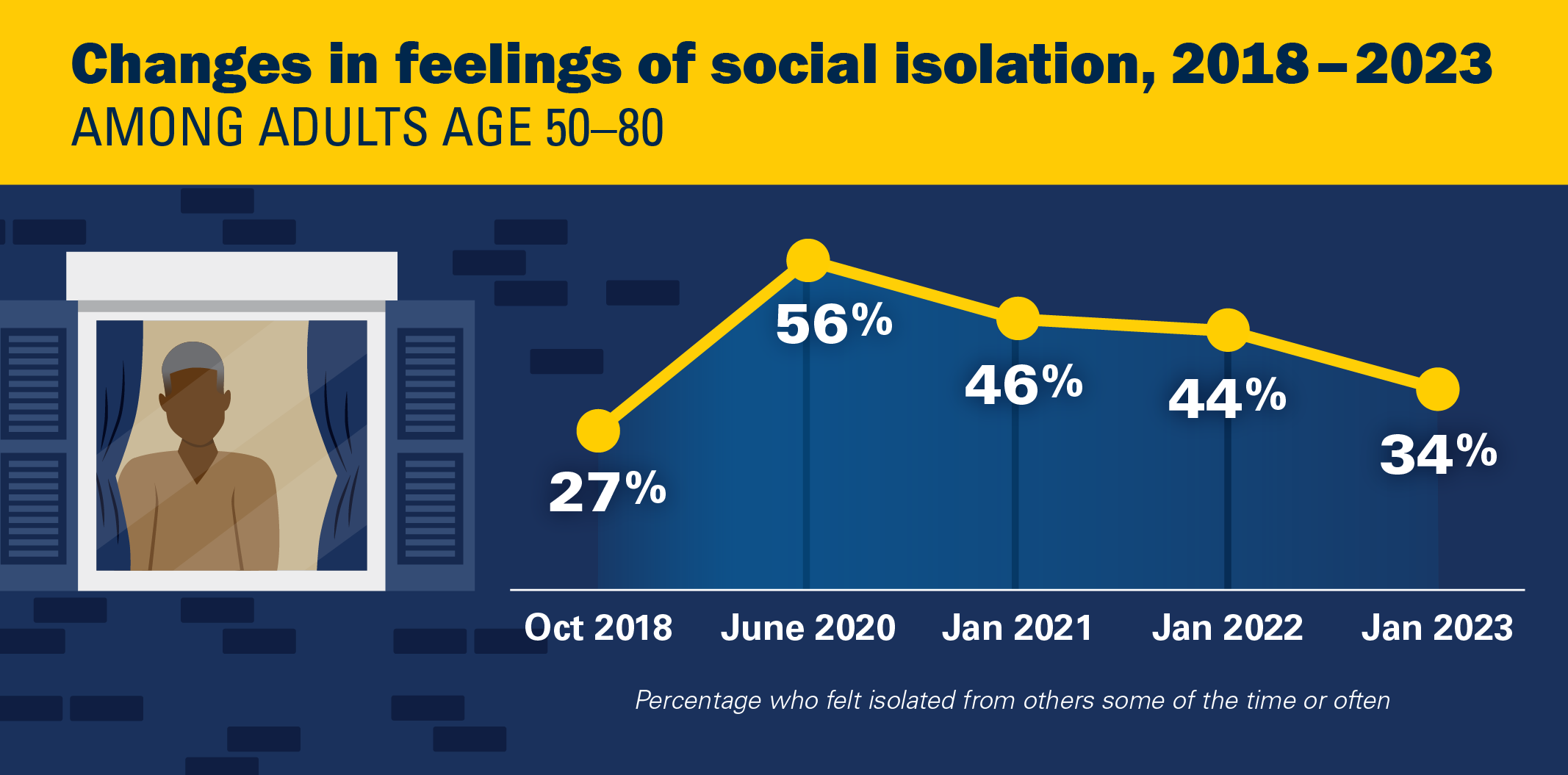
In 2023, one in three adults age 50–80 (34%) reported feeling isolated from others (29% some of the time, 5% often) in the past year. This represents a marked decline compared with the 56% (43% some of the time, 13% often) who felt isolated in 2020, but a greater proportion than the 27% (22% some of the time, 5% often) who reported feeling isolated in 2018.

National Poll On Healthy Aging (March 2023) – More than one in three older adults (37%) reported feeling a lack of companionship (29% some of the time, 8% often) in the past year, compared with 41% (32% some of the time, 9% often) in 2020, and 34% (26% some of the time, 8% often) in 2018.
One in three older adults (33%) reported infrequent contact (once a week or less) with people from outside their home in 2023 (14% once a week, 10% every 2–3 weeks, 9% once a month or less). This rate of infrequent contact was significantly less than the 46% reported in 2020 (19% once a week, 11% every 2–3 weeks, 16% once a month or less), but higher than the 28% reported in 2018 (15% once a week, 7% every 2–3 weeks, 6% once a month or less).

Covid-19: Heart Disease Risks Rise After Infection
In December 2020, a week before cardiologist Stuart Katz was scheduled to receive his first COVID-19 vaccine, he came down with a fever. He spent the next two weeks wracked with a cough, body aches and chills. After months of helping others to weather the pandemic, Katz, who works at New York University, was having his own first-hand experience of COVID-19.
On Christmas Day, Katz’s acute illness finally subsided. But many symptoms lingered, including some related to the organ he’s built his career around: the heart. Walking up two flights of stairs would leave him breathless, with his heart racing at 120 beats per minute. Over the next several months, he began to feel better, and he’s now back to his normal routine of walking and cycling. But reports about COVID-19’s effects on the cardiovascular system have made him concerned about his long-term health. “I say to myself, ‘Well, is it really over?’” Katz says.
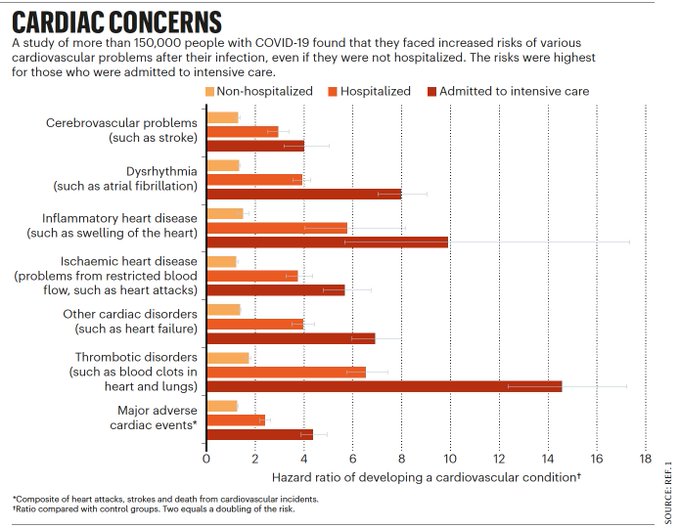
In one study1 this year, researchers used records from the US Department of Veterans Affairs (VA) to estimate how often COVID-19 leads to cardiovascular problems. They found that people who had had the disease faced substantially increased risks for 20 cardiovascular conditions — including potentially catastrophic problems such as heart attacks and strokes — in the year after infection with the coronavirus SARS-CoV-2. Researchers say that these complications can happen even in people who seem to have completely recovered from a mild infection.
Some smaller studies have mirrored these findings, but others find lower rates of complications. With millions or perhaps even billions of people having been infected with SARS-CoV-2, clinicians are wondering whether the pandemic will be followed by a cardiovascular aftershock. Meanwhile, researchers are trying to understand who is most at risk of these heart-related problems, how long the risk persists and what causes these symptoms.
Women’s Health: How Mammograms Can Reveal Cardiovascular Disease
The routine mammograms women receive to check for breast cancer may also offer clues to their risk for heart disease, new research suggests.
White spots or lines visible on mammograms indicate a buildup of calcium in breast arteries. This breast arterial calcification is different from coronary artery calcification, which is known to be a marker for higher cardiovascular risk. For the study, researchers followed 5,059 postmenopausal women (ages 60 to 79) for six and a half years. They found that those with breast arterial calcification were 51% more likely to develop heart disease or have a stroke than those without calcification. The study was published March 15, 2022, in Circulation: Cardiovascular Imaging.