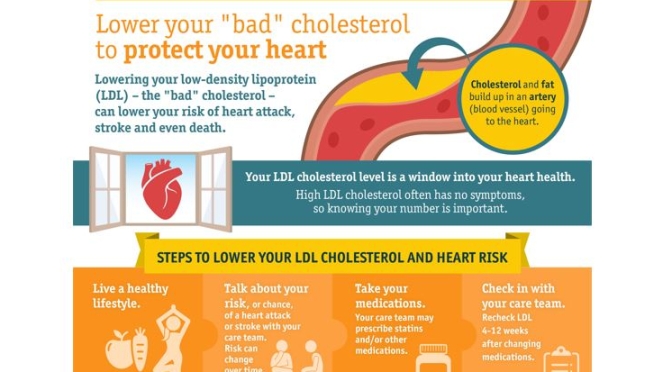
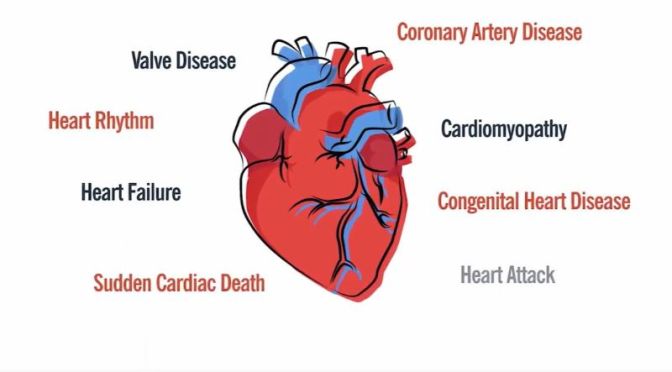
Influenza-related stress on your body can launch a negative chain of events that builds toward a heart attack. This video shares how getting a seasonal flu shot can significantly lower your risk of having a heart attack or cardiac arrest, especially if you’re in a high-risk group.
Chapters: 0:00 Can flu shots lower risk of heart attacks? 0:37 How does the flu shot lower risk of heart attacks? 1:08 Who is most at risk of having a flu related heart attack? 1:30 Why else should you get a flu shot?