From a The Lancet online article:
 As a consultant, I had profoundly failed to appreciate the experience of fatigue and apathy among patients. More than excessive tiredness, the fatigue was overwhelming, turning simple activities into insurmountable, exhausting challenges. It was frustrating and I fell into the trap of overexertion when I did have energy, thus exhausting myself and sabotaging the day’s recovery plan. Had staff not been so adept at encouraging me when I lacked energy and holding me back when I tried to overdo things, I would have squandered much valuable rehabilitation time.
As a consultant, I had profoundly failed to appreciate the experience of fatigue and apathy among patients. More than excessive tiredness, the fatigue was overwhelming, turning simple activities into insurmountable, exhausting challenges. It was frustrating and I fell into the trap of overexertion when I did have energy, thus exhausting myself and sabotaging the day’s recovery plan. Had staff not been so adept at encouraging me when I lacked energy and holding me back when I tried to overdo things, I would have squandered much valuable rehabilitation time.
I was a consultant in neurological rehabilitation for acquired brain injury when, at the age of 62 years, I had a stroke. Running for a train, I experienced pain in the right side of my head and mild weakness and sensory loss in my left limbs. I thought I’d had a stroke, but I was remarkably calm. It was late and my instinct was to get home, where I went to the study. In the morning, I found myself on the floor, half-blind, half-paralysed, and terrified.
.
Scans showed a large intracerebral haemorrhage in the area of the right basal ganglia. My symptoms could be explained by the damage to my brain—my medical world was in order, something to hold on to. I discussed my diagnosis and treatment with my colleagues during brief waking periods, grateful that they still saw the person I was before my stroke. Meanwhile, my wife was in the good hands of staff who treated her with sensitivity, giving her plain facts and support.











 Facing shortages of critical equipment, medical workers must make life-or-death decisions about who receives care. WSJ’s Joe Palazzolo reports from an emergency room that’s running short on ventilators, and Chris Weaver explains the plans hospitals are putting in place to decide who gets them.
Facing shortages of critical equipment, medical workers must make life-or-death decisions about who receives care. WSJ’s Joe Palazzolo reports from an emergency room that’s running short on ventilators, and Chris Weaver explains the plans hospitals are putting in place to decide who gets them. 
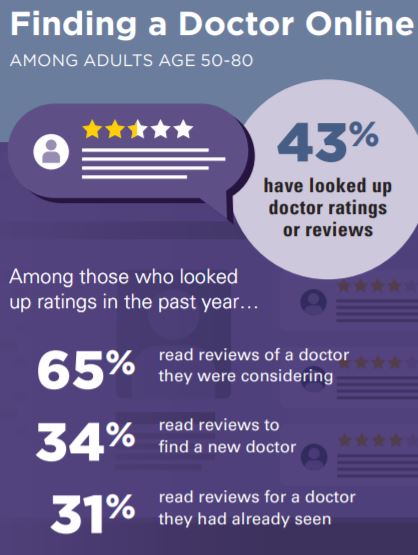 Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago.
Among older adults age 50–80, 43% had ever reviewed doctor ratings; 14% had reviewed ratings more than once in the past year, 19% had done so once in the past year, and 10% had reviewed ratings more than one year ago. Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a
Ratings and reviews for nearly everything can be found online these days, including doctors. How are older adults using these ratings in their decisions about choosing doctors? In May 2019, the University of Michigan National Poll on Healthy Aging asked a
 …primary care providers (general practice, paediatrics, and internal medicine) performed the best, giving a considerably lower percentage of antibiotic prescriptions without a documented indication (12%) than other specialists such as gynaecologists and urologists, who commonly prescribed antibiotics (24%), as well as those in all other specialties (29%).
…primary care providers (general practice, paediatrics, and internal medicine) performed the best, giving a considerably lower percentage of antibiotic prescriptions without a documented indication (12%) than other specialists such as gynaecologists and urologists, who commonly prescribed antibiotics (24%), as well as those in all other specialties (29%).
 This systematic review and meta-analysis of 11 studies involving 21 517 physicians demonstrated an association between physician depressive symptoms and an increased risk for perceived medical errors (RR, 1.95; 95% CI, 1.63-2.33). We also found that the magnitude of the associations of physician depressive symptoms and perceived medical errors were relatively consistent across studies that assessed training and practicing physicians, providing additional evidence that physician depression has implications for the quality of care delivered by physicians at different career stages.
This systematic review and meta-analysis of 11 studies involving 21 517 physicians demonstrated an association between physician depressive symptoms and an increased risk for perceived medical errors (RR, 1.95; 95% CI, 1.63-2.33). We also found that the magnitude of the associations of physician depressive symptoms and perceived medical errors were relatively consistent across studies that assessed training and practicing physicians, providing additional evidence that physician depression has implications for the quality of care delivered by physicians at different career stages.


 As a consultant, I had profoundly failed to appreciate the experience of fatigue and apathy among patients. More than excessive tiredness, the fatigue was overwhelming, turning simple activities into insurmountable, exhausting challenges. It was frustrating and I fell into the trap of overexertion when I did have energy, thus exhausting myself and sabotaging the day’s recovery plan. Had staff not been so adept at encouraging me when I lacked energy and holding me back when I tried to overdo things, I would have squandered much valuable rehabilitation time.
As a consultant, I had profoundly failed to appreciate the experience of fatigue and apathy among patients. More than excessive tiredness, the fatigue was overwhelming, turning simple activities into insurmountable, exhausting challenges. It was frustrating and I fell into the trap of overexertion when I did have energy, thus exhausting myself and sabotaging the day’s recovery plan. Had staff not been so adept at encouraging me when I lacked energy and holding me back when I tried to overdo things, I would have squandered much valuable rehabilitation time. 
 It was all horribly familiar — a rerun of an episode 15 months earlier, when she was with her family in River Vale, N.J. Back then, the burning pressure sent her to the emergency department, and she was told the same thing: She was having a heart attack. Immediately the cardiologist looked for blockages in the coronary arteries, which feed blood and oxygen to the hardworking muscles of her heart. That was the cause of most heart attacks. But they found no blockage.
It was all horribly familiar — a rerun of an episode 15 months earlier, when she was with her family in River Vale, N.J. Back then, the burning pressure sent her to the emergency department, and she was told the same thing: She was having a heart attack. Immediately the cardiologist looked for blockages in the coronary arteries, which feed blood and oxygen to the hardworking muscles of her heart. That was the cause of most heart attacks. But they found no blockage. Indeed, that was the clue that led the rheumatologist to a likely diagnosis: Behcet’s disease. It’s an unusual inflammatory disorder characterized by joint pains, muscle pains and recurrent ulcers in mucus membranes throughout the body. Almost any part of the body can be involved — the eyes, the nose and lungs, the brain, the blood vessels, even the heart. Behcet’s was named after a Turkish dermatologist who in 1937 described a triad of clinical findings including canker sores (medically known as aphthous ulcers), genital ulcers and an inflammatory condition of the eye.
Indeed, that was the clue that led the rheumatologist to a likely diagnosis: Behcet’s disease. It’s an unusual inflammatory disorder characterized by joint pains, muscle pains and recurrent ulcers in mucus membranes throughout the body. Almost any part of the body can be involved — the eyes, the nose and lungs, the brain, the blood vessels, even the heart. Behcet’s was named after a Turkish dermatologist who in 1937 described a triad of clinical findings including canker sores (medically known as aphthous ulcers), genital ulcers and an inflammatory condition of the eye.