Science Magazine – September 29, 2023: This special issue examines the threats to human health and how they can be mitigated.
AN UNHEALTHY CLIMATE
Introducing a special issue of Science
Earth scientists often call climate change a “great global experiment,” which humanity is heedlessly performing as we pump greenhouse gases into the atmosphere. The dire consequences are already becoming clear—not just for the workings of the planet, but for our own health. Over the next few days, the stories in this special package will explore the threats, and how we can minimize them.
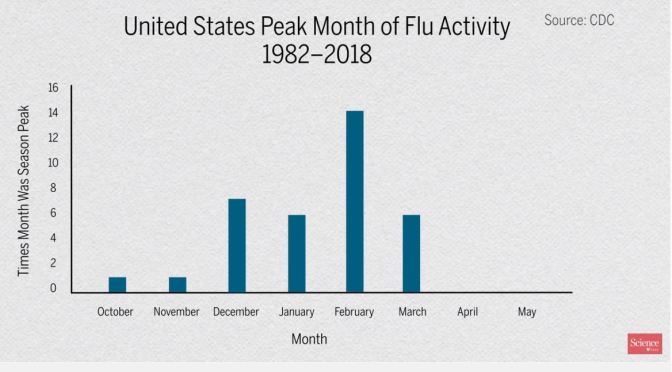
Will flu outbreaks ease in a warming world?
From cold viruses to influenza to respiratory syncytial virus, viruses that spread through the air cause billions of infections each year. That makes it important to understand how they will respond to climate change. But little is known so far, except that different viruses will react differently. Measles, for instance, spreads efficiently in all climates, suggesting global warming will make little difference to its transmission.