Scripps Research (April 21, 2023) – Chronic alcohol consumption may make people more sensitive to pain through two different molecular mechanisms—one driven by alcohol intake and one by alcohol withdrawal. That is one new conclusion by scientists at Scripps Research on the complex links between alcohol and pain.
The research, published in the British Journal of Pharmacology on April 12, 2023, also suggests potential new drug targets for treating alcohol-associated chronic pain and hypersensitivity.
“There is an urgent need to better understand the two-way street between chronic pain and alcohol dependence,” says senior author Marisa Roberto, PhD, the Schimmel Family Chair of Molecular Medicine, and a professor of neuroscience at Scripps Research. “Pain is both a widespread symptom in patients suffering from alcohol dependence, as well as a reason why people are driven to drink again.”
Alcohol use disorder (AUD), which encompasses the conditions commonly called alcohol abuse, alcohol dependence and alcohol addiction, affects 29.5 million people in the U.S. according to the 2021 National Survey on Drug Use and Health. Over time, AUD can trigger the development of numerous chronic diseases, including heart disease, stroke, liver disease and some cancers.











 Tension-type headaches can be either episodic or chronic. They are rarely disabling or associated with any significant autonomic phenomena, thus patients do not usually seek medical care and usually successfully self-treat. Unlike migraine, there is no significant nausea, no vomiting, and a lack of aggravation by routine physical activity.
Tension-type headaches can be either episodic or chronic. They are rarely disabling or associated with any significant autonomic phenomena, thus patients do not usually seek medical care and usually successfully self-treat. Unlike migraine, there is no significant nausea, no vomiting, and a lack of aggravation by routine physical activity.
 replicating a
replicating a 



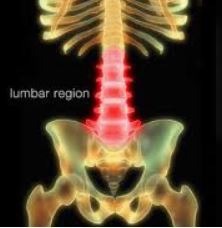 Sleep problems may decrease the likelihood of recovery from chronic low
Sleep problems may decrease the likelihood of recovery from chronic low  “Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?”
“Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?” Dr. Grace Dammann, medical director of the Pain Clinic at Laguna Honda Hospital, and seven of her colleagues talk about what does and does not work in the treatment of chronic pain. She talks as both a patient and a provider. There is also a discussion of various non-pharmacologic and complementary medicine modalities to treat pain.
Dr. Grace Dammann, medical director of the Pain Clinic at Laguna Honda Hospital, and seven of her colleagues talk about what does and does not work in the treatment of chronic pain. She talks as both a patient and a provider. There is also a discussion of various non-pharmacologic and complementary medicine modalities to treat pain.