This Friday, March 17, is World Sleep Day, an annual event that aims to raise awareness of the importance of getting a good night’s sleep. This year’s campaign tagline is “Sleep is essential for health.” According to a study by the American College of Cardiology, up to 8 percent of deaths from any cause could be attributed to “poor sleep patterns”, while those with healthier sleep habits are less likely to die prematurely.
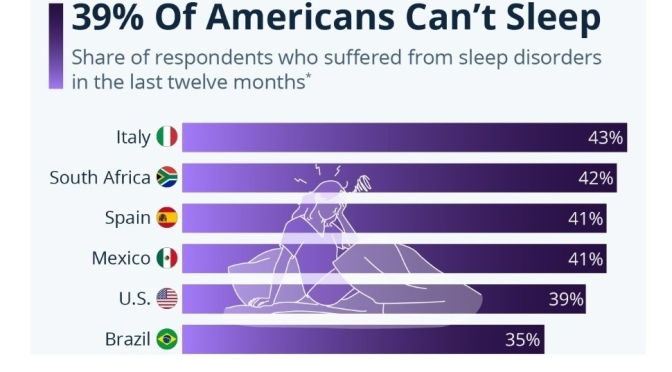
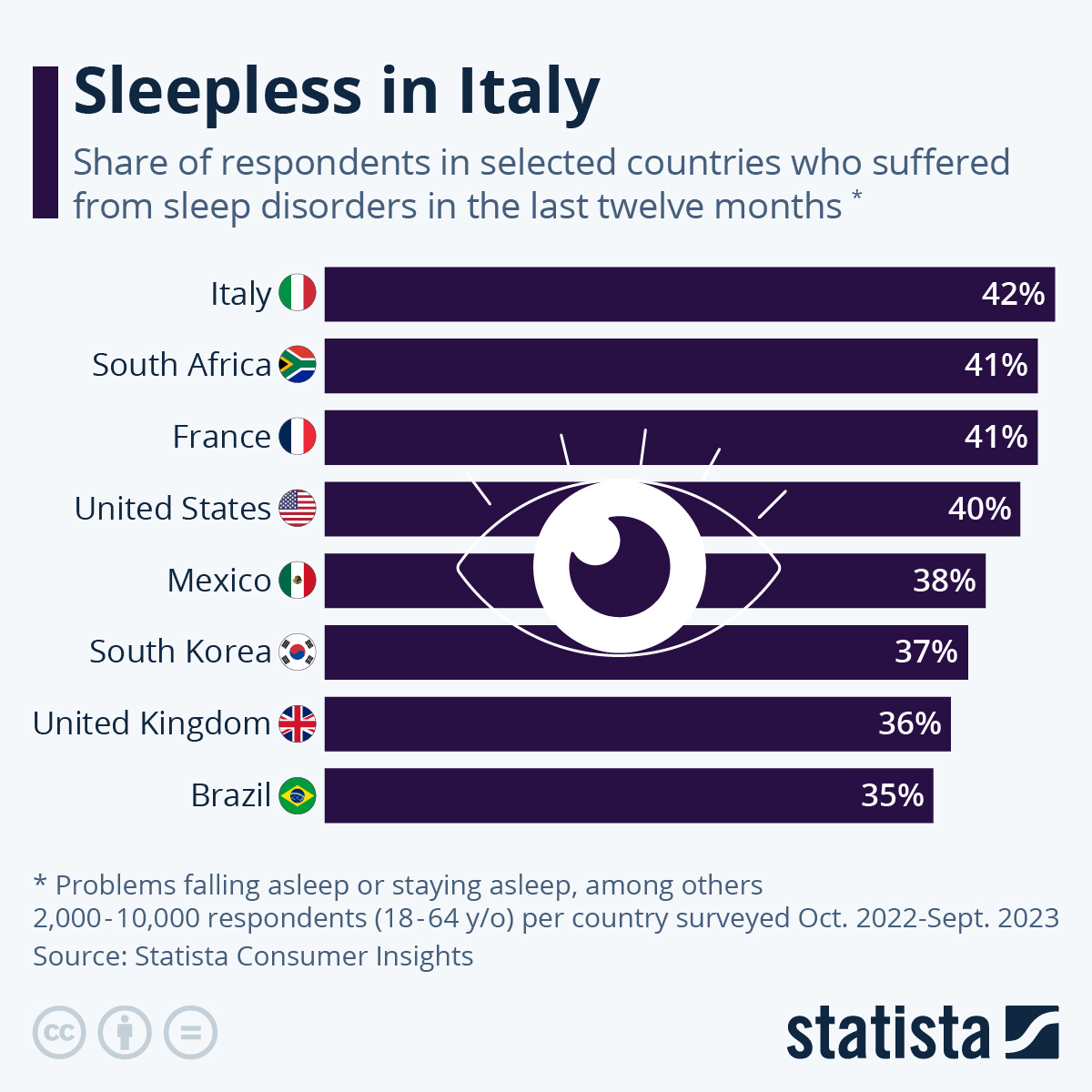
Data from Statista Consumer Insights shows that in the United States, 39 percent of respondents said they had suffered from a sleep disorder (problems falling asleep or staying asleep, insomnia, etc.) in the 12 months prior to the survey. Italians were among the worst sleepers in the survey at 48 percent reporting a sleep disorder, while India registered a higher share of good sleepers, with only 26 percent suffering from poor sleep.