Tag Archives: Telemedicine
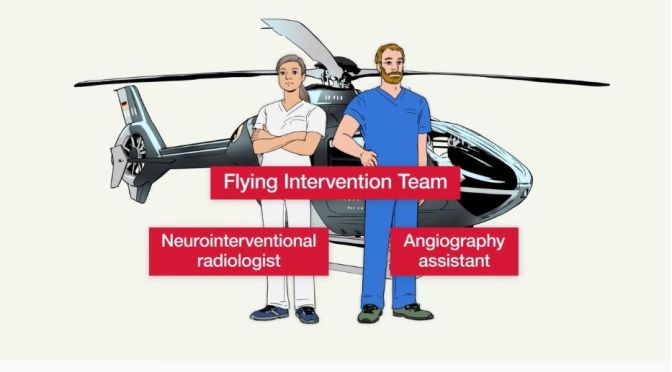
Emergency Medicine: Use Of Flying Intervention Teams In Ischemic Stroke
In a nonrandomized controlled intervention study published in JAMA, researchers in Germany assessed whether deployment of a flying interventional team, consisting of a neurointerventional radiologist and an angiography assistant, was associated with a shorter time to endovascular thrombectomy for patients in rural or intermediate population areas in Southeast Bavaria.
This video explains the study design. Click https://ja.ma/FIT for full details.
Technology: How AI Can Improve Health Care
AI has the power to transform health care. From more efficient diagnoses to safer treatments, it could remedy some of the ills suffered by patients. Film supported by @Maersk
Timeline: 00:00 – Can AI help heal the world? 00:45 – How can AI spot blindness? 04:01 – Protecting patients’ privacy 05:10 – How to share medical data safely 06:11 – Medical AI is rapidly expanding 08:02 – What do the sceptics say? 08.36 – Using AI for new medical devices 11:08 – What does the future hold for medical AI?
Health: Annual Physical Exams Are Going Virtual
Telemedicine: Growth Rate Peaked In April 2020, Stabilized During 2021
A year ago, we estimated that up to $250 billion of US healthcare spend could potentially be shifted to virtual or virtually enabled care. Approaching this potential level of virtual health is not a foregone conclusion. It would likely require sustained consumer and clinician adoption and accelerated redesign of care pathways to incorporate virtual modalities.
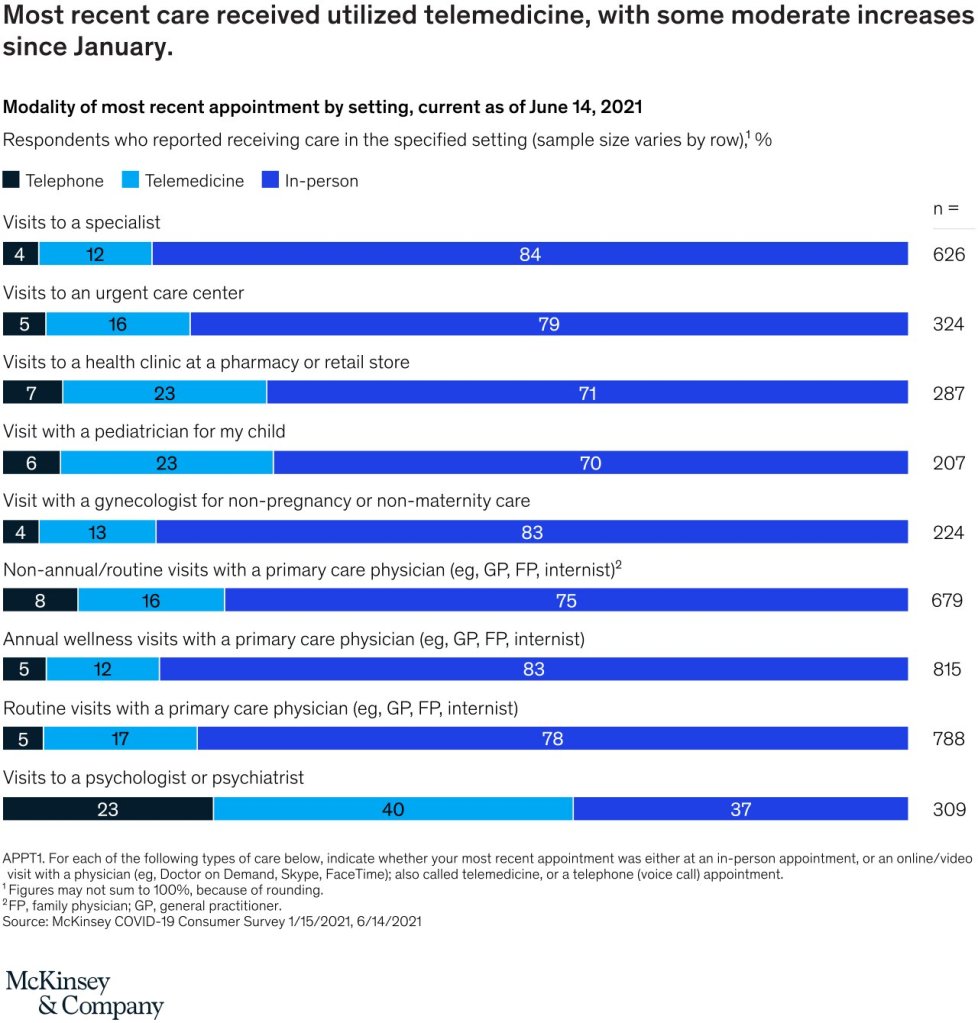
- Telehealth utilization has stabilized at levels 38X higher than before the pandemic. After an initial spike to more than 32 percent of office and outpatient visits occurring via telehealth in April 2020, utilization levels have largely stabilized, ranging from 13 to 17 percent across all specialties.2 This utilization reflects more than two-thirds of what we anticipated as visits that could be virtualized.3
- Similarly, consumer and provider attitudes toward telehealth have improved since the pre-COVID-19 era. Perceptions and usage have dropped slightly since the peak in spring 2020. Some barriers—such as perceptions of technology security—remain to be addressed to sustain consumer and provider virtual health adoption, and models are likely to evolve to optimize hybrid virtual and in-person care delivery.
- Some regulatory changes that facilitated expanded use of telehealth have been made permanent, for example, the Centers for Medicare & Medicaid Services’ expansion of reimbursable telehealth codes for the 2021 physician fee schedule. But uncertainty still exists as to the fate of other services that may lose their waiver status when the public health emergency ends.
- Investment in virtual care and digital health more broadly has skyrocketed, fueling further innovation, with 3X the level of venture capitalist digital health investment in 2020 than it had in 2017.4
- Virtual healthcare models and business models are evolving and proliferating, moving from purely “virtual urgent care” to a range of services enabling longitudinal virtual care, integration of telehealth with other virtual health solutions, and hybrid virtual/in-person care models, with the potential to improve consumer experience/convenience, access, outcomes, and affordability.
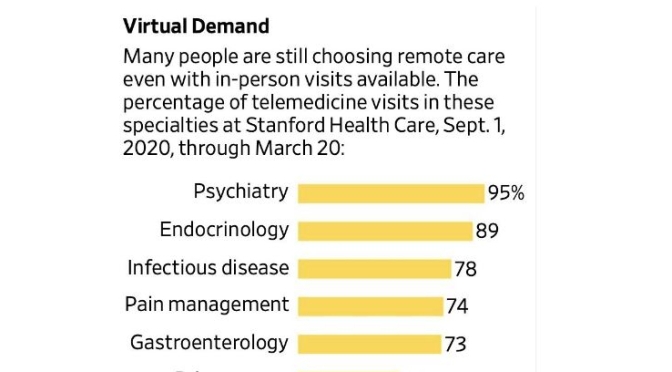
Telemedicine Survey: ‘High Demand’ Continues For Virtual Medical Visits
Infographic: Future Of Healthcare Is Digital
ANALYSIS: ‘THE EXPLOSIVE GROWTH OF TELEMEDICAL HEALTHCARE IN 2020’ (VIDEO)
Join CNET during CES 2021 for talks with three medical luminaries to discuss what we’ve gained — and need to fix — with telehealth over a turbulent pandemic year.
Telehealth: Older Adults’ “Telemedicine Visits” Rise From 4% To 26% In 2020
From 2019 to 2020, there was a substantial increase in the proportion of older adults who reported that their health care providers offered telehealth visits. In May 2019, 14% of older adults said that their health care providers offered telehealth visits, compared to 62% in June 2020.
Similarly, the percentage of older adults who had ever participated in a telehealth visit rose sharply from 4% in May 2019 to 30% in June 2020. Of those surveyed in 2020, 6% reported having a telehealth visit prior to March 2020, while 26% reported having a telehealth visit in the period from March to June 2020.

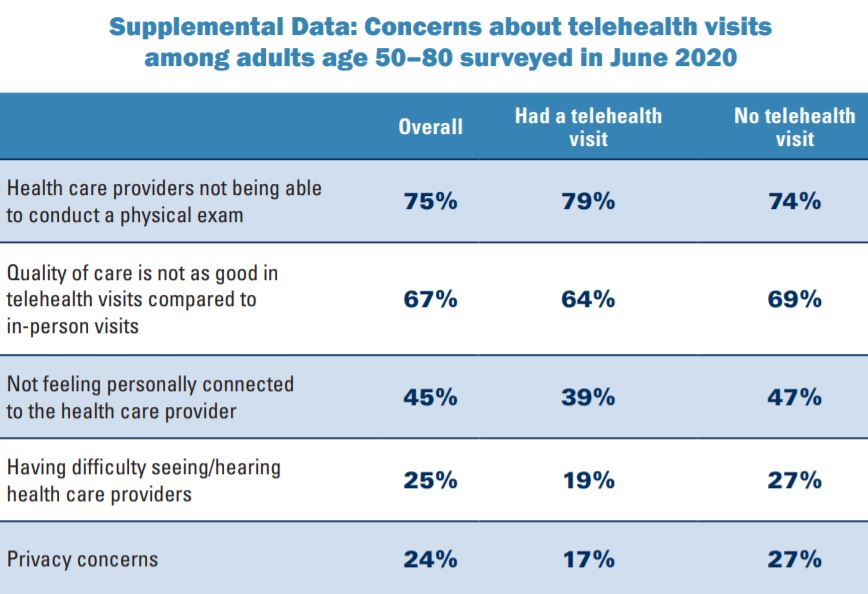
Over the past year, some concerns about telehealth visits decreased among adults age 50–80 whether or not they had a telehealth visit. Older adults’ concerns about privacy in telehealth visits decreased from 49% in May 2019 to 24% in June 2020, and concerns about having difficulty seeing or hearing health care providers in telehealth visits decreased from 39% in May 2019 to 25% in June 2020. Concerns about not feeling personally connected to the health care provider decreased slightly (49% to 45%).
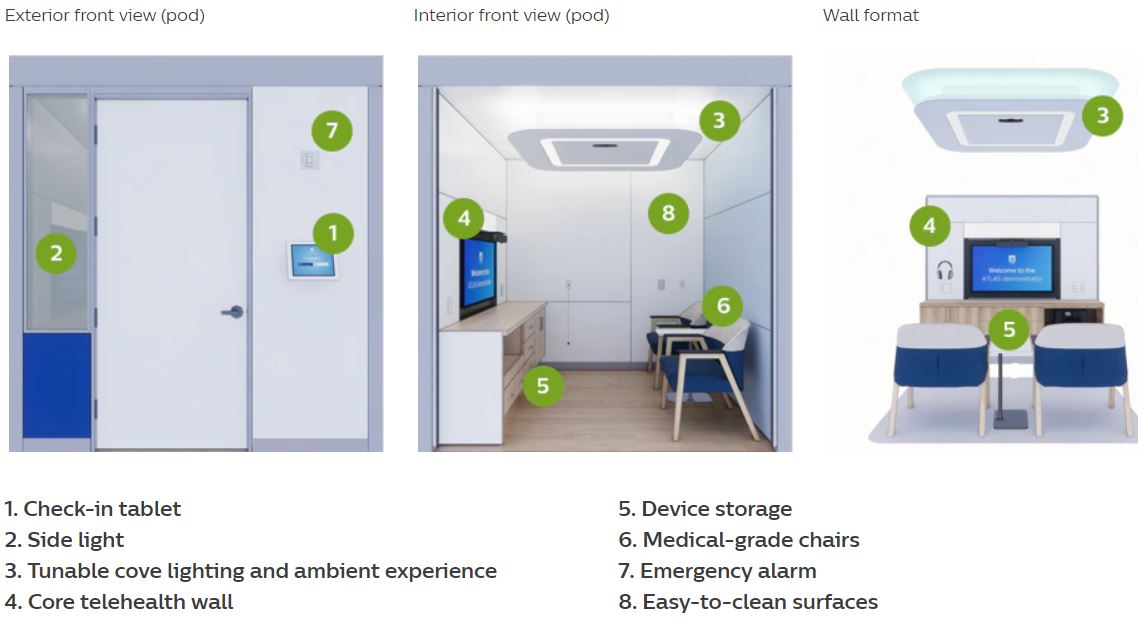
Telehealth Technology: Philips “Virtual Care Station” – “High Quality, Secure, Clinical-Grade”
Philips Virtual Care Station, inspired by the VA’s ATLAS program, is a community-based telehealth solution designed to expand access to high-quality care by connecting patients and providers remotely through a secure, clinical-grade environment.