The Lancet (January 2023) – For our 200th anniversary year we have identified five Spotlight subjects of particular importance. Watch as Richard Horton, Editor-in-Chief, and other Lancet Editors around the world outline these Spotlights and discuss priorities for the future of health.
This year, we draw attention to the most critical issues impacting health globally, the extraordinary people involved in tackling them, and the voices of those most impacted. For five Spotlights, we will run a programme of activities to bring these issues to life and convene the right people and resources in order to drive change in these areas.
Spotlight on Universal Health Coverage
Ensuring all populations globally have access to affordable, quality health care
Spotlight on Research for Health
Prioritising evidence to guide and inform decision making
Spotlight on Child and Adolescent Health
Prioritising the health needs of children and adolescents now
Spotlight on Health and Climate Change
Tackling climate change through the lens of human health
Spotlight on Mental Health
Implementing sustainable global mental health in a fragmenting world
















 Prevention
Prevention
 Smartphone app-based platforms for urine testing could improve adherence to albumin creatinine ratio (ACR) testing. One study showed screening of at-risk patients almost doubled with a home urine test kit that uses a smartphone camera to easily and accurately quantify ACR from a user-performed urine dipstick. If independently validated in a large, diverse population, this low-cost strategy could change the often dim trajectory for individuals with declining kidney function.
Smartphone app-based platforms for urine testing could improve adherence to albumin creatinine ratio (ACR) testing. One study showed screening of at-risk patients almost doubled with a home urine test kit that uses a smartphone camera to easily and accurately quantify ACR from a user-performed urine dipstick. If independently validated in a large, diverse population, this low-cost strategy could change the often dim trajectory for individuals with declining kidney function. 

 WHO’s definition of health is famously “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity”. One of the oldest medical texts we know of, The Science of Medicine attributed to Hippocrates, sets out the goal of medicine in comparable terms: “the complete removal of the distress of the sick”.
WHO’s definition of health is famously “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity”. One of the oldest medical texts we know of, The Science of Medicine attributed to Hippocrates, sets out the goal of medicine in comparable terms: “the complete removal of the distress of the sick”.
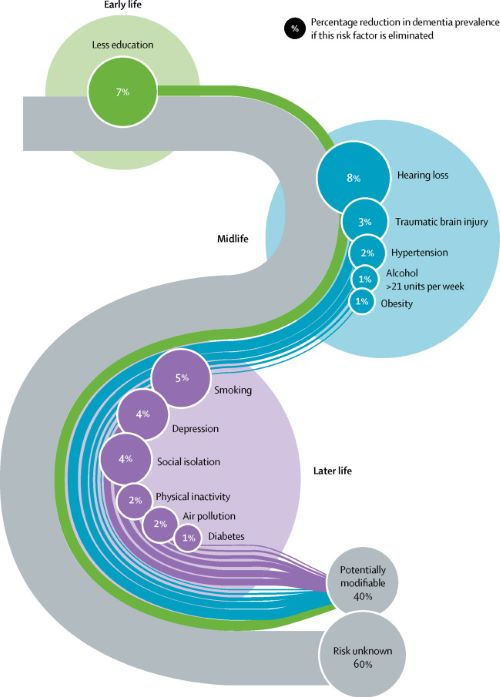
 …the researchers demonstrated that the biggest drop in cognitive ability occurs at the slightest level of hearing loss — a decline from zero to the “normal” level of 25 decibels, with smaller cognitive losses occurring when hearing deficits rise from 25 to 50 decibels.
…the researchers demonstrated that the biggest drop in cognitive ability occurs at the slightest level of hearing loss — a decline from zero to the “normal” level of 25 decibels, with smaller cognitive losses occurring when hearing deficits rise from 25 to 50 decibels.