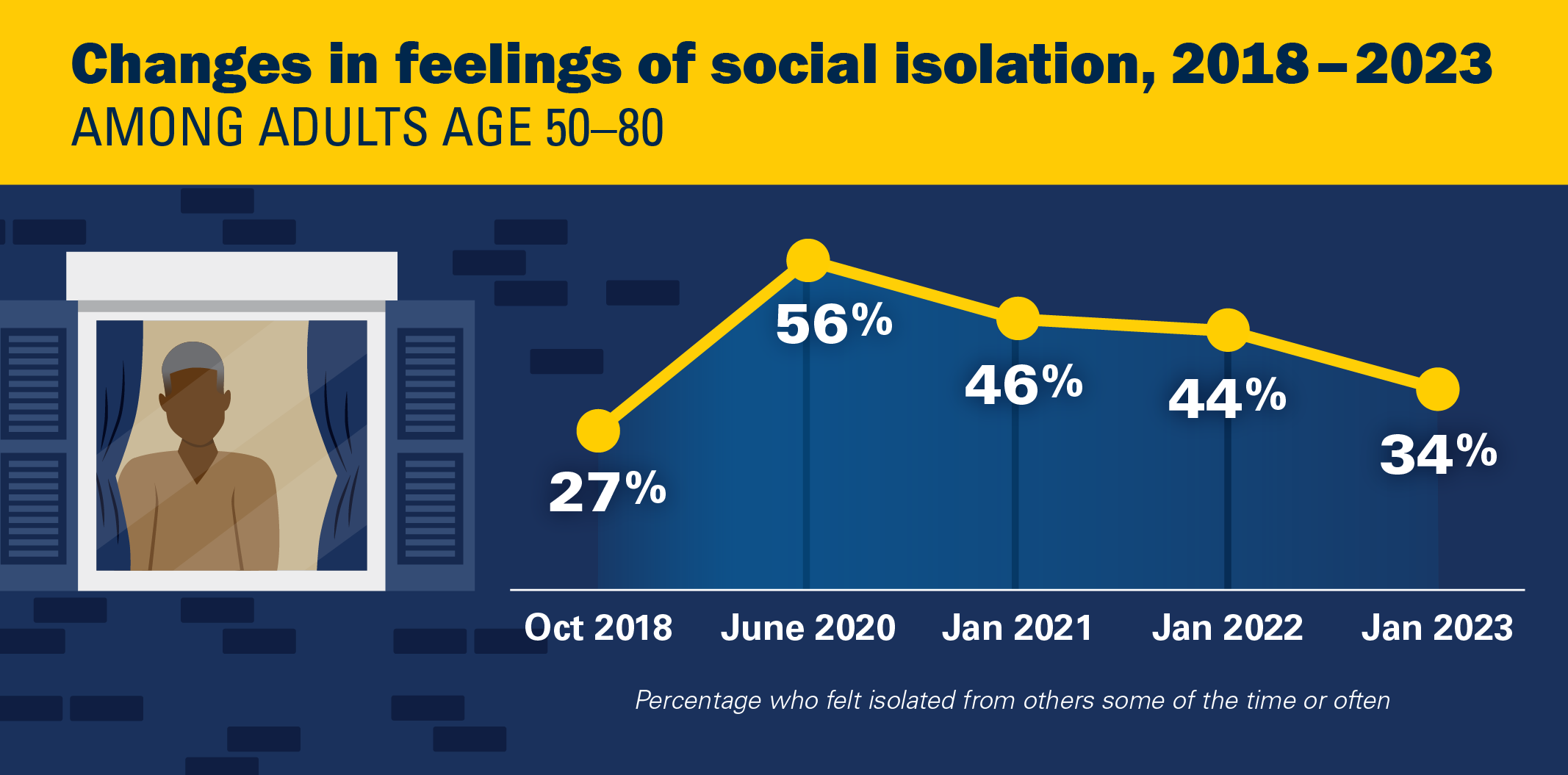
In 2023, one in three adults age 50–80 (34%) reported feeling isolated from others (29% some of the time, 5% often) in the past year. This represents a marked decline compared with the 56% (43% some of the time, 13% often) who felt isolated in 2020, but a greater proportion than the 27% (22% some of the time, 5% often) who reported feeling isolated in 2018.

National Poll On Healthy Aging (March 2023) – More than one in three older adults (37%) reported feeling a lack of companionship (29% some of the time, 8% often) in the past year, compared with 41% (32% some of the time, 9% often) in 2020, and 34% (26% some of the time, 8% often) in 2018.
One in three older adults (33%) reported infrequent contact (once a week or less) with people from outside their home in 2023 (14% once a week, 10% every 2–3 weeks, 9% once a month or less). This rate of infrequent contact was significantly less than the 46% reported in 2020 (19% once a week, 11% every 2–3 weeks, 16% once a month or less), but higher than the 28% reported in 2018 (15% once a week, 7% every 2–3 weeks, 6% once a month or less).


















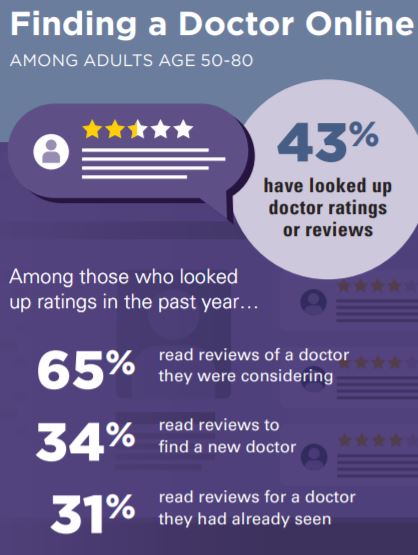 Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago.
Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago. Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a
Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a