Dear @MayoClinic: My doctor suggested I get a yearly skin check by a dermatologist to check for #melanoma. Why is this necessary? I am almost 50 and have never had any suspicious moles or spots. https://t.co/cVva5q2qbQ #SkinCancer pic.twitter.com/yPjt8W0n1H
— Mayo Clinic Comprehensive Cancer Center (@MayoCancerCare) July 23, 2021
Tag Archives: Dermatology
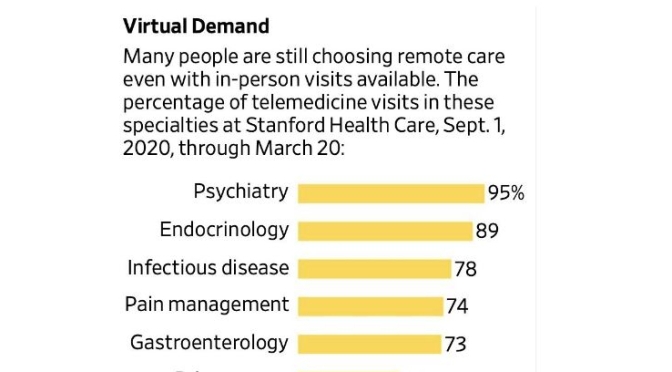
Telemedicine Survey: ‘High Demand’ Continues For Virtual Medical Visits
Future Of Medicine: “The Rise Of Teledermatology”
From AMA.org (June 12, 2020):
 “There’s an aging population, and there’s a lot of skin out there,” said Dr. Isaacs. “One in five people in the country develop skin cancer, but there is a plethora of benign skin conditions that also require the expertise of the dermatologist. So, you have increasing demand and a limited supply of dermatologists.”
“There’s an aging population, and there’s a lot of skin out there,” said Dr. Isaacs. “One in five people in the country develop skin cancer, but there is a plethora of benign skin conditions that also require the expertise of the dermatologist. So, you have increasing demand and a limited supply of dermatologists.”
A basic example of how the TPMG teledermatology program works involves a patient who is concerned about a suspicious lesion or mole on their body. The patient can take a picture of the location in question and send it to their primary care physician for review. The physician can request the patient come in for a more thorough evaluation, or if the physician determines that a dermatologist should be involved, they can send the photo to an on-call dermatologist to review.
If the patient does an in-person evaluation, the physician can also take a higher-quality image and forward that to a dermatologist. The dermatologist can then decide whether there is a problem, if a prescription is needed, or if there should be an in-person evaluation and potential biopsy.
A study in the Journal of the American Academy of Dermatology in 2019 found that when TPMG dermatologists had the chance to look at well-photographed skin lesions, they were able to identify nearly 10% more cancers with almost 40% fewer referrals to the dermatology department.
Health Talk: Stanford Dermatology Professor Eleni Linos On “Tanning Bed” Cancer Research
 “Studies with financial links to the indoor tanning industry were much more likely to discuss perceived benefits of indoor tanning and to downplay the harms,” said Eleni Linos, MD, DrPH, professor of dermatology, who sees patients at Stanford Health Care’s dermatology clinic at the Hoover Pavilion. “The association is quite striking. We need scientific data to be independent of industry influence. I am concerned that funding sources may influence the conclusions of these papers.”
“Studies with financial links to the indoor tanning industry were much more likely to discuss perceived benefits of indoor tanning and to downplay the harms,” said Eleni Linos, MD, DrPH, professor of dermatology, who sees patients at Stanford Health Care’s dermatology clinic at the Hoover Pavilion. “The association is quite striking. We need scientific data to be independent of industry influence. I am concerned that funding sources may influence the conclusions of these papers.”
 In 2012, Eleni Linos, professor of dermatology at Stanford university, published a systematic review and meta-analysis of the link between non-melanoma cancer and sun-beds. That bit of pretty standard research, and a particular rapid response to it, has kicked of years of work – and in this podcast I talk to Eleni and her colleagues Stanton…
In 2012, Eleni Linos, professor of dermatology at Stanford university, published a systematic review and meta-analysis of the link between non-melanoma cancer and sun-beds. That bit of pretty standard research, and a particular rapid response to it, has kicked of years of work – and in this podcast I talk to Eleni and her colleagues Stanton…
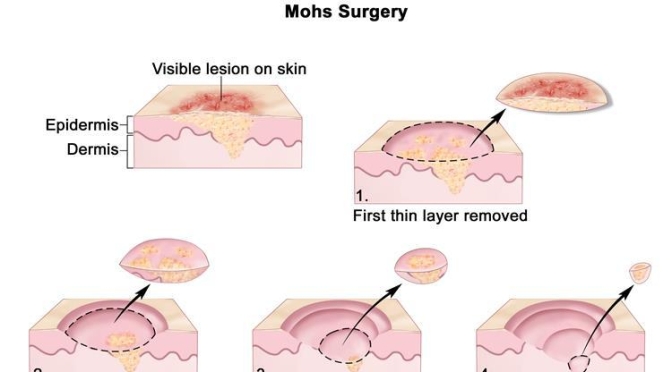
Medical: “Mohs Micrographic Surgery” For Skin Cancer Explained
Named after the late Frederic Mohs, M.D., Mohs micrographic surgery is a highly precise excision technique in which the cancer is removed in stages, one tissue layer at a time. After each removal step, the layer is examined under a microscope to determine whether cancer remains in the patient’s skin and, if present, where exactly it is located so that the surgeon can pinpoint where to remove the remaining skin cancer. This allows for the smallest scar and best cosmetic result.