Tag Archives: Colorectal Cancer
CANCER: WHAT AGE SHOULD YOU GET A COLONOSCOPY?
According to the American Cancer Society, colorectal cancer is the third most common cancer diagnosed in both men and women in the United States. While diagnoses are decreasing in people over the age of 50, there’s been an increase for those who are younger.
For more information on why you should get a colonoscopy and how to schedule yours today, please visit https://cle.clinic/3oqWdy6
Harvard Study: Vitamin D Lowers The Risk Of Young-Onset Colorectal Cancer
Medicine: When Colon Cancer Spreads To The Liver (Mayo Clinic Video)
Colorectal cancer is a leading cancer among men and women around the world. Many colorectal cancers are likely to spread to other organs, with the most common site of metastases being the liver. In this Mayo Clinic Minute, Dr. Sean Cleary, a hepatobiliary and pancreas surgeon at Mayo Clinic explains what this means to patients.
Infographic: ‘The Most Common Types Of Cancer’

Health Infographics: “Cancers Associated With Overweight & Obesity”
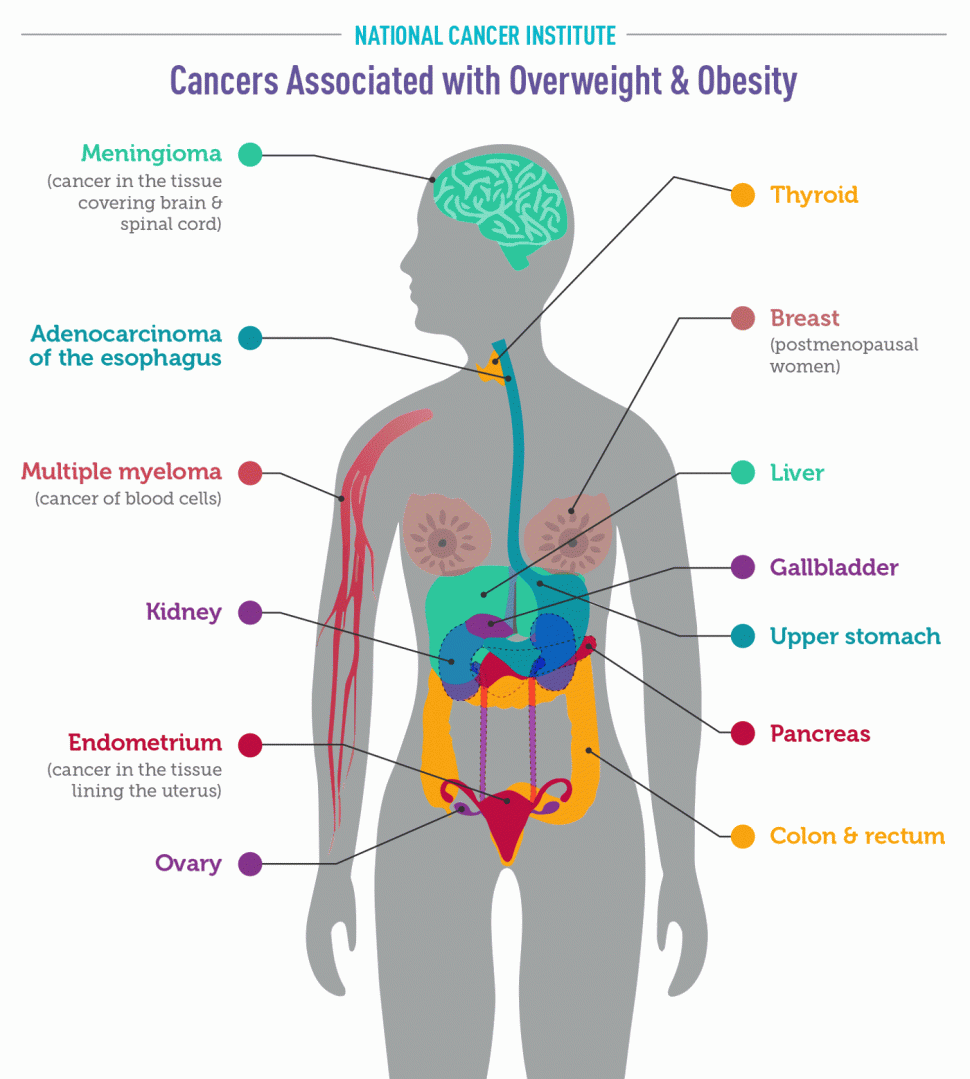
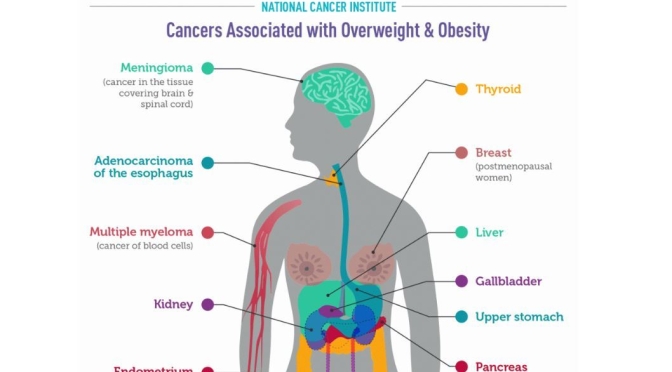
There is consistent evidence that higher amounts of body fat are associated with increased risks of a number of cancers (6), including:
- Endometrial cancer: Obese and overweight women are two to about four times as likely as normal-weight women to develop endometrial cancer (cancer of the lining of the uterus), and extremely obese women are about seven times as likely to develop the more common of the two main types of this cancer (7). The risk of endometrial cancer increases with increasing weight gain in adulthood, particularly among women who have never used menopausal hormone therapy (8).
- Esophageal adenocarcinoma: People who are overweight or obese are about twice as likely as normal-weight people to develop a type of esophageal cancer called esophageal adenocarcinoma, and people who are extremely obese are more than four times as likely (9).
- Gastric cardia cancer: People who are obese are nearly twice as likely as normal-weight people to develop cancer in the upper part of the stomach, that is, the part that is closest to the esophagus (10).
- Liver cancer: People who are overweight or obese are up to twice as likely as normal-weight people to develop liver cancer. The association between overweight/obesity and liver cancer is stronger in men than women (11, 12).
- Kidney cancer: People who are overweight or obese are nearly twice as likely as normal-weight people to develop renal cell cancer, the most common form of kidney cancer (13). The association of renal cell cancer with obesity is independent of its association with high blood pressure, a known risk factor for kidney cancer (14).
- Multiple myeloma: Compared with normal-weight individuals, overweight and obese individuals have a slight (10% to 20%) increase in the risk of developing multiple myeloma (15).
- Meningioma: The risk of this slow-growing brain tumor that arises in the membranes surrounding the brain and the spinal cord is increased by about 50% in people who are obese and about 20% in people who are overweight (16).
- Pancreatic cancer: People who are overweight or obese are about 1.5 times as likely to develop pancreatic cancer as normal-weight people (17).
- Colorectal cancer: People who are obese are slightly (about 30%) more likely to develop colorectal cancer than normal-weight people (18).A higher BMI is associated with increased risks of colon and rectal cancers in both men and in women, but the increases are higher in men than in women (18).
- Gallbladder cancer: Compared with normal-weight people, people who are overweight have a slight (about 20%) increase in risk of gallbladder cancer, and people who are obese have a 60% increase in risk of gallbladder cancer (19, 20). The risk increase is greater in women than men.
- Breast cancer: Many studies have shown that, in postmenopausal women, a higher BMI is associated with a modest increase in risk of breast cancer. For example, a 5-unit increase in BMI is associated with a 12% increase in risk (21). Among postmenopausal women, those who are obese have a 20% to 40% increase in risk of developing breast cancer compared with normal-weight women (22). The higher risks are seen mainly in women who have never used menopausal hormone therapy and for tumors that express hormone receptors. Obesity is also a risk factor for breast cancer in men (23).In premenopausal women, by contrast, overweight and obesity have been found to be associated with a 20% decreased risk of breast tumors that express hormone receptors (22).
- Ovarian cancer: Higher BMI is associated with a slight increase in the risk of ovarian cancer, particularly in women who have never used menopausal hormone therapy (24). For example, a 5-unit increase in BMI is associated with a 10% increase in risk among women who have never used menopausal hormone therapy (24).
- Thyroid cancer: Higher BMI (specifically, a 5-unit increase in BMI) is associated with a slight (10%) increase in the risk of thyroid cancer (25).
Medical Health Videos: “Symptoms Of Colon Cancer” (Mayo Clinic)
The team at Mayo Clinic prefer to see patients screened for colorectal cancer before they show symptoms.
Health Talk: “Colorectal Cancer” & Importance Of Screening (Mayo Clinic)
On the Mayo Clinic Radio program, Dr. John Kisiel, a Mayo Clinic gastroenterologist, discusses colorectal cancer and the importance of recommended screening tests.
This interview originally aired March 7, 2020. Disclaimer: Mayo Clinic has a financial interest in Exact Sciences.
Among cancers that affect men and women, colorectal cancer is the second leading cause of cancer deaths in the U.S., according to the Centers for Disease Control and Prevention. Most cases of colorectal cancer begin as small, noncancerous (benign) clumps of cells called polyps. Over time, some polyps become colon cancer. Because these polyps may be small and produce few, if any, symptoms, health care providers recommend regular screening tests to prevent colon cancer. These screenings identify and remove polyps before they become cancerous. March is Colorectal Cancer Awareness month, a time to educate the public about the importance of colorectal cancer screening.
Studies: Steep Increase In “Early-Onset Colorectal Cancer”; First Screening At Age 45 Suggested (JAMA)
From a JAMA Network Open online release (Jan 31, 2020):
 Steep incidence increases between 49 and 50 years of age are consistent with previously undetected colorectal cancers diagnosed via screening uptake at 50 years. These cancers are not reflected in observed rates of colorectal cancer in the SEER registries among individuals younger than 50 years. Hence, using observed incidence rates from 45 to 49 years of age alone to assess potential outcomes of earlier screening may underestimate cancer prevention benefits.
Steep incidence increases between 49 and 50 years of age are consistent with previously undetected colorectal cancers diagnosed via screening uptake at 50 years. These cancers are not reflected in observed rates of colorectal cancer in the SEER registries among individuals younger than 50 years. Hence, using observed incidence rates from 45 to 49 years of age alone to assess potential outcomes of earlier screening may underestimate cancer prevention benefits.
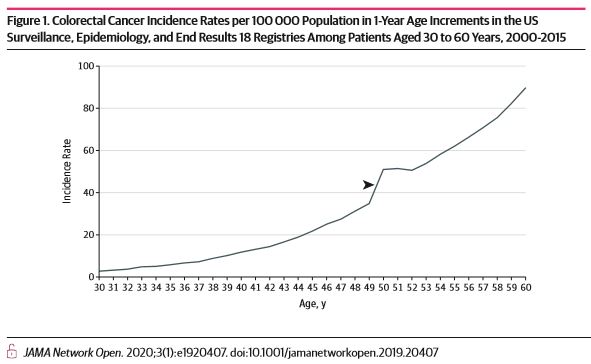
Early-onset colorectal cancer (EOCRC) incidence rates are increasing, and controversy exists regarding whether average-risk screening should begin at 45 or 50 years of age.1 In 2018, the American Cancer Society recommended that average-risk screening start at 45 years of age.2 Others recommend screening at 50 years of age, although the US Multi-Society Task Force on Colorectal Cancer recommends screening African American individuals at age 45 years of age owing to higher incidence, mortality, and earlier-onset disease.3–6 The American Cancer Society decision incorporated modeling studies that used updated incidence and mortality data encompassing time periods of increasing EOCRC incidence rates; modeling compared life-years gained by initiating screening at 45 vs 50 years.
Medical Case Studies: Identifying Metastatic Colorectal Cancer (Johns Hopkins Video)
A Chinese patient initially diagnosed with lung cancer traveled to Johns Hopkins for a second opinion. Noticing inconsistencies in the scans, experts at #JohnsHopkins brought her case to the gastrointestinal tumor board. Working as a team, these experts deduced her condition is actually metastatic colorectal cancer and recommended a new, more targeted treatment plan.