




The heart is a hero. It works relentlessly to deliver oxygen and nutrients to the body. But just like all heroes, sometimes it gets tired, and can’t do its job as well. This is called heart failure – the inability for the heart to pump enough blood and oxygen to the lungs and rest of the body. In this video, Northwestern Medicine cardiologists Clyde W. Yancy, MD, MSc and Jane E. Wilcox, MD, MSc explain what heart failure is and the integrated and collaborative approach used to diagnose, stage and treat heart failure at Northwestern Medicine. For more information, visit http://heart.nm.org
Mayo Clinic Division of Preventive Cardiology will be preparing a series of recordings focusing on Cardiovascular Disease states. This is the Exercise Series and this particular one focuses on HIIT and its benefits. Results in physiological adaptations linked to improved health (even with a very small volume of exercise).
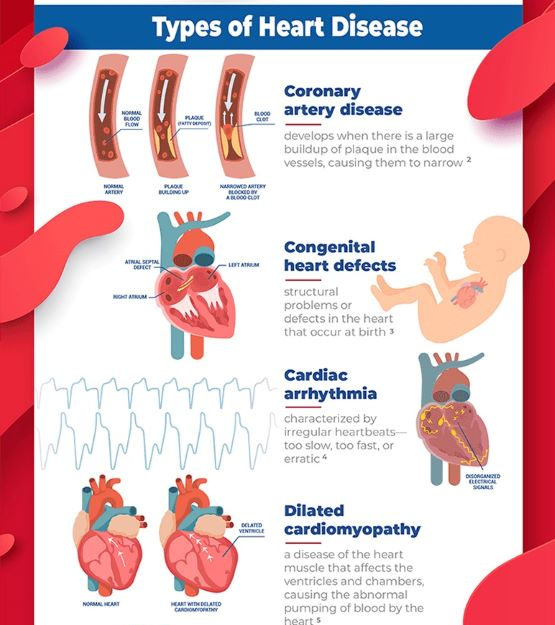
The heart is a muscle and it’s main job is to pump blood but certain things can cause that muscle to fail. There are genetic reasons, there are reasons related to valve disease, and there’s a viral infection that affects the heart called myocarditis.
The most common cause of heart failure is a heart attack. Fatty plaque builds up in the blood vessel that supplies the heart itself and unless that blood vessel is opened up immediately that muscle will die. The rest of the muscle that’s not dead anymore has to do extra to keep on pumping the blood and overtime it cannot keep and that’s when heart failure develops.
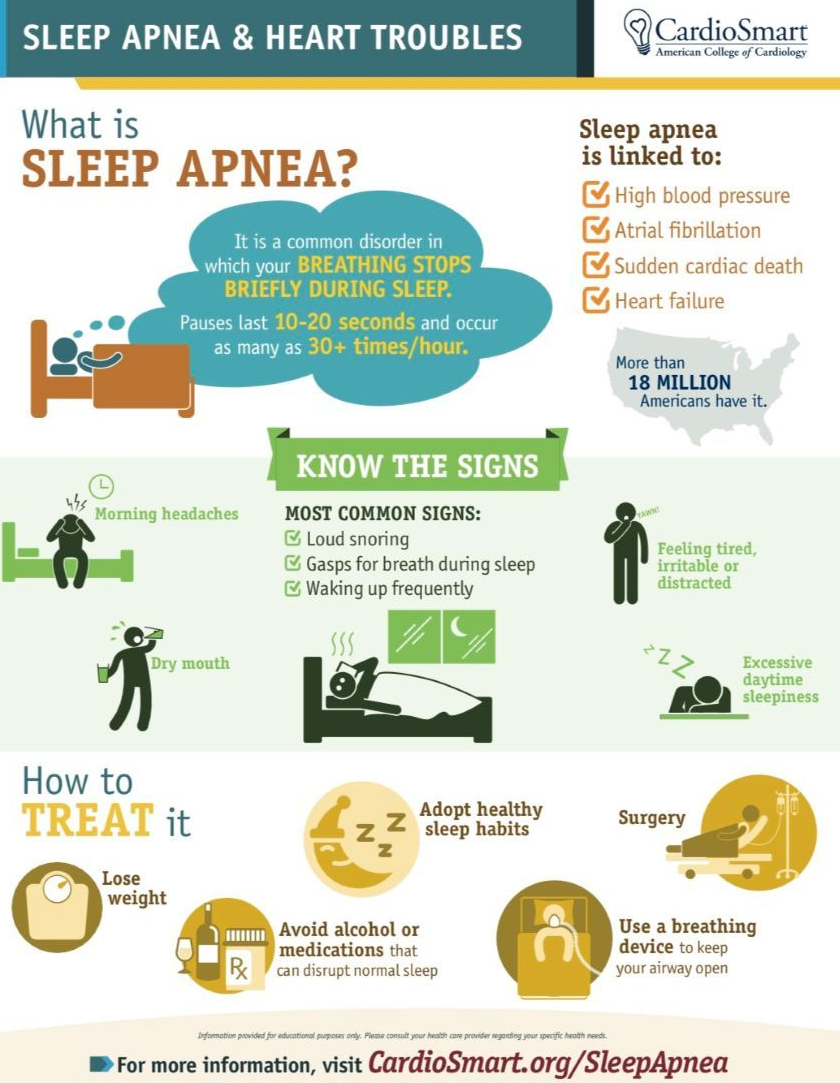

Hospitals across the U.S. are experiencing an influx of COVID-19 patients, but clinicians are reportedly seeing fewer patients going to the emergency room for heart attack or stroke.
Experts worry that patients who need critical care are delaying their treatment over COVID-19 concerns.
To encourage patients to pay close attention to their symptoms and call 9-1-1 immediately if they believe they are having a heart attack or stroke, ACC’s CardioSmart team developed the Coronavirus and Your Heart Infographic.
The infographic urges patients not to ignore symptoms, especially if they have a heart condition, and reassures them that hospitals have safety measures to protect patients from infection with the novel coronavirus.
From a “Circulation: Heart Failure” Journal study (Feb 25, 2020):
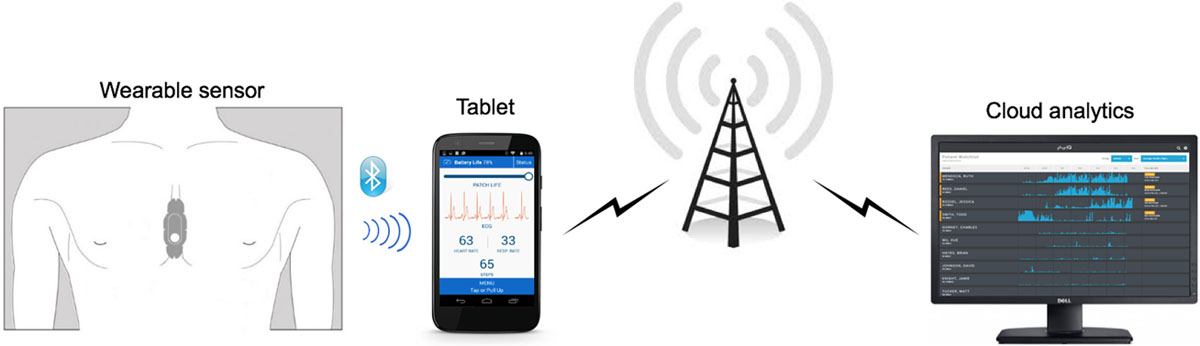
 The study shows that wearable sensors coupled with machine learning analytics have predictive accuracy comparable to implanted devices.
The study shows that wearable sensors coupled with machine learning analytics have predictive accuracy comparable to implanted devices.
We demonstrate that machine learning analytics using data from a wearable sensor can accurately predict hospitalization for heart failure exacerbation…at a median time of 6.5 days before the admission.
Heart failure (HF) is a major public health problem affecting >23 million patients worldwide. Hospitalization costs for HF represent 80% of costs attributed to HF care. Thus, accurate and timely detection of worsening HF could allow for interventions aimed at reducing the risk of HF admission.
Several such approaches have been tested. Tracking of daily weight, as recommended by current HF guidelines, did not lead to reduction of the risk of HF hospitalization, most likely because the weight gain is a contemporaneous or lagging indicator rather than a leading event. Interventions based on intrathoracic impedance monitoring also did not result in reduction of readmission risk. The results suggest that physiological parameters other than weight or intrathoracic impedance in isolation may be needed to detect HF decompensation in a timely manner. In fact, 28% reduction of rehospitalization rates has been shown with interventions based on pulmonary artery hemodynamic monitoring. More recently, in the MultiSENSE study (Multisensor Chronic Evaluation in Ambulatory HF Patients), an algorithm based on physiological data from sensors in the implantable cardiac resynchronization therapy defibrillators, was shown to have 70% sensitivity in predicting the risk of HF hospitalization or outpatient visit with intravenous therapies for worsening of HF.
From a News-Medical.net online release:
 “Patients can go home after a shorter length of stay in the hospital without increased risk of complications and rehospitalizations,” said Dr. Malaisrie. “Because we found no detrimental effect of accelerated discharge, both patients and physicians should not be averse to discharging patients when medically ready.”
“Patients can go home after a shorter length of stay in the hospital without increased risk of complications and rehospitalizations,” said Dr. Malaisrie. “Because we found no detrimental effect of accelerated discharge, both patients and physicians should not be averse to discharging patients when medically ready.”
Dr. Malaisrie anticipates that the Northwestern Medicine cardiac ERAS program will result in faster recoveries, reduced complications, decreased time in the hospital, lower costs, and improved patient/family satisfaction. In the future, the researchers plan to closely examine both traditional clinical endpoints and patient-reported outcomes from the program.
“Expectations for recovery after cardiac surgery are being reset in the current era,” he said. “What does this mean for patients? It means that prolonged or taxing recovery is no longer required. Patients should know that recovery from heart surgery is not only quicker, but also better with ERAS programs.”