NYU Langone surgeon Dr. Kepal Patel explains radiofrequency ablation, which is a minimally invasive treatment for large, benign thyroid nodules.
Learn more about treatment for benign thyroid nodules: https://nyulangone.org/conditions/thy…
NYU Langone surgeon Dr. Kepal Patel explains radiofrequency ablation, which is a minimally invasive treatment for large, benign thyroid nodules.
Learn more about treatment for benign thyroid nodules: https://nyulangone.org/conditions/thy…
From a National Poll on Aging (Univ. of Michigan) online release:
 Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago.
Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago.
Among older adults who had looked up doctor ratings within the past year, 65% read reviews of a doctor they were considering, 34% read reviews to find a new doctor, and 31% read reviews for a doctor they had already seen.
 Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a
Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a
national sample of adults age 50–80 about their use and perceptions of online doctor ratings.
From the Journal of Sport and Health Science:
Therefore, promotion of adequate volumes and intensities of physical exercise (i.e., approximately 3 months of moderate-intensity aerobic exercise, with 2–3 sessions/week lasting not less than 30 min) represents an inexpensive and safe strategy for boosting BDNF (brain-derived neurotrophic factor) release that may preserve or restore cognitive function.
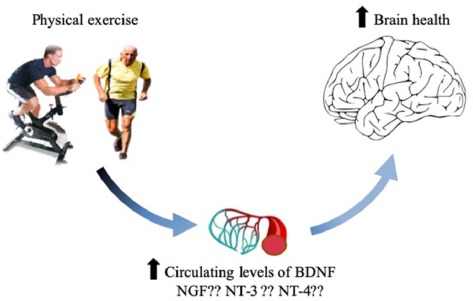
Taken together, the currently available data seemingly confirm the existence of a positive relationship between physical exercise and circulating BDNF levels, both in the short and long term, and also support the beneficial impact of training programs for amplifying the acute BDNF response.
From Wikipedia:
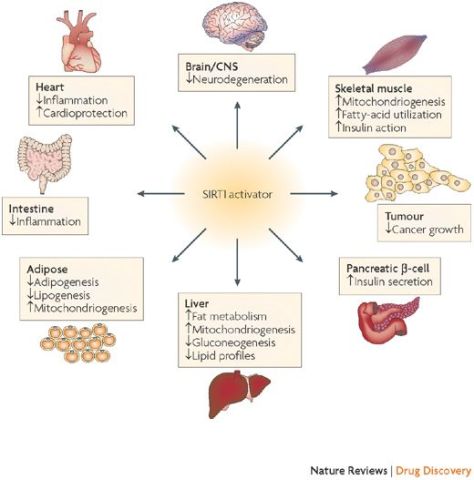
Sirtuins are a class of proteins that possess either mono-ADP-ribosyltransferase, or deacylase activity, including deacetylase, desuccinylase, demalonylase, demyristoylase and depalmitoylase activity. The name Sir2 comes from the yeast gene ‘silent mating-type information regulation 2‘, the gene responsible for cellular regulation in yeast.
From in vitro studies, sirtuins are implicated in influencing cellular processes like aging, transcription, apoptosis, inflammation and stress resistance, as well as energy efficiency and alertness during low-calorie situations. As of 2018, there was no clinical evidence that sirtuins affect human aging.
Although preliminary studies with resveratrol, an activator of deacetylases such as SIRT1, led some scientists to speculate that resveratrol may extend lifespan, there was no clinical evidence for such an effect, as of 2018.
In vitro studies shown that calorie restriction regulates the plasma membrane redox system, involved in mitochondrial homeostasis, and the reduction of inflammation through cross-talks between SIRT1 and AMP-activated protein kinase (AMPK), but the role of sirtuins in longevity is still unclear, as calorie restriction in yeast could extend lifespan in the absence of Sir2 or other sirtuins, while the in vivo activation of Sir2 by calorie restriction or resveratrol to extend lifespan has been challenged in multiple organisms.
This interview originally aired Jan. 4, 2020.
From a NeuroscienceNews.com online release article (01/02/20):
During the years 1976 through 1980, 15% of U.S. adults were obese. Today, about 40%of adults are obese. Another 33% are overweight.
“But, of course, food is now abundant, and our next meal is as close as the kitchen, or the nearest fast-food drive-through, or right here on our desk. Often, these foods are high in fats, sugars, and therefore calories, and that’s why they taste good. It’s easy to overconsume, and, over time, this takes a toll on our health.”
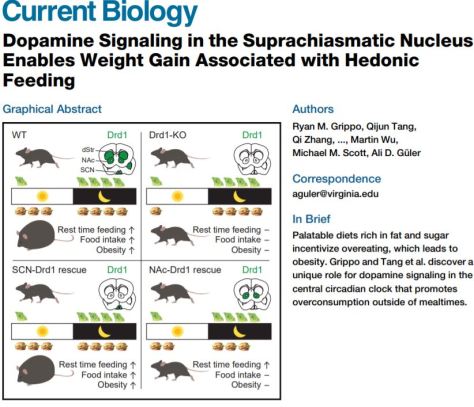
In a study published Thursday in the journal Current Biology, Güler and his colleagues demonstrate that the pleasure center of the brain that produces the chemical dopamine, and the brain’s separate biological clock that regulates daily physiological rhythms, are linked, and that high-calorie foods – which bring pleasure – disrupt normal feeding schedules, resulting in overconsumption. Using mice as study models, the researchers mimicked the 24/7 availability of a high-fat diet, and showed that anytime snacking eventually results in obesity and related health problems.
From a New York Times online article:
 If one geriatrician can care for 700 patients with complicated medical needs, as a federal model estimates, then the nation will need 33,200 such doctors in 2025. It has about 7,000, only half of them practicing full time. (They’re sometimes confused with gerontologists, who study aging, and may work with older adults, but are not health care providers.)
If one geriatrician can care for 700 patients with complicated medical needs, as a federal model estimates, then the nation will need 33,200 such doctors in 2025. It has about 7,000, only half of them practicing full time. (They’re sometimes confused with gerontologists, who study aging, and may work with older adults, but are not health care providers.)
Geriatrics became a board-certified medical specialty only in 1988. An analysis published in 2018 showed that over 16 years, through academic year 2017-18, the number of graduate fellowship programs that train geriatricians, underwritten by Medicare, increased to 210 from 182. That represents virtually no growth when adjusted for the rising United States population.
“It’s basically stagnation,” said Aldis Petriceks, the study’s lead author, now a medical student at Harvard.
From a The Lancet online article:
Effective physicians interrogate their patients’ choice of words as well as their body language; they attend to what they leave out of their stories as well as what they put in. More than 2000 years after Hippocrates, there remains as much poetry in medicine as there is science.
 WHO’s definition of health is famously “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity”. One of the oldest medical texts we know of, The Science of Medicine attributed to Hippocrates, sets out the goal of medicine in comparable terms: “the complete removal of the distress of the sick”.
WHO’s definition of health is famously “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity”. One of the oldest medical texts we know of, The Science of Medicine attributed to Hippocrates, sets out the goal of medicine in comparable terms: “the complete removal of the distress of the sick”.
In my working life as a physician, I’ve never found the distinction between arts and sciences a particularly useful one. In the earliest ancient Greek texts, medicine is described as a techne—a word better translated as “know-how”. It conveys elements of science, art, and skill, but also of artisanal craft. The precise functions of medicine may have subtly shifted over the ages, but our need as human beings for doctors remains the same; we go to them because we wish to invoke some change in our lives, either to cure or prevent an illness or influence some unwelcome mental or bodily process. The goal of medicine is, and always has been, the relief of human suffering—the word patient, from the Latin patientem, means sufferer. And the word physician is from the Greek phusis, or nature: to be engaged in clinical work is to engage oneself with the nature of illness, the nature of recovery, the nature of humanity.
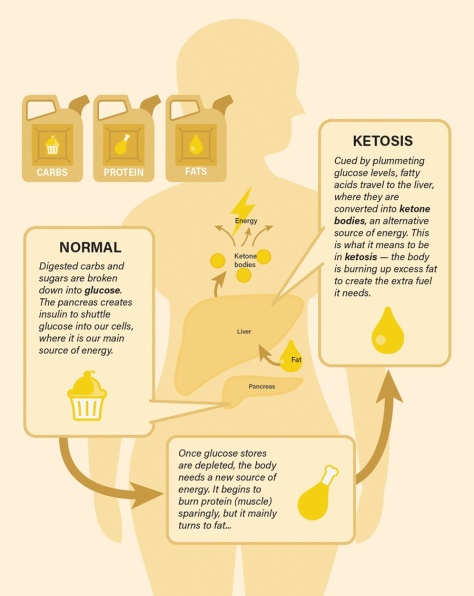
…It seems fasting triggers a dramatic switch in the body’s metabolism, according  to a paper Mattson and colleagues published in February in the experimental biology journal FASEB. In humans, fasting for 12 hours or more drops the levels of glycogen, a form of cellular glucose. Like changing to a backup gas tank, the body switches from glucose to fatty acids, a more efficient fuel. The switch generates the production of ketones, which are energy molecules that are made in the liver. “When the fats are mobilized and used to produce ketones, we think that is a key factor in accruing the health benefits,” says Mattson.
to a paper Mattson and colleagues published in February in the experimental biology journal FASEB. In humans, fasting for 12 hours or more drops the levels of glycogen, a form of cellular glucose. Like changing to a backup gas tank, the body switches from glucose to fatty acids, a more efficient fuel. The switch generates the production of ketones, which are energy molecules that are made in the liver. “When the fats are mobilized and used to produce ketones, we think that is a key factor in accruing the health benefits,” says Mattson.
From a New Atlas online article (Jan 1, 2020):
 “This is an entirely new approach with no current treatments able to change scar in this way,” says Associate Professor James Chong who led the research. “By improving cardiac function and scar formation following heart attack, treatment with rhPDGF-AB led to an overall increase in survival rate in our study.”
“This is an entirely new approach with no current treatments able to change scar in this way,” says Associate Professor James Chong who led the research. “By improving cardiac function and scar formation following heart attack, treatment with rhPDGF-AB led to an overall increase in survival rate in our study.”
The research centers on a protein therapy called recombinant human platelet-derived growth factor-AB (rhPDGF-AB), which had previously been shown to improve heart function in mice that had suffered a heart attack. In a new study aimed at bringing the treatment closer to human trials, a team set out to discover if it produced similar results in large animals, namely pigs.
The researchers from the Westmead Institute for Medical Research (WIMR) and the University of Sydney found that when pigs that had suffered a heart attack received an infusion of rhPDGF, it did indeed prompt the formation of new blood vessels in the heart and led to a reduction of potentially fatal heart arrhythmia.