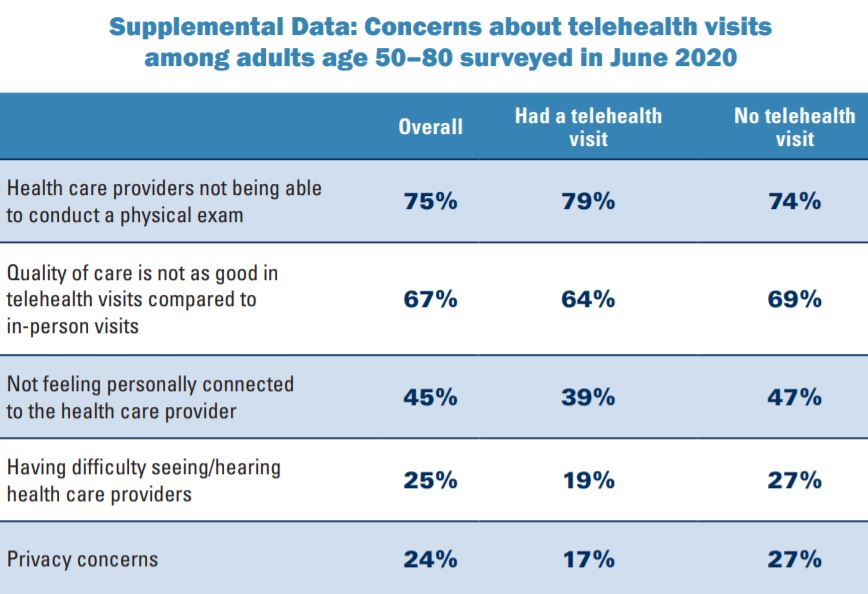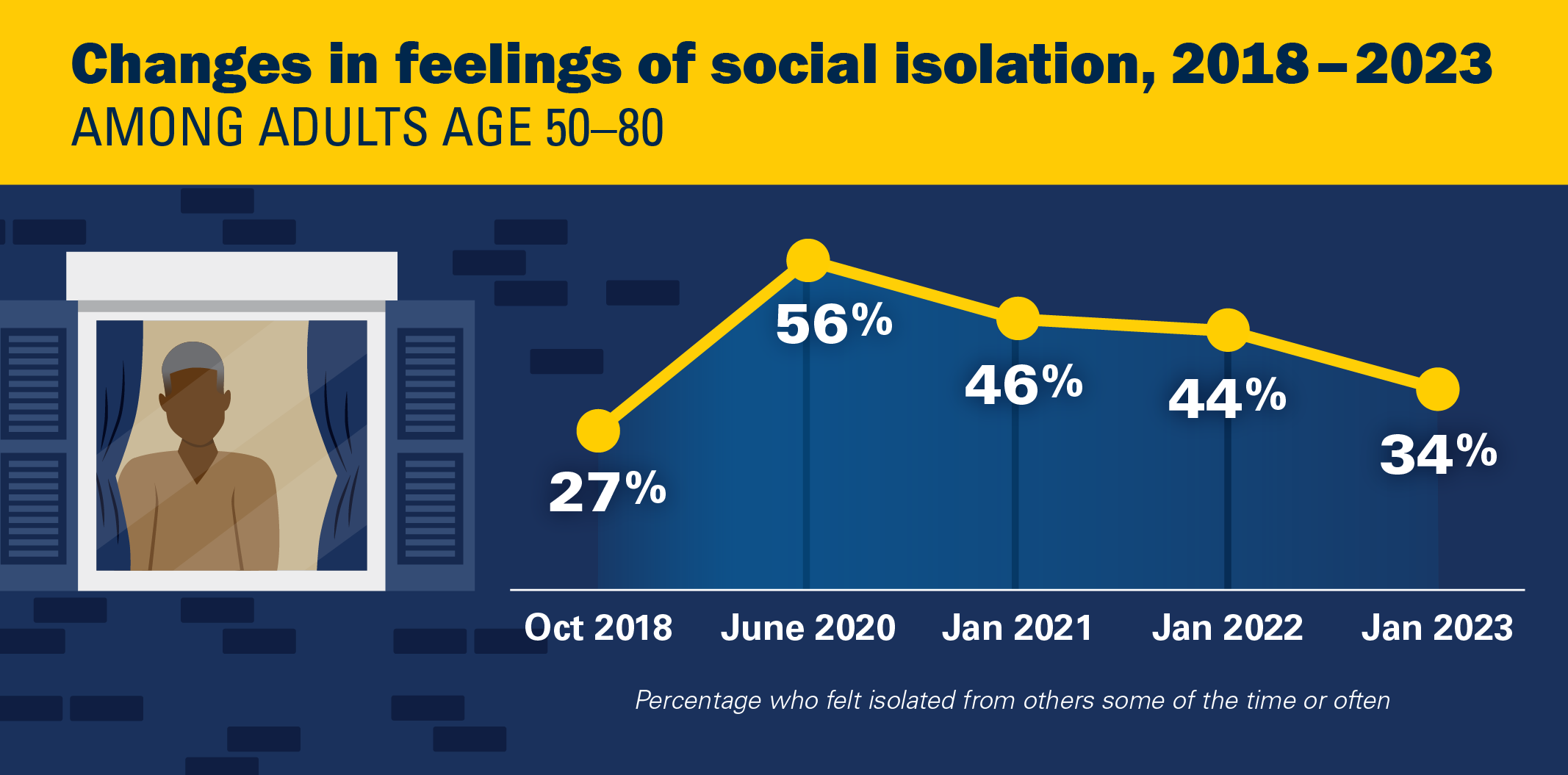
In 2023, one in three adults age 50–80 (34%) reported feeling isolated from others (29% some of the time, 5% often) in the past year. This represents a marked decline compared with the 56% (43% some of the time, 13% often) who felt isolated in 2020, but a greater proportion than the 27% (22% some of the time, 5% often) who reported feeling isolated in 2018.

National Poll On Healthy Aging (March 2023) – More than one in three older adults (37%) reported feeling a lack of companionship (29% some of the time, 8% often) in the past year, compared with 41% (32% some of the time, 9% often) in 2020, and 34% (26% some of the time, 8% often) in 2018.
One in three older adults (33%) reported infrequent contact (once a week or less) with people from outside their home in 2023 (14% once a week, 10% every 2–3 weeks, 9% once a month or less). This rate of infrequent contact was significantly less than the 46% reported in 2020 (19% once a week, 11% every 2–3 weeks, 16% once a month or less), but higher than the 28% reported in 2018 (15% once a week, 7% every 2–3 weeks, 6% once a month or less).