UCSF orthopedic surgeon Dr. Paul Toogood discusses the types and origins or Arthritis.
From Scientific American (June 23, 2020):
 In fact, research on actual cases, as well as models of the pandemic, indicate that between 10 and 20 percent of infected people are responsible for 80 percent of the coronavirus’s spread.
In fact, research on actual cases, as well as models of the pandemic, indicate that between 10 and 20 percent of infected people are responsible for 80 percent of the coronavirus’s spread.
Researchers have identified several factors that make it easier for superspreading to happen. Some of them are environmental.
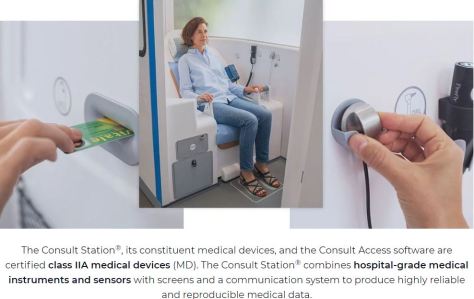
H4D facilitates access to healthcare by allowing patients to consult a doctor remotely in the Consult Station®, the first connected local telemedicine booth. This medical device allows quality healthcare to be delivered for primary care, occupational health, and general health promotion.
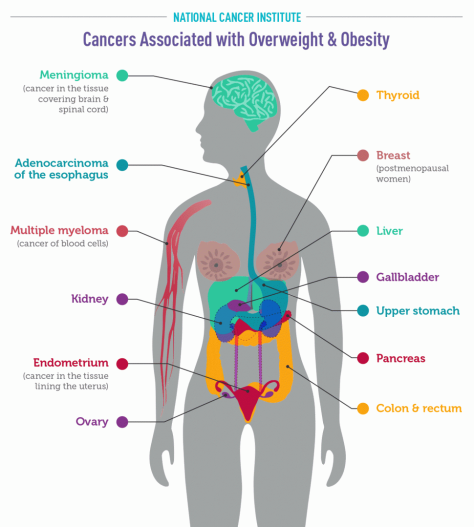
There is consistent evidence that higher amounts of body fat are associated with increased risks of a number of cancers (6), including:
 The Wall Street Journal looks at how air travel will change and what it will be like to fly after the pandemic.
The Wall Street Journal looks at how air travel will change and what it will be like to fly after the pandemic.
From the Wall Street Journal (June 8, 2020):
“We have to operate a hospital within a hospital, taking care of the needs for patients who have had strokes or a newborn delivery or need surgery while dealing with an otherwise healthy 35-year-old who picked up Covid-19 at a social event,” says James Linder, chief executive of Nebraska Medicine…
 For instance, more hospitals are remotely triaging and registering patients before they even arrive. Clinicians can consult with patients from their home via telemedicine to help determine how sick they are and if they need to come to the ER at all. From there, admissions are made with as little contact with staff or other patients as possible.
For instance, more hospitals are remotely triaging and registering patients before they even arrive. Clinicians can consult with patients from their home via telemedicine to help determine how sick they are and if they need to come to the ER at all. From there, admissions are made with as little contact with staff or other patients as possible.
Hospitals are rethinking how they operate in light of the Covid-19 pandemic—and preparing for a future where such crises may become a grim fact of life.
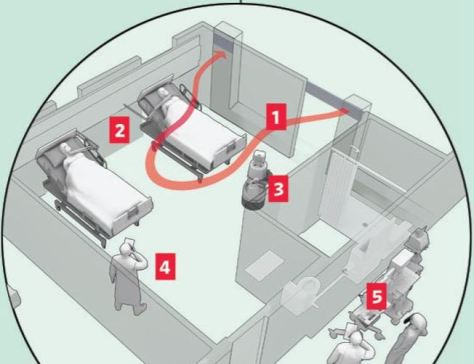
 With the potential for resurgences of the coronavirus, and some scientists warning about outbreaks of other infectious diseases, hospitals don’t want to be caught flat-footed again. So, more of them are turning to new protocols and new technology to overhaul standard operating procedure, from the time patients show up at an emergency room through admission, treatment and discharge.
With the potential for resurgences of the coronavirus, and some scientists warning about outbreaks of other infectious diseases, hospitals don’t want to be caught flat-footed again. So, more of them are turning to new protocols and new technology to overhaul standard operating procedure, from the time patients show up at an emergency room through admission, treatment and discharge.
We observed that increased adherence to the MedDiet modulates specific components of the gut microbiota that were associated with a reduction in risk of frailty, improved cognitive function and reduced inflammatory status.
Dr Philip Smith, Digital and Education Editor of Gut and Consultant Gastroenterologist at the Royal Liverpool Hospital interviews Professor Paul O’Toole; who is Professor of Microbial Genomics, Head of School of Microbiology and Principal Investigator in APC Microbiome Ireland, an SFI funded centre at University College Cork, Ireland, on “Mediterranean diet intervention alters the gut microbiome in older people reducing frailty and improving health status: the NU-AGE 1-year dietary intervention across 5 European countries” published in paper copy in Gut in July 2020.

In this audio interview conducted on June 3, 2020, the editors discuss two new studies: one comparing test swabs collected by health care workers with swabs collected by the patients themselves and one assessing hydroxychloroquine treatment in people who had been exposed to Covid-19 but weren’t yet ill.
The continuing spread of SARS-CoV-2 remains a Public Health Emergency of International Concern. What physicians need to know about transmission, diagnosis, and treatment of Covid-19 is the subject of ongoing updates from infectious disease experts at the Journal.
Eric Rubin is the Editor-in-Chief of the Journal. Lindsey Baden is a Deputy Editor of the Journal. Stephen Morrissey, the interviewer, is the Executive Managing Editor of the Journal.