What you need to know
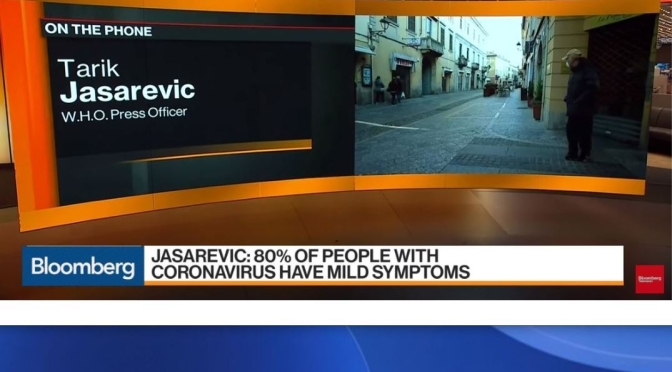
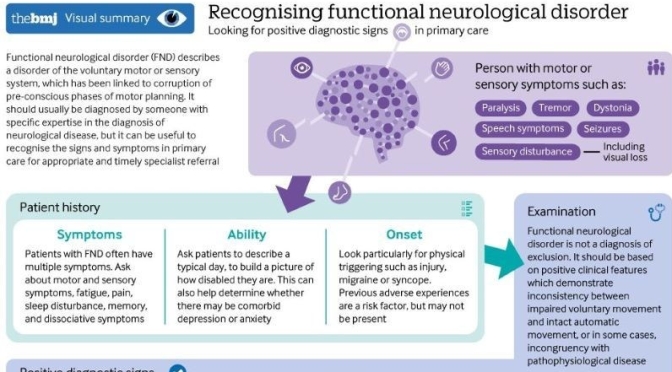
- Functional neurological disorder (FND) is associated with considerable distress and disability. The symptoms are not faked
- Diagnose FND positively on the basis of typical clinical features. It is not a diagnosis of exclusion
- FND can be diagnosed and treated in presence of comorbid, pathophysiologically defined disease
- Psychological stressors are important risk factors but are neither necessary nor sufficient for the diagnosis
Functional disorders are conditions whose origin arises primarily from a disorder of nervous system functioning rather than clearly identifiable pathophysiological disease—such as irritable bowel syndrome, fibromyalgia, and functional neurological disorder (FND)—they are the second commonest reason for new neurology consultations.1 FND is common in emergency settings,2 stroke,3 and rehabilitation services.4 It causes considerable physical disability and distress, and often places an economic burden both on patients and health services.5 Many clinicians have had little formal clinical education on the assessment and management of these disorders, and patients are often not offered potentially effective treatments.




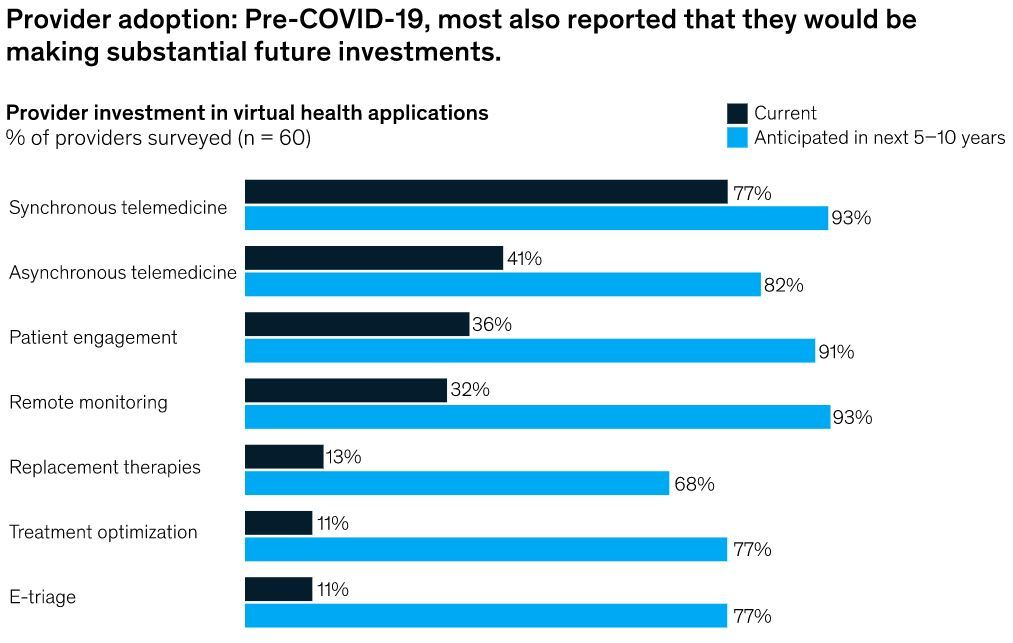


 For instance, more hospitals are remotely triaging and registering patients before they even arrive. Clinicians can consult with patients from their home via telemedicine to help determine how sick they are and if they need to come to the ER at all. From there, admissions are made with as little contact with staff or other patients as possible.
For instance, more hospitals are remotely triaging and registering patients before they even arrive. Clinicians can consult with patients from their home via telemedicine to help determine how sick they are and if they need to come to the ER at all. From there, admissions are made with as little contact with staff or other patients as possible.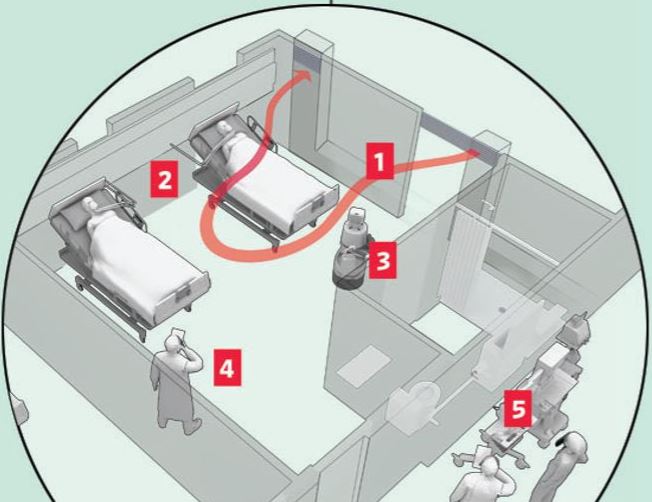
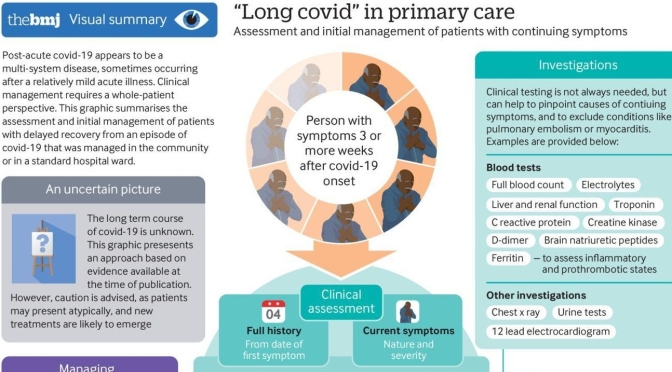
 With the potential for resurgences of the coronavirus, and some scientists warning about outbreaks of other infectious diseases, hospitals don’t want to be caught flat-footed again. So, more of them are turning to new protocols and new technology to overhaul standard operating procedure, from the time patients show up at an emergency room through admission, treatment and discharge.
With the potential for resurgences of the coronavirus, and some scientists warning about outbreaks of other infectious diseases, hospitals don’t want to be caught flat-footed again. So, more of them are turning to new protocols and new technology to overhaul standard operating procedure, from the time patients show up at an emergency room through admission, treatment and discharge.
 Doctors are delaying procedures and surgeries in order to save resources like hospital beds and ventilators for Covid-19 patients, and prevent the infection from spreading.
Doctors are delaying procedures and surgeries in order to save resources like hospital beds and ventilators for Covid-19 patients, and prevent the infection from spreading.
 Cardiovascular consults are way down. Is the threat of COVID-19 infection scaring people away from ED’s?
Cardiovascular consults are way down. Is the threat of COVID-19 infection scaring people away from ED’s?
 When a man returning from Wuhan, China in January 2020 exhibited symptoms of the novel coronavirus, public health officials in the Seattle area were already on alert.
When a man returning from Wuhan, China in January 2020 exhibited symptoms of the novel coronavirus, public health officials in the Seattle area were already on alert.