
Tag Archives: Physical Exercise
Study: “Intensive Diet And Exercise” Reverses Type 2 Diabetes In 61% Of Patients
From The Lancet Diabetes & Endocrinology (June 2020):
Our findings show that the intensive lifestyle intervention led to significant weight loss at 12 months, and was associated with diabetes remission in over 60% of participants and normoglycaemia in over 30% of participants. The provision of this lifestyle intervention could allow a large proportion of young individuals with early diabetes to achieve improvements in key cardiometabolic outcomes, with potential long-term benefits for health and wellbeing.

Health & Fitness: “What Is Exercise Physiology?” (Penn Medicine Video)
Exercise physiologists are healthcare professionals that work with patients who are deconditioned or have a variety of different health complications. They work with pulmonary and cardiac patients, as well as competitive athletes with a wide range of fitness issues.
Penn Medicine’s Christopher J. Kusmiesz, MS describes his role as “assessing a patient’s fitness level and providing recommendations and guidance so they can improve and reach their health and fitness goals.”
Exercise physiologists at Penn uses patient test results, recommendations from their cardiologist and the patient’s own goals to create an exercise program that is unique to each patient.
Exercise Health Benefits: “Should I Go To The Gym Today?” (MGH Video)
This presentation by Julia Browne, PhD, a clinical and research fellow in the Center of Excellence for Psychosocial and Systemic Research at Massachusetts General Hospital and Harvard Medical School was part of Schizophrenia Education Day 2019.
Health Infographics: Importance Of “Physical Activity And Ageing” (BMJ)
Studies: “Why Your Brain Needs Exercise” (Scientific American)
From a Scientic American online article:
 In our own study of more than 7,000 middle-aged to older adults in the U.K., published in 2019 in Brain Imaging and Behavior, we demonstrated that people who spent more time engaged in moderate to vigorous physical activity had larger hippocampal volumes. Although it is not yet possible to say whether these effects in humans are related to neurogenesis or other forms of brain plasticity, such as increasing connections among existing neurons, together the results clearly indicate that exercise can benefit the brain’s hippocampus and its cognitive functions.
In our own study of more than 7,000 middle-aged to older adults in the U.K., published in 2019 in Brain Imaging and Behavior, we demonstrated that people who spent more time engaged in moderate to vigorous physical activity had larger hippocampal volumes. Although it is not yet possible to say whether these effects in humans are related to neurogenesis or other forms of brain plasticity, such as increasing connections among existing neurons, together the results clearly indicate that exercise can benefit the brain’s hippocampus and its cognitive functions.
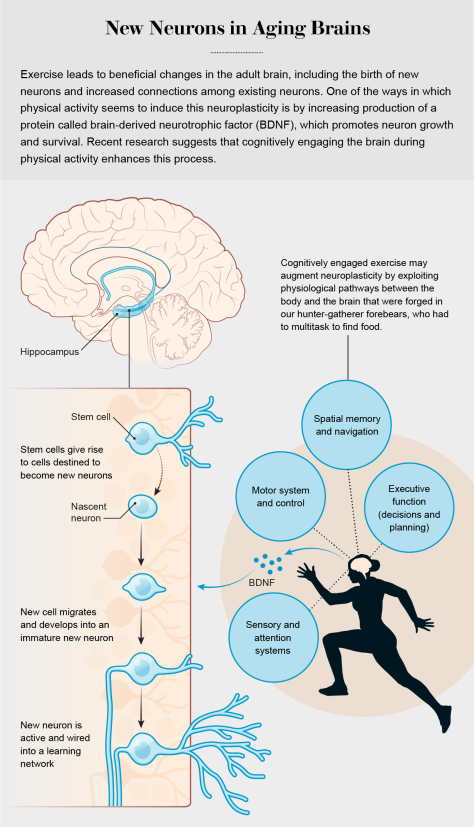
In fact, a growing body of research suggests that exercise that is cognitively stimulating may indeed benefit the brain more than exercise that does not make such cognitive demands. For example, Gerd Kempermann and his colleagues at the Center for Regenerative Therapies Dresden in Germany explored this possibility by comparing the growth and survival of new neurons in the mouse hippocampus after exercise alone or after exercise combined with access to a cognitively enriched environment. They found an additive effect: exercise alone was good for the hippocampus, but combining physical activity with cognitive demands in a stimulating environment was even better, leading to even more new neurons. Using the brain during and after exercise seemed to trigger enhanced neuron survival.
To read more: https://www.scientificamerican.com/article/why-your-brain-needs-exercise/
Exercise Studies: Older Adults’ “Fragmented Physical Exercise” Linked To Higher Death Rates
From a National Institute On Aging release:

Fragmented physical activity, but not total daily activity, was significantly associated with death, the researchers found. For each 10% higher degree of activity fragmentation, mortality risk was 49% greater. The duration of physical activity also mattered: Participants who frequently engaged in short bouts of activity of less than five minutes were more likely to die than those whose activity bouts lasted five minutes or longer. These associations held after adjusting for age, sex, body mass index and other factors.
Daily physical activity, which benefits health and quality of life, typically decreases in older adults. A new study shows that higher fragmentation of that activity — more transitions from activity to sedentariness — may be a better indicator of risk of death than a person’s overall level of physical activity.
Researchers from the Johns Hopkins Bloomberg School of Public Health, Baltimore, analyzed data from the NIA-supported Baltimore Longitudinal Study of Aging (BLSA), looking at a week’s worth of minute-by-minute physical activity for 548 healthy participants age 65 and older (average age, 76).
To read more: https://www.nia.nih.gov/news/fragmented-physical-activity-linked-higher-risk-death-older-adults
Chronic Pain: Cornell To Study Behavioral Change (Physical Exercise), Non-Drug Treatments For Pain
From a Cornell University news release:
 “Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?”
“Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?”
More than 100 million Americans suffer from chronic pain – outnumbering those affected by heart disease, diabetes and cancer combined.
To develop innovative approaches to pain management, a team of behavioral and social science researchers on Cornell’s Ithaca campus, clinical researchers at Weill Cornell Medicine and computer scientists at Cornell Tech has received a five-year, $3 million grant from the National Institute on Aging, part of the National Institutes of Health (NIH).
To read more: http://news.cornell.edu/stories/2019/10/nih-grant-will-fund-non-pharmacological-pain-research










