People who used a #salt substitute on their food had a lower risk of #stroke, #heartattack, and early death, compared with people who used regular salt, according to a large study published by The New England Journal of Medicine: https://t.co/JMsg9mnMwh #HarvardHealth pic.twitter.com/nBaYfYtlp7
— Harvard Health (@HarvardHealth) January 2, 2022
Tag Archives: New England Journal Of Medicine
2021 Heart Research: Top Findings Of Cardiologists
Coronary artery bypass graft (CABG) was supported as superior to fractional flow reserve (FFR)–guided percutaneous coronary intervention (PCI) for three-vessel coronary artery disease (CAD). PCI failed to meet noninferiority criteria at 1-year follow-up in a study comparing outcomes between FFR-guided PCI using contemporary stents and CABG. This adds to existing evidence showing superior outcomes with CABG in patients with the most-complex CAD.
The sodium–glucose transporter-2 (SGLT-2) inhibitor empagliflozin was found to be beneficial in heart failure with preserved ejection fraction. Empagliflozin is the first medication shown to improve outcomes in this population. It’s unknown if this is a class effect of all SGLT-2 inhibitors, but this could be a game changer.
Poor-quality carbohydrates were linked to cardiovascular mortality, around the world. Consumption of higher-glycemic-index carbohydrates was associated with higher rates of cardiovascular disease and mortality in countries all around the world. These data are particularly important because lower-income countries often have diets high in refined carbohydrates, which may worsen cardiovascular disparities.
New guidelines for managing valvular heart disease were released. These new guidelines add or elevate several recommendations for transcatheter therapy, and they lower thresholds for intervention in some conditions.
The editors of Circulation: Cardiovascular Quality and Outcomes addressed racial-ethnic disparities. The editors affirmed that structural racism is a public health crisis and that the scientific publishing community can play a role in addressing it.
Tricuspid annuloplasty for moderate regurgitation during mitral-valve surgery was of unclear benefit. Annuloplasty was associated with less progression of moderate tricuspid regurgitation but more pacemakers at 2 years. Unfortunately, this mixed outcome does not clearly inform the decision on performing annuloplasty at the time of surgery, and longer-term follow-up is needed.
Immediate angiography was not beneficial in out-of-hospital cardiac arrest without ST elevation. Patients with out-of-hospital cardiac arrest who did not have ST elevation on their initial ECG did not benefit from immediate angiography. Although a potential coronary culprit was identified in about 40% of patients, neurologic injury was by far the most frequent cause of death, negating any benefit from coronary revascularization.
Many statin side effects are related to the “nocebo” effect. A creative study enrolled 60 people with statin intolerance and gave them 12 randomly ordered 1-month treatment periods: 4 periods of no medication, 4 of placebo, and 4 of statin. Symptom intensity did not differ between placebo and statin periods and, interestingly, some even had more symptoms on placebo. This demonstrates that some cases of “statin intolerance” may be related to the “nocebo” effect.
Shorter duration of dual antiplatelet therapy following PCI/stent placement was found to be acceptable in patients with high bleeding risk. A large, randomized trial found that 1 month of dual antiplatelet therapy provided similar clinical outcomes and a lower bleeding risk than 3-to-6-month regimens for this challenging patient subset.
“De-escalation” of dual antiplatelet therapy for patients undergoing PCI for acute myocardial infarction (MI). This industry-funded study evaluated patients who had received 1 month of aspirin plus ticagrelor after acute MI and stent placement and “de-escalated” half to aspirin plus clopidogrel. At 1 year, there was significantly less bleeding in the de-escalation group and a nonsignificant trend toward fewer ischemic events as well.
PODCAST: ‘THE FUTURE OF DRUG PRICE TRANSPARENCY’
Interview with Dr. William Feldman on a new federal price-transparency rule and legal challenges to efforts to increase access to pricing information.
William Feldman is a physician and researcher in the Division of Pharmacoepidemiology and Pharmacoeconomics at Brigham and Women’s Hospital. Stephen Morrissey, the interviewer, is the Executive Managing Editor of the Journal.
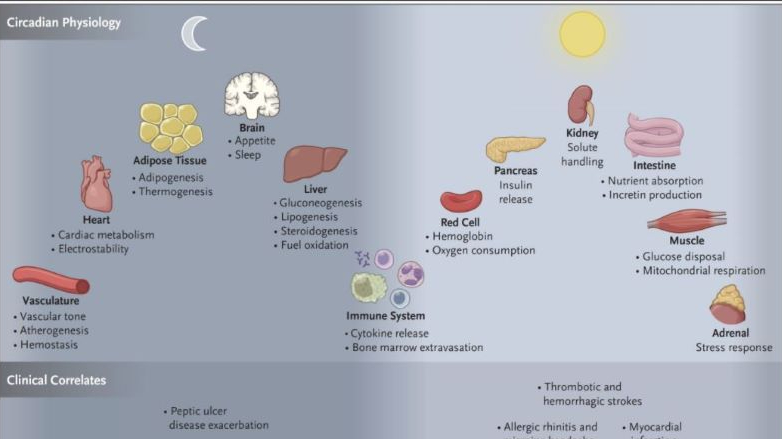
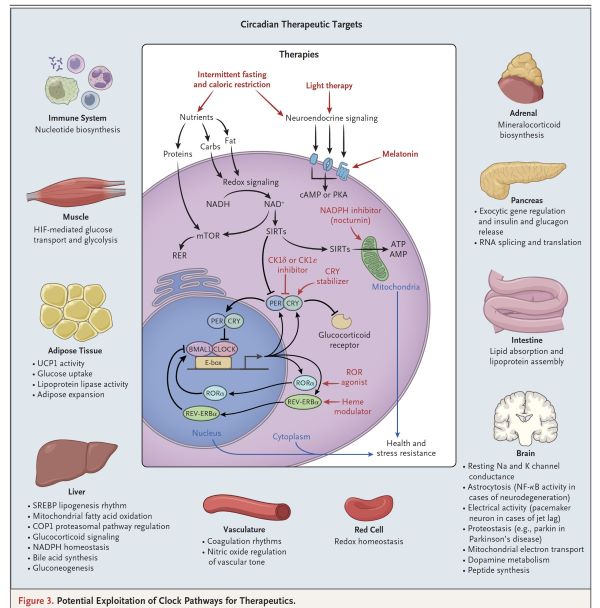
NEJM: Circadian Rhythms Importance In Medicine
Covid-19 Vaccines: ‘Frequently Asked Questions Answered’

How does each of the available Covid-19 vaccines work?
Once the vaccine is injected, the mRNA is taken up by the macrophages near the injection site and instructs those cells to make the spike protein. The spike protein then appears on the surface of the macrophages, inducing an immune response that mimics the way we fight off infections and protects us from natural infection with SARS-CoV-2. Enzymes in the body then degrade and dispose of the mRNA. No live virus is involved, and no genetic material enters the nucleus of the cells.
Although these are the first mRNA vaccines to be broadly tested and used in clinical practice, scientists have been working on mRNA vaccines for years. And despite this wonderful parody piece. opens in new tab saying that the technology is “obvious,” in fact the breakthrough insight that put the mRNA inside a lipid coating to prevent it from degrading is quite brilliant — and yes, this may be the first time the New England Journal of Medicine has referenced a piece in The Onion. (Last reviewed/updated on 11 Jan 2021)
How should early side effects be managed?
Analgesics and antipyretics such as acetaminophen or ibuprofen are effective in managing post-vaccine side effects including injection-site pain, myalgias, and fever. However, the CDC does not recommend prevaccine administration of these drugs, as they could theoretically blunt vaccine-induced antibody responses.
Because of the small risk of anaphylaxis, sites that administer the vaccines must have on hand strategies to evaluate and treat these potentially life-threatening reactions. The CDC has issued recommendations on how sites should prepare. opens in new tab. (Last reviewed/updated on 11 Jan 2021)
How long will the vaccines work? Are booster doses required?
Since the vaccines have been tested only since the summer of 2020, we do not have information about the durability of protection. Data from the phase 1 trial of the Moderna vaccine suggested that neutralizing antibodies persisted for nearly 4 months. opens in new tab, with titers declining slightly over time. Given the absence of information on how long the vaccines will be protective, there is currently no specific recommendation for booster doses. (Last reviewed/updated on 11 Jan 2021)
Do the vaccines prevent transmission of the virus to others?
Many commentaries on the results of the vaccine clinical trials cite a lack of information on asymptomatic infection as a limitation in our knowledge about the vaccines’ effectiveness. Indeed, this is a theoretical concern, since up to 40% of people who get infected with SARS-CoV-2 have no symptoms but may still transmit the virus to others.
Nonetheless, there are several good reasons to be optimistic about the vaccines’ effect on disease transmission. First, in the Moderna trial. opens in new tab, participants underwent nasopharyngeal swab PCR testing at baseline and testing at week 4, when they returned for their second dose. Among those who were negative at baseline and without symptoms, 39 (0.3%) in the placebo group and 15 (0.1%) in the mRNA-1273 group had nasopharyngeal swabs that were positive for SARS-CoV-2 by RT-PCR. These data suggest that even after one dose, the vaccine has a protective effect in preventing asymptomatic infection.
Second, findings from population-based studies now suggest that people without symptoms are less likely to transmit the virus to others. Third, it would be highly unlikely in biological terms for a vaccine to prevent disease and not also prevent infection. If there is an example of a vaccine in widespread clinical use that has this selective effect — prevents disease but not infection — I can’t think of one!
Until we know more, however, we should continue to emphasize to our patients that vaccination does not allow us to stop other important measures to prevent the spread of Covid-19. We need to continue social distancing, masking, avoiding crowded indoor settings, and regular hand washing. (Last reviewed/updated on 11 Jan 2021)
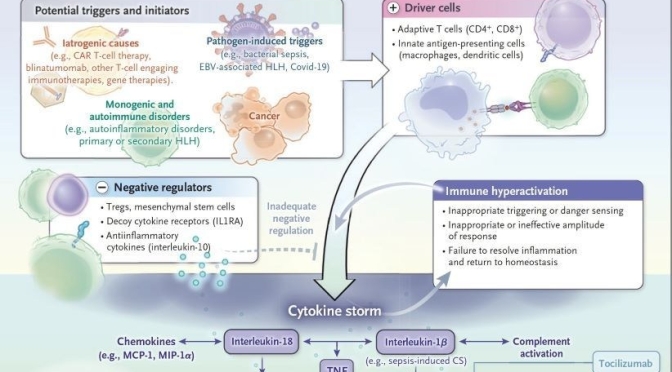
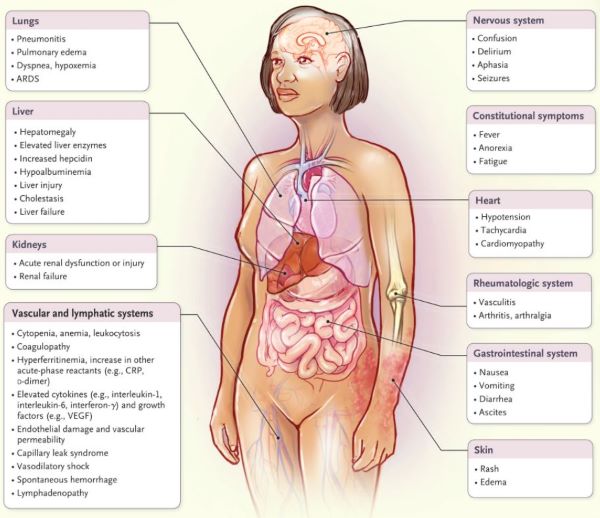
Medical Reviews: Covid-19 & ‘Cytokine Storm’ (NEJM)
Covid-19 Podcast: New Studies On Transmission

In this audio interview conducted on November 25, 2020, the editors look at new studies of disease transmission in closed environments and provide updates on convalescent plasma and hydroxychloroquine.
Aging Adults: ‘Learning About “End-Of-Life Care” From Grandpa’ (NEJM)
I described another option to Grandpa: he could voluntarily stop eating and drinking. He’d never considered this possibility (which reminded me again how one’s family members and clinicians contribute to inequities in end-of-life care). The option intrigued Grandpa, and during subsequent visits he reinforced his plan to pursue it. I insisted that he first move into my home. I wanted to ensure the quality of his care, knowing that I could enroll him in my health system’s hospice program. But I also wished to test his resolve, reasoning that his mind might change once his isolation ended.

For a month after he entered our home, his spirits were brighter, his gait steadier, and his appetite heartier. He joined my wife, two daughters, and me for dinner each night, typically preceded by a vodka martini that I had stirred for him — a daily pleasure he’d allowed himself for 80 years and had missed as a facility resident. He’d tell stories of the Navy, his career, and his family history and would regularly quip, “If you keep treating me this well, I might just stick around a while longer!”
But eventually he returned to his goal of hastening death. One night, he said he was ready to stop eating and drinking the next morning, but when morning came, he asked for his usual coffee and bagel. He confided that he was scared. When I asked of what, he replied, “It’s like trying to roller skate. I’m scared of starting. Though I know that once I do, I’ll probably roll.”
Winery Profile Podcast: The Urban Wine Company, London, ‘CHATEAU TOOTING’

Monocle’s Georgina Godwin heads to southwest London to visit The Urban Wine Company, that harvests its bounty from vines across the city.

The Urban Wine Company™ was born out of an idea a few years back. Neighbours Richard and Paul were relaxing underneath a vine enjoying a glass of wine that had been flown half-way across the world. Realising they were sat in an urban garden of Eden surrounded by grape vines, they asked the impossible…
“Would it be possible to make a wine made from London grapes?”

So, in September 2009 they set about harvesting grapes grown in gardens, allotments, behind supermarkets and even at the side of railways. They teamed up with winemaking experts to produce the very first batch of ‘Chateau Tooting’. Pleasantly surprised, if not a little amazed by its ‘Drinkability’ The Urban Wine Company™ was formed. Not only had a fantastic tasting wine been created using grapes grown in a city centre, something unique had also been born.
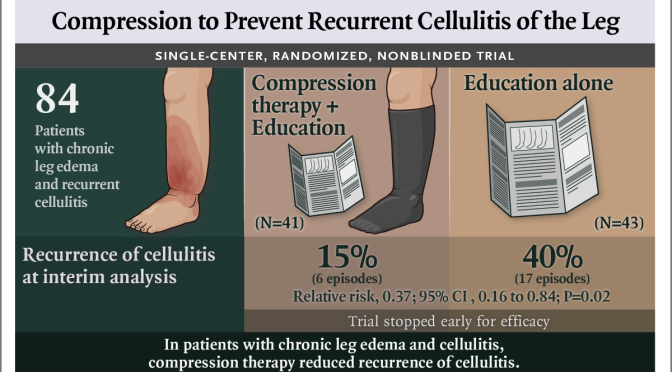
Health: “Compression Therapy” Reduces Chronic Cellulitis & Leg Edema
New England Journal of Medicine (Aug 13, 2020) – In this small, single-center, nonblinded trial involving patients with chronic edema of the leg and cellulitis, compression therapy resulted in a lower incidence of recurrence of cellulitis than conservative treatment.
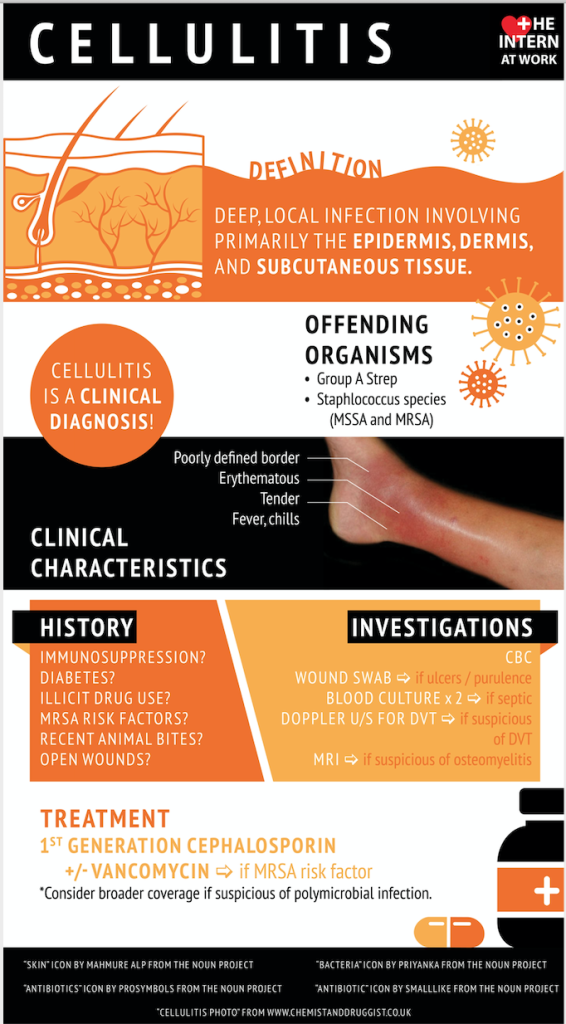
The researchers have conducted a single-center, randomized, nonblinded trial that aimed to find out an association between the compression therapy and controlled incidents of chronic edema of the leg and people with cellulitis that can be defined as an infection of the skin that involves subcutaneous tissues or the innermost layer of the skin. Cellulitis can be caused by trauma or scratching of other lesions due to animal or human bites that result in fever, extreme pain, and redness of the skin.