Tag Archives: Health
Health: “Assessment Of Chest Pain” (BMJ Podcast)
 Chest pain is a common chief complaint. It may be caused by either benign or life-threatening aetiologies and is usually divided into cardiac and non-cardiac causes. James E. Brown, Professor and Chair, Wright State University Boonshoft School of Medicine, Kettering, Ohio, gives us an overview of assessing chest pain in the emergency setting.
Chest pain is a common chief complaint. It may be caused by either benign or life-threatening aetiologies and is usually divided into cardiac and non-cardiac causes. James E. Brown, Professor and Chair, Wright State University Boonshoft School of Medicine, Kettering, Ohio, gives us an overview of assessing chest pain in the emergency setting.
Sleeping Better: Positions And Environment Matter (Johns Hopkins Medicine)
From Johns Hopkins Medicine:
 “The sleep environment is something that can easily be fixed,” Salas says. By giving a little thought to positioning your body and bed, you might find your slumber is even sweeter.
“The sleep environment is something that can easily be fixed,” Salas says. By giving a little thought to positioning your body and bed, you might find your slumber is even sweeter.
For young, healthy people, sleep position is less important, Salas says. “But as you get older and have more medical issues, sleep position can become positive or negative.”
Consider these factors before you switch off the light:
- Back and neck pain: When it comes to alleviating pain, sleeping on your back is a mixed bag, Salas says. For people with neck pain, sleeping face up can sometimes make the pain worse. But many people find back sleep is helpful for alleviating low-back pain. If you have soreness in your spine, experiment with different positions and pillows to find what works for you.
- Snoring and sleep apnea: Obstructive sleep apnea causes the airways to collapse during sleep, leading to pauses in breathing. It often goes hand-in-hand with snoring. Positioning yourself on your side or stomach can help the airways stay open to reduce snoring and alleviate mild apnea, Salas says.
- Reflux and heartburn: If you suffer from heartburn, sleeping on your right side can make symptoms worse, Salas says. That’s true for people who have gastroesophageal reflux disease (GERD) and for people who have heartburn for other reasons, such as pregnant women. Flip to your left side to cool the burn.
- Appearance: If you sleep on your side or stomach, you’ve probably noticed creases on your face when you wake up. “Over time, that can lead to breakouts or cause chronic changes to the skin,” Salas says. “If you’re concerned about wrinkles, it’s another reason to sleep on your back.”
Don’t underestimate the importance of optimizing your bedroom to help you get a good night’s sleep. Salas adds:
- Clean sheets: Wash sheets frequently and vacuum the mattress to rid it of dust and dander that can cause allergies and impair your sleep.
- Close the blinds: Use curtains or blinds to keep the room dim at night. But open the curtains (or head outside) in the morning to reset your internal clock.
- Location matters: Position your bed so you aren’t facing distractions such as a desk stacked with work or a blinking light.
Infographic: “Physicians Adopting Telemedicine”
Diagnostics World (June 30, 2020): The shift from face-to-face patient visits to remote medical appointments is a worldwide phenomenon, but most especially in the U.S., finds a recent global survey conducted by the doctors-only social networking platform Sermo. Unsurprisingly, Zoom tops the list of most-mentioned technologies. About one-fifth of surveyed doctors say they expect to be using telehealth tools “significantly” more post-pandemic than before COVID-19 upended business as usual.

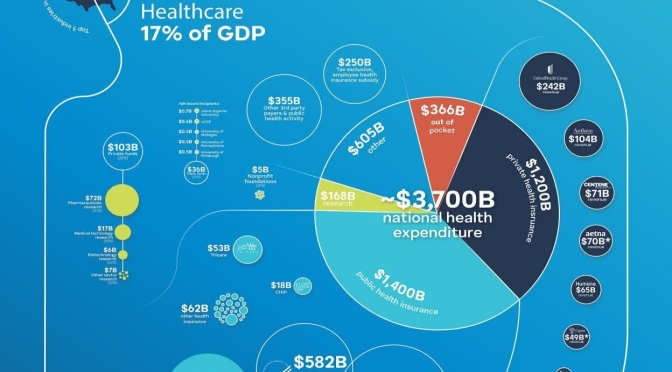
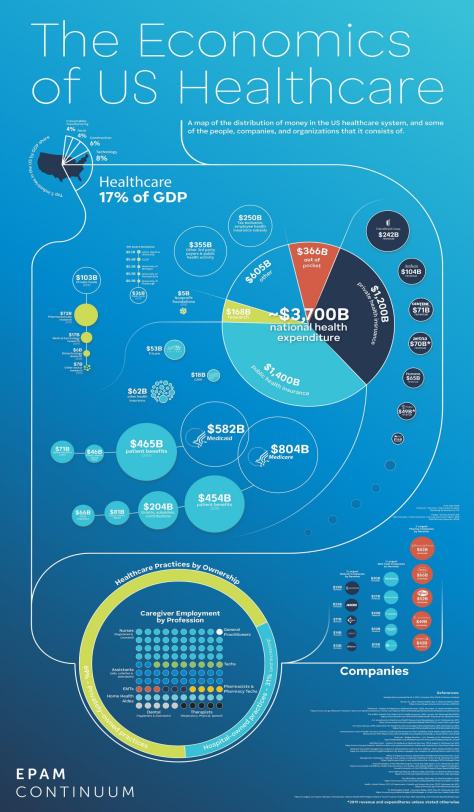
Infographic: “The Economics Of U.S. Healthcare” In 2020
Transportation: “How Covid-19 Is Changing Everyday Commuting”
Traveling on trains and buses means potential exposure to the coronavirus, so cities are racing to make their public transit systems safe. WSJ explores how things like sanitizing robots, working from home and expanded bike lanes are changing our commutes. Video/Illustration: Jaden Urbi and Zoë Soriano.
Infographic: “Advanced Prostate Cancer” In The U.S. Is Rising (2020)
Post-Covid Cities: “Fear In An Elevator” (CityLab)
As offices and businesses around the world slowly begin to reopen, the spotlight turns to one of the most traditionally uninteresting forms of transportation: the elevator. Modern cities are intrinsically reliant on these vertical transports which, in light of the global pandemic, can carry new risk factors.
World Health: “Covid-19 – The Second Wave” (Video)
The world now faces the threat of a second wave of coronavirus outbreaks. Zanny Minton Beddoes, The Economist’s editor-in-chief, and Slavea Chankova, our health-care correspondent, answer your questions.
Podcasts: The Many Difficulties Ahead For Restaurant Patio Dining
 Public health experts think Covid-19 risk is lower outside, and restaurateurs want to fill tables. It’s an easy solution—except for all the hard parts.
Public health experts think Covid-19 risk is lower outside, and restaurateurs want to fill tables. It’s an easy solution—except for all the hard parts.
“In a restaurant operating on the typical dining model of table service, I have not yet seen a case where outdoor seating would make up for the amount of lost indoor seating due to distancing,” Boor says. “Even the ones that come close require some pretty big assumptions about making that outdoor seating usable, like building something like wind screens and heating elements.” Few cities in the US have year-round pleasant weather in the evenings, whether that’s because of heat, humidity, cold, or rain. So restaurants trying to expand their borders are going to have to build some kind of nimbus of infrastructure to minimize the picnic-in-the-rain vibe. Of course, the more enclosed an outdoor space is, the more it is like an indoor space—with all the concomitant risks.