When asked how likely they would be to get a COVID-19 vaccine when available and if no cost to them, 58% of older adults indicated they would be likely to get a COVID-19 vaccine (33% very likely, 25% somewhat likely), 28% said they were unlikely (11% somewhat unlikely, 17% very unlikely), and 14% were unsure or did not know.
About two in three older adults (63%) indicated they received a flu shot last flu season. Seven in ten either received one since August 2020 (34%) or intended to get one this flu season (38%). Nearly half of adults age 50–80 (49%) believed that getting a flu vaccine is more important this year compared to other years, 44% said it is just as important, and 7% said it was less important.
Interest in getting a COVID-19 vaccine was more common among those age 65–80 compared with those 50–64 (63% vs. 54%), men compared with women (64% vs. 52%), and Whites compared with Hispanics and Blacks (63% vs. 51% vs. 40%). Individuals who lived with others, had higher household incomes, or had more education were also more likely to report they would get a COVID vaccine.
Half of adults age 50–80 (52%) said they personally knew someone who had COVID-19, and 2% reported having had it themselves. One in five older adults (19%) indicated they personally knew someone who died from COVID-19. The likelihood of getting a COVID-19 vaccine did not differ based on whether respondents knew someone who had COVID-19 or who died from it.
In deciding whether to get a COVID-19 vaccine, older adults rated the following as very important: how well it works (80%), their own research (56%), and if it was recommended by their doctor (52%), public health officials (42%), or family and friends (13%). Cost was rated as very important by 30% of older adults.
Website

















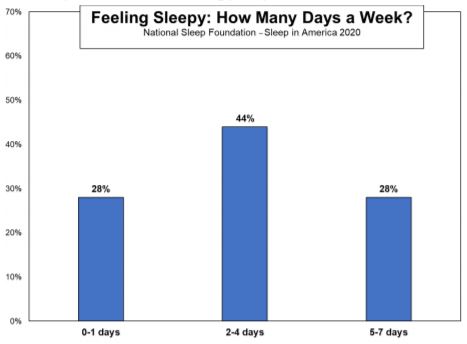
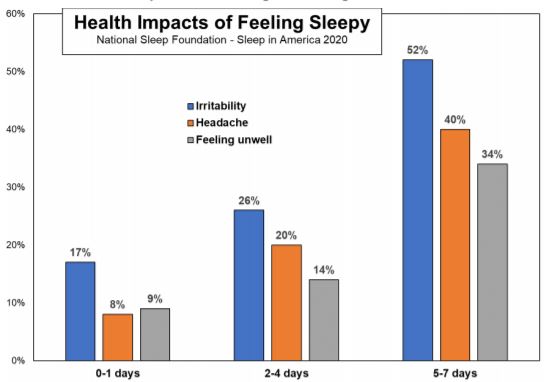
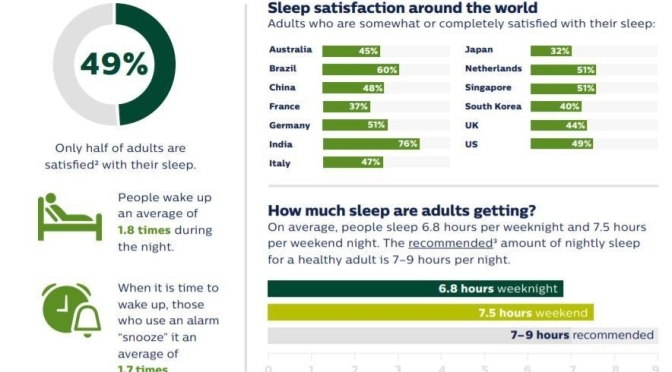
 “The decrease in people taking action to improve sleep is alarming, especially when it is clear people around the world deeply value sleep. Sleep deficit impacts people both mentally and physically, so we need to educate people on available sleep resources and empower them with the confidence that their efforts will pay off,” said Mark Aloia, PhD, Global Lead for Behavior Change, Sleep & Respiratory Care at Philips.
“The decrease in people taking action to improve sleep is alarming, especially when it is clear people around the world deeply value sleep. Sleep deficit impacts people both mentally and physically, so we need to educate people on available sleep resources and empower them with the confidence that their efforts will pay off,” said Mark Aloia, PhD, Global Lead for Behavior Change, Sleep & Respiratory Care at Philips.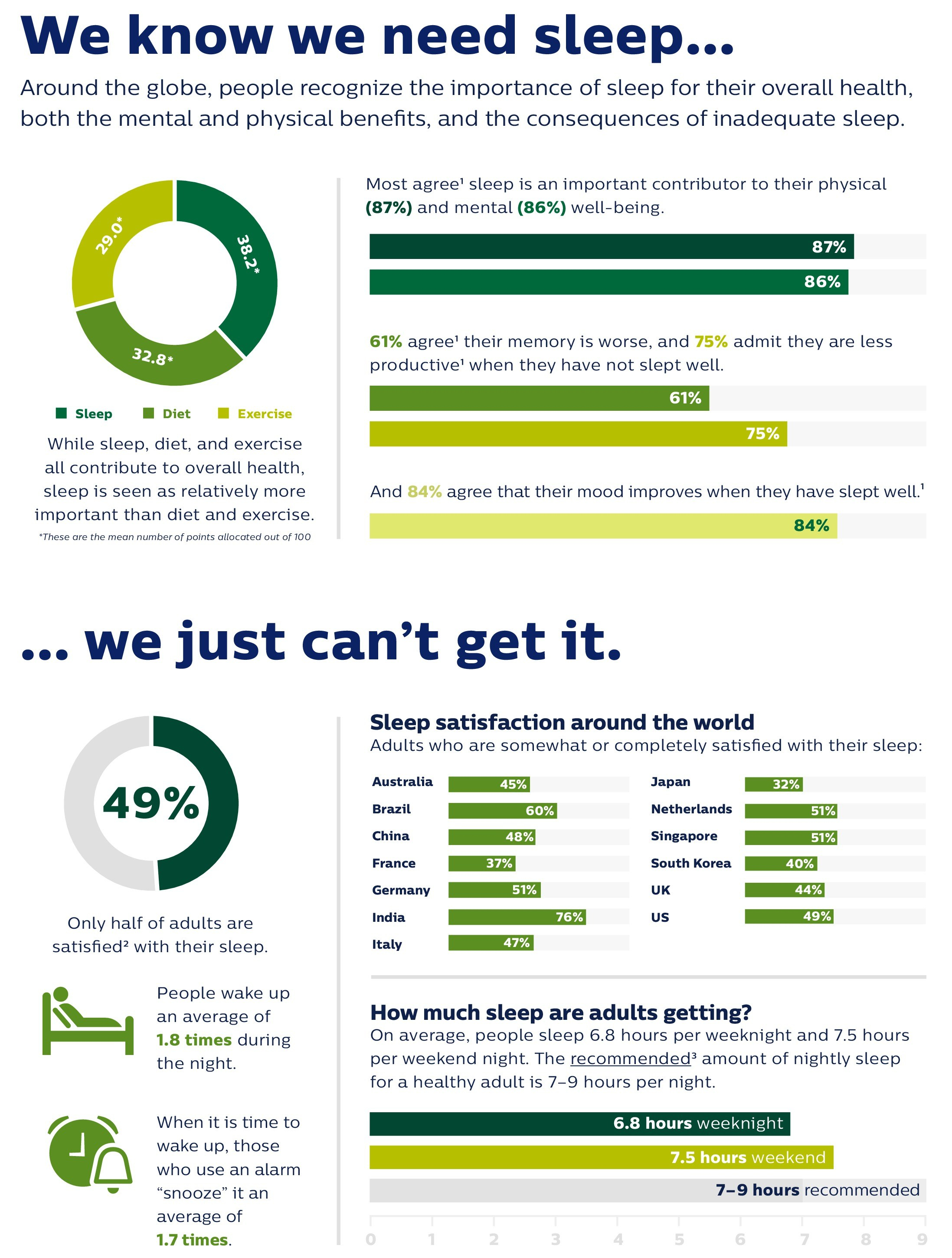

 Many Americans are willing to make significant personal tradeoffs to lower their health insurance rates or medical costs, such as agreeing to 24/7 personal monitoring or working with artificial intelligence instead of a human doctor, the Center for the Digital Future at the USC Annenberg School for Communication and Journalism finds.
Many Americans are willing to make significant personal tradeoffs to lower their health insurance rates or medical costs, such as agreeing to 24/7 personal monitoring or working with artificial intelligence instead of a human doctor, the Center for the Digital Future at the USC Annenberg School for Communication and Journalism finds.
 • For many devices, adoption among adults ages 50 and older is comparable to younger generations. Adults ages 50
• For many devices, adoption among adults ages 50 and older is comparable to younger generations. Adults ages 50