Research reveals how irisin—a hormone produced during endurance exercise—works in multiple ways to protect brain health and prevent Alzheimer’s and dementia in mammalian models https://t.co/WExA9ZUVZN via @HarvardMagazine pic.twitter.com/WnLw3iWDPe
— Harvard Medical School (@harvardmed) December 22, 2021
Tag Archives: Health Benefits of Exercise
Exercise: The Evolution Of Human Physical Activity
Human physical activities differ significantly from other species. How, when and why did these capabilities evolve? What adaptations underlie them? And how did the evolution of human physical activity affect other key human characteristics that have advanced our species?
Herman Pontzer explores the evolution of human metabolism and its role in our evolution and health. From an evolutionary perspective, life is a game of turning energy into offspring. The strategies that species use to acquire energy, in the form of food, and allocate energy to the essential tasks of growth, maintenance, movement, and reproduction, are incredibly diverse and reflect the ecological pressures and opportunities encountered. There is a deep evolutionary history of the human metabolic strategy and our divergence from other apes.
Timeline: 00:00 – Start 01:38 – The Evolution of Human Metabolism
More from: CARTA: The Evolution of Human Physical Activity (https://www.uctv.tv/carta-physical-ac…)
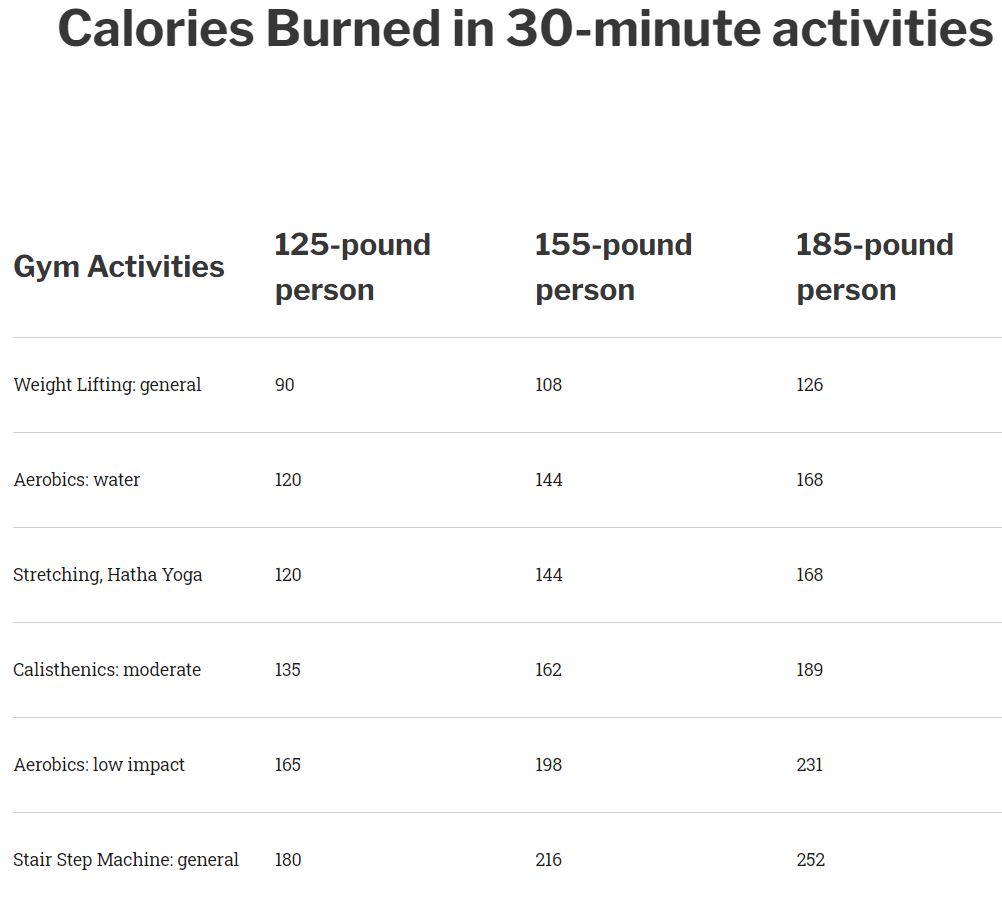
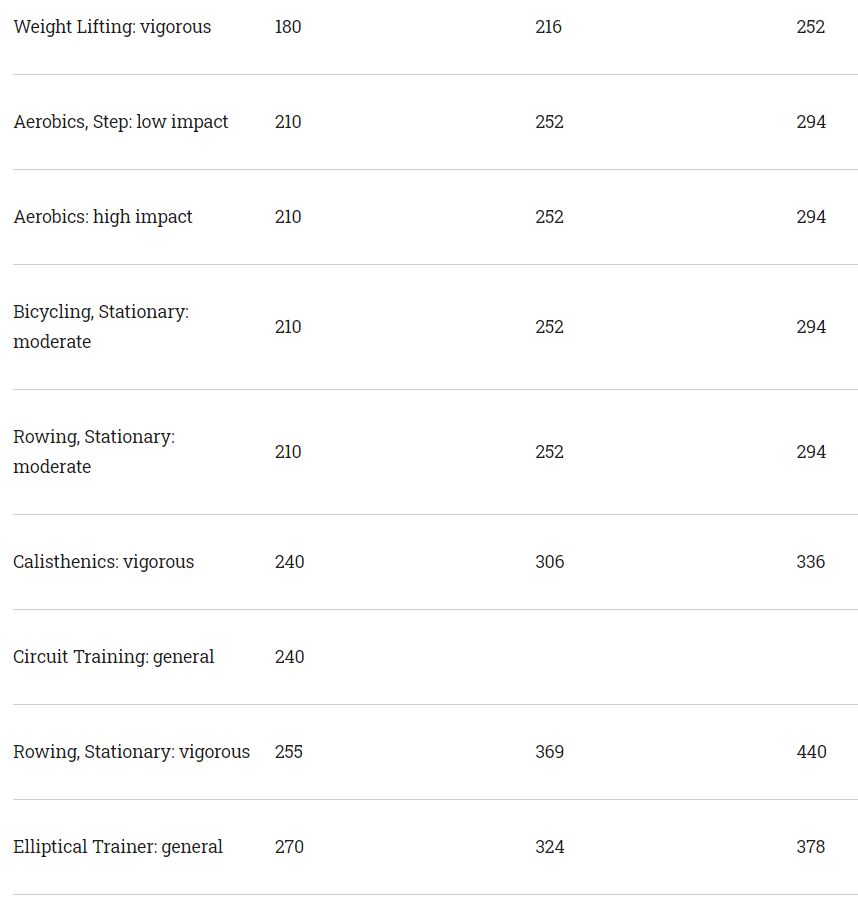
Charts: Calories Burned In 30-Minutes Of Exercise

Research: Importance Of Exercise & Movement For Brain Function & Health


But the connection between movement and the brain goes deeper than you might think. A revolutionary new understanding of the mind-body connection is revealing how our thoughts and emotions don’t just happen inside our heads, and that the way we move has a profound influence on how our minds operate. This opens up the possibility of using our bodies as tools to change the way we think and feel.
Evidence is starting to stack up that this is indeed the case, and it isn’t all about doing more exercise. In my new book, Move! The new science of body over mind, I explore emerging research in evolutionary biology, physiology, neuroscience and cell biology to find out which body movements affect the mind and why.
Whatever it is that you want from your mind – more creativity, improved resilience or higher self-esteem – the evidence shows that there is a way of moving the body that can help. Here is my pick of the best ways to use your body to achieve a healthier, better-functioning mind.
Exercise: Benefits Of HIIT (High-Intensity Interval Training) – Mayo Clinic
Mayo Clinic Division of Preventive Cardiology will be preparing a series of recordings focusing on Cardiovascular Disease states. This is the Exercise Series and this particular one focuses on HIIT and its benefits. Results in physiological adaptations linked to improved health (even with a very small volume of exercise).
Health: Three Exercise Benefits For The Brain
Memory

Many studies suggest that exercise can help protect our memory as we age. This is because exercise has been shown to prevent the loss of total brain volume (which can lead to lower cognitive function), as well as preventing shrinkage in specific brain regions associated with memory. For example, one magnetic resonance imaging (MRI) scan study revealed that in older adults, six months of exercise training increases brain volume.
Another study showed that shrinkage of the hippocampus (a brain region essential for learning and memory) in older people can be reversed by regular walking. This change was accompanied by improved memory function and an increase of the protein brain-derived neutropic factor (BDNF) in the bloodstream.
Blood vessels
The brain is highly dependent on blood flow, receiving approximately 15% of the body’s entire supply – despite being only 2-3% of our body’s total mass. This is because our nervous tissues need a constant supply of oxygen to function and survive. When neurons become more active, blood flow in the region where these neurons are located increases to meet demand. As such, maintaining a healthy brain depends on maintaining a healthy network of blood vessels.
Regular exercise increases the growth of new blood vessels in the brain regions where neurogenesis occurs, providing the increased blood supply that supports the development of these new neurons. Exercise also improves the health and function of existing blood vessels, ensuring that brain tissue consistently receives adequate blood supply to meet its needs and preserve its function.
Inflammation
Recently, a growing body of research has centred on microglia, which are the resident immune cells of the brain. Their main function is to constantly check the brain for potential threats from microbes or dying or damaged cells, and to clear any damage they find.
With age, normal immune function declines and chronic, low-level inflammation occurs in body organs, including the brain, where it increases risk of neurodegenerative disease, such as Alzheimer’s disease. As we age, microglia become less efficient at clearing damage, and less able to prevent disease and inflammation. This means neuroinflammation can progress, impairing brain functions – including memory.
Podcast Interviews: “Exercise Is Medicine” Author Judy Foreman
 Health journalist Judy Foreman talks about her new book Exercise Is Medicine: How Physical Activity Boosts Health and Slows Aging
Health journalist Judy Foreman talks about her new book Exercise Is Medicine: How Physical Activity Boosts Health and Slows Aging
 This is Scientific American’s Science Talk, posted on April 24th, 2020. I’m Steve Mirsky. And under our current, often locked-down situation, it’s still really important to try to get some exercise. Judy Foreman is the author of the new book Exercise is Medicine: How Physical Activity Boosts Health and Slows Aging. She’s a former nationally syndicated health columnist for the Boston Globe, LA times, Baltimore Sun and other places, and an author for the Oxford University Press.
This is Scientific American’s Science Talk, posted on April 24th, 2020. I’m Steve Mirsky. And under our current, often locked-down situation, it’s still really important to try to get some exercise. Judy Foreman is the author of the new book Exercise is Medicine: How Physical Activity Boosts Health and Slows Aging. She’s a former nationally syndicated health columnist for the Boston Globe, LA times, Baltimore Sun and other places, and an author for the Oxford University Press.
Judy Foreman is the author of “A Nation in Pain” (2014), “The Global Pain Crisis” (2017), and “Exercise is Medicine,” (2020), all published by Oxford University Press, and was a staff writer at The Boston Globe for 22 years and the health columnist for many of these years. Her column was syndicated in national and international outlets including the Los Angeles Times, Dallas Morning News, Baltimore Sun and others.
She graduated Phi Beta Kappa from Wellesley College and has a Master’s from the Harvard Graduate School of Education. She was a Lecturer on Medicine at Harvard Medical School, a Fellow in Medical Ethics at Harvard Medical School and a Knight Science Journalism Fellow at the Massachusetts Institute of Technology. She spent six months as a guest reporter for The Times of London. She was also a Senior Fellow at the Schuster Institute for Investigative Journalism at Brandeis University. She was also host of a live, weekly call-in radio show on Healthtalk.com.
Judy has won more than 50 journalism awards, including a 1998 George Foster Peabody award for co-writing a video documentary about a young woman dying of breast cancer and the 2015 Science in Society award from the National Association of Science Writers.
Study: Middle-Aged Knees With Meniscal Tears – No Benefits To Surgery Over Exercise Therapy (BMJ)

Conclusion: The study was inconclusive with respect to potential differences in progression of individual radiographic features after surgical and non-surgical treatment for degenerative meniscal tear. Further, we found no strong evidence in support of differences in development of incident radiographic knee osteoarthritis or patient-reported outcomes between exercise therapy and arthroscopic partial meniscectomy.
Objective: To evaluate progression of individual radiographic features 5 years following exercise therapy or arthroscopic partial meniscectomy as treatment for degenerative meniscal tear.
Design: Randomized controlled trial including 140 adults, aged 35-60 years, with a magnetic resonance image verified degenerative meniscal tear, and 96% without definite radiographic knee osteoarthritis. Participants were randomized to either 12-weeks of supervised exercise therapy or arthroscopic partial meniscectomy. The primary outcome was between-group difference in progression of tibiofemoral joint space narrowing and marginal osteophytes at 5 years, assessed semi-quantitatively by the OARSI atlas. Secondary outcomes included incidence of radiographic knee osteoarthritis and symptomatic knee osteoarthritis, medial tibiofemoral fixed joint space width (quantitatively assessed), and patient-reported outcome measures. Statistical analyses were performed using a full analysis set. Per protocol and as treated analysis were also performed.
Results: The risk ratios (95% CI) for progression of semi-quantitatively assessed joint space narrowing and medial and lateral osteophytes for the surgery group were 0.89 (0.55-1.44), 1.15 (0.79-1.68) and 0.77 (0.42-1.42), respectively, compared to the exercise therapy group. In secondary outcomes (full-set analysis) no statistically significant between-group differences were found.
Health & Fitness: “What Is Exercise Physiology?” (Penn Medicine Video)
Exercise physiologists are healthcare professionals that work with patients who are deconditioned or have a variety of different health complications. They work with pulmonary and cardiac patients, as well as competitive athletes with a wide range of fitness issues.
Penn Medicine’s Christopher J. Kusmiesz, MS describes his role as “assessing a patient’s fitness level and providing recommendations and guidance so they can improve and reach their health and fitness goals.”
Exercise physiologists at Penn uses patient test results, recommendations from their cardiologist and the patient’s own goals to create an exercise program that is unique to each patient.
Health Talk: “Exercise And The Heart” (Mayo Clinic)
On the Mayo Clinic Radio program, Dr. Todd Miller, a Mayo Clinic cardiologist, explains how exercise affects the heart. This interview originally aired Feb. 22, 2020. Learn more about exercise and the heart: https://www.mayoclinic.org/healthy-li…