CBS Sunday Morning (February 18, 2024): This isn’t your grandfather’s old age. CBS News chief medical correspondent Dr. Jonathan LaPook talks with experts about the distinctions between normal and abnormal aging as it affects memory issues, a workforce continuing beyond traditional retirement age, and the testing of surgeons who currently work without age limits.
Tag Archives: Older Adults
Reviews: “A New Way Of Thinking About Aging”
“People 50 and older hold the vast majority of wealth in the country, but we’re producing products and services for people who don’t have nearly as much money to spend…”

April 27, 2023: Thanks to advances in medicine and public health, people are living longer, healthier lives. The world’s population of people 60 and older is growing five times faster than the population as a whole. Global life expectancy has doubled since 1900, and experts say that children born in developed countries now have a good chance of living to 100.

A “silver tsunami” is already sweeping the U.S. labor force: the Bureau of Labor Statistics projects that 36% of people ages 65–69 will remain on the job in 2024 — up significantly from the 22% who were working in 1994.
These longer-lived, longer-working individuals generate an ever-bigger slice of global GDP and control an expanding tranche of global wealth. In her recent book Stage (Not Age), Golden estimates that the “longevity economy” is worth more than $22 trillion — $8.3 trillion in the United States alone.
That may be a conservative figure: AARP (the organization formerly known as the American Association of Retired Persons) estimates that people over 50 already account for half of consumer spending worldwide, or $35 trillion. (This range of figures may have to do with how “older adult” is defined: The term is variously used to refer to people over the ages of 65, 60, or — sorry, Gen Xers — 50.)
Aging: 34% Of The Elderly Feel ‘Socially Isolated’
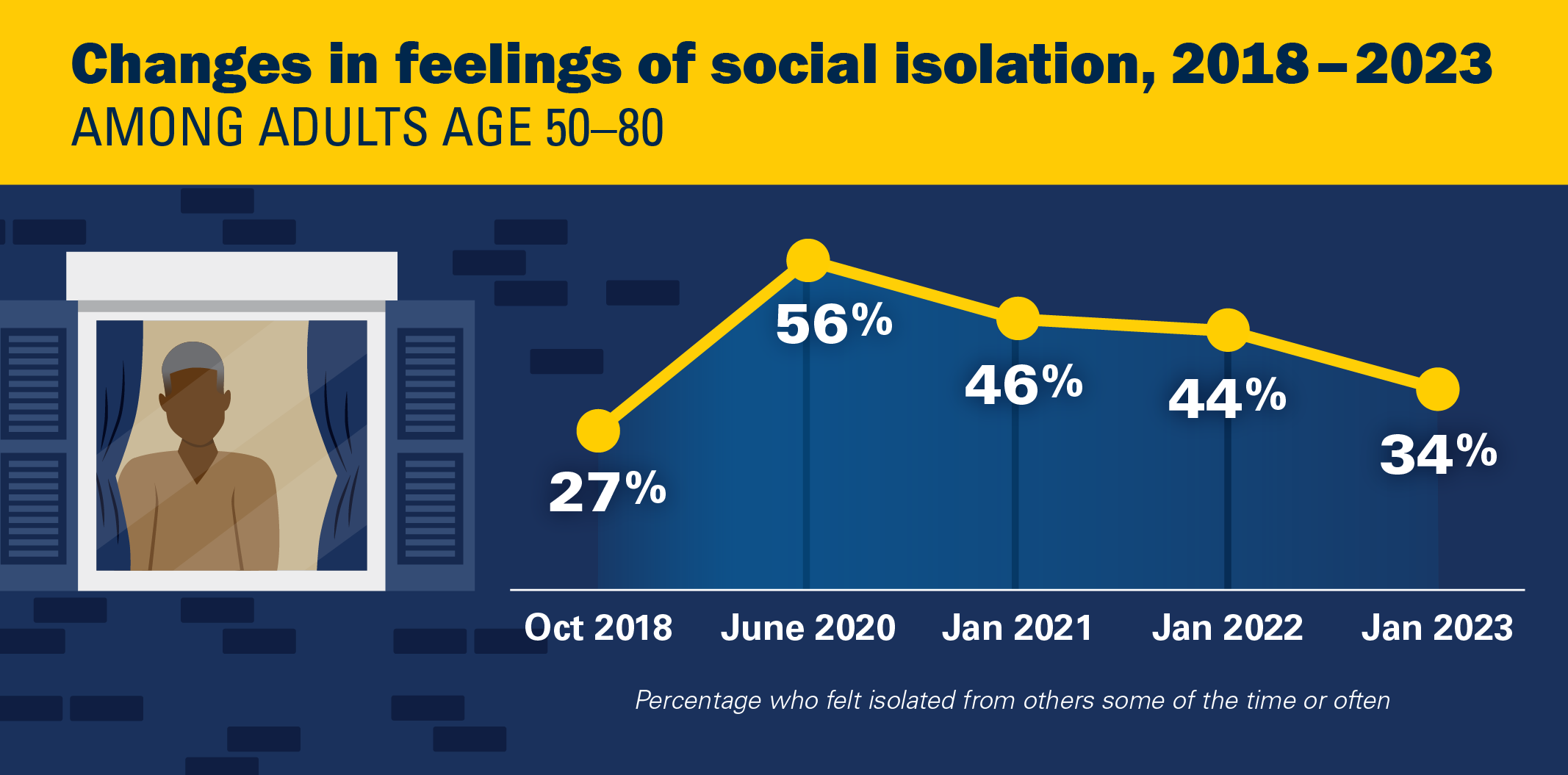
In 2023, one in three adults age 50–80 (34%) reported feeling isolated from others (29% some of the time, 5% often) in the past year. This represents a marked decline compared with the 56% (43% some of the time, 13% often) who felt isolated in 2020, but a greater proportion than the 27% (22% some of the time, 5% often) who reported feeling isolated in 2018.

National Poll On Healthy Aging (March 2023) – More than one in three older adults (37%) reported feeling a lack of companionship (29% some of the time, 8% often) in the past year, compared with 41% (32% some of the time, 9% often) in 2020, and 34% (26% some of the time, 8% often) in 2018.
One in three older adults (33%) reported infrequent contact (once a week or less) with people from outside their home in 2023 (14% once a week, 10% every 2–3 weeks, 9% once a month or less). This rate of infrequent contact was significantly less than the 46% reported in 2020 (19% once a week, 11% every 2–3 weeks, 16% once a month or less), but higher than the 28% reported in 2018 (15% once a week, 7% every 2–3 weeks, 6% once a month or less).

REVIEWS: THE TOP 5 ARTICLES ON HEALTHY AGING IN 2022
National Institute on Aging – As 2022 comes to a close, NIA invites you to explore some of the most popular health information topics from this past year:
High Blood Pressure and Older Adults
— High blood pressure, or hypertension, is common in older adults. The good news is that blood pressure can be controlled in most people.
What Is Menopause?
— Menopause is a normal part of aging for women, but it affects every woman differently.
Memory, Forgetfulness, and Aging: What’s Normal and What’s Not?
— As you age, you may wonder about the difference between normal, age-related forgetfulness and a serious memory problem, such as dementia.
Shingles
— Shingles is a disease that triggers a painful skin rash. About one in three people will get shingles, but there is a vaccine for older adults to help prevent the disease.
Vitamins and Minerals for Older Adults
— Vitamins and minerals are types of nutrients that your body needs to survive and stay healthy.
Health Plans: Pros & Cons Of Medicare Advantage
Consumer Reports – November 2022:



For More Information
When you’re ready to start reviewing plans, check out the Medicare plan finder tool, which will let you compare Medicare Advantage and Part D prescription drug plans available in your area. You can also get this information by calling Medicare at 800-633-4227.
If you’re looking for a Medigap plan, you can also start at medicare.gov, where you can compare the different types of coverage, as well as find the policies available in your ZIP code.
Another good resource is the State Health Insurance Assistance Program (SHIP), which provides free guidance over the phone. To find your state’s program, go to shiphelp.org or call 877-839-2675.
Aging: ‘Healthy Longevity’ Journal – November 2022

Inside the November 2022 Issue:
Research & review on #Alzheimers, global burden of benign prostatic hyperplasia, #WHO def of vitality capacity, IPD meta on social connection & #cognition, #oralhealth for older people & more.
Hope on the horizon for Alzheimer’s disease treatment?
Social connectedness and cognitive decline
Time to take oral health seriously
Aging: How Regenerative Medicine Slows The Clock
“Diverse aging populations, vulnerable to chronic disease, are at the cusp of a promising future. Indeed, growing regenerative options offer opportunities to boost innate healing, and address aging-associated decline. The outlook for an extended well-being strives to achieve health for all,”
Andre Terzic, M.D., Ph.D., a Mayo Clinic cardiologist
Regenerative medicine could slow the clock on degenerative diseases that often ravage the golden years, a Mayo Clinic study finds. Life span has nearly doubled since the 1950s, but health span — the number of disease-free years — has not kept pace. According to a paper published in NPJ Regenerative Medicine., people are generally living longer, but the last decade of life is often racked with chronic, age-related diseases that diminish quality of life. These final years come with a great cost burden to society.
Researchers contend that new solutions for increasing health span lie at the intersection of regenerative medicine research, anti-senescent investigation, clinical care and societal supports. A regenerative approach offers hope of extending the longevity of good health, so a person’s final years can be lived to the fullest.
Aging: How Biomarkers Help Diagnose Dementia
Biomarkers are measurable indicators of what’s happening in your body. They can be found in blood, other body fluids, organs, and tissues, and can be used to track healthy processes, disease progression, or even responses to a medication. Biomarkers are an important part of dementia research.
Old Age: ‘Hyperexcitable Neurons’ Interrupt Sleep
For many older adults, a good night’s rest is elusive. The implications of chronically poor sleep can be far-reaching and include a decline in cognitive functioning and detrimental effects on health and general well-being. Fortunately, relief may be in sight.
A new study led by investigators at the Stanford University School of Medicine shows that neurons in the lateral hypothalamus, a brain region, play a pivotal role in sleep loss in old mice. More specifically, the arousal-promoting hypocretin neurons become hyperexcitable, driving sleep interruptions.
Read the full story: https://stan.md/3JQ7z77
Luis de Lecea, PhD, is a professor of psychiatry and behavioral sciences at Stanford Medicine. He is the study’s senior author and hopes the finding could pave the way to new drug treatments for age-related sleep problems in humans.
Shi-Bin Li, PhD, is an instructor in the Psychiatry and Behavioral Sciences department at Stanford Medicine. He is also a basic life research scientist in the de Lecea lab, and is the lead author of the study.
Dementia Study: A High-Fiber Diet May Lower Risk
Fiber is known for keeping your digestive system healthy and lowering cholesterol levels. Now, study findings suggest it also may protect the brain from dementia.
The study involved approximately 3,700 healthy adults, ages 40 to 64, who completed routine dietary surveys for 16 years. Researchers then monitored the participants for two decades to see which ones developed dementia. The study revealed that people who consumed the most daily fiber had the lowest rates of dementia. The reverse also was true — those who ate the least fiber had the highest rates. Specifically, the low-risk group consumed an average of 20 grams daily, while those with the highest risk averaged only 8 grams. (The USDA recommends that men over age 50 eat 30 grams of fiber daily.)











