

March 28, 2021 8:00 am ET




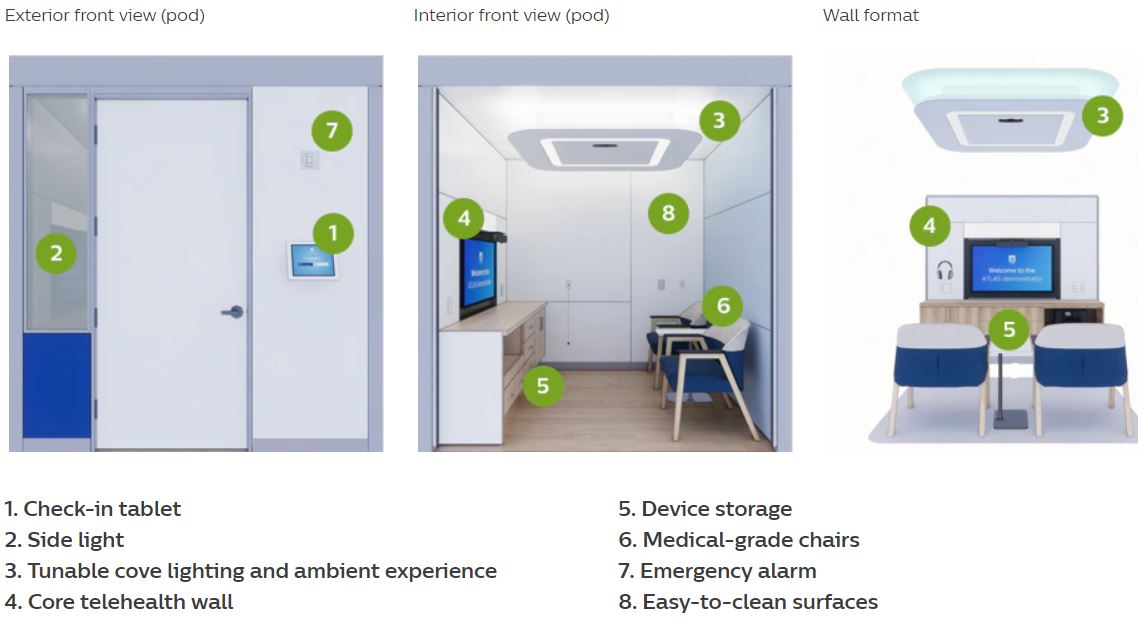
Philips Virtual Care Station, inspired by the VA’s ATLAS program, is a community-based telehealth solution designed to expand access to high-quality care by connecting patients and providers remotely through a secure, clinical-grade environment.
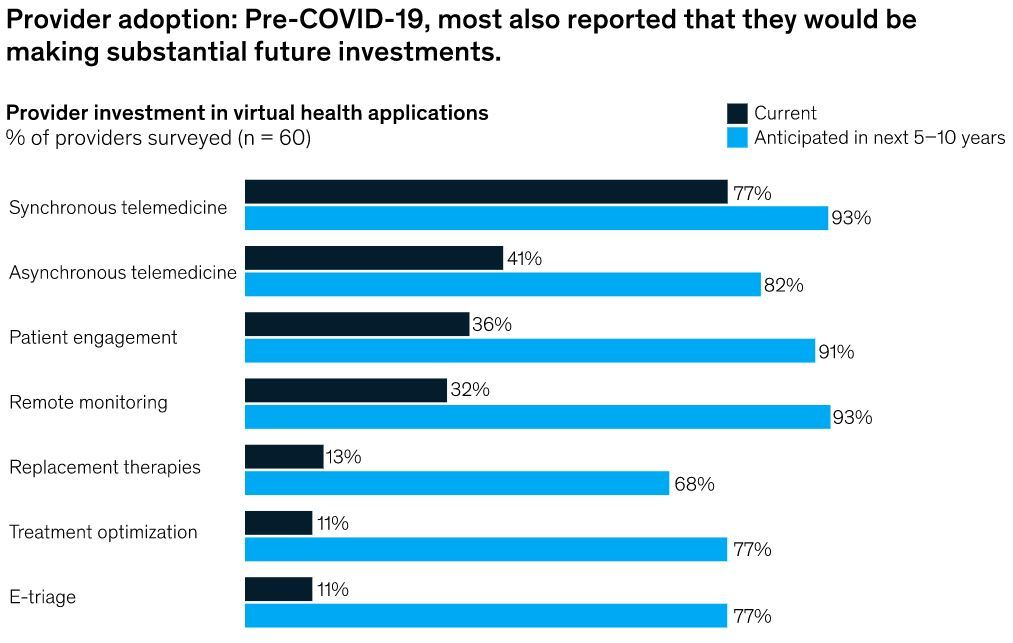
From McKinsey & Company (June 11, 2020)
For the past 10 to 15 years, virtual health has been heralded as the next disrupter in the delivery of care, but there has been minimal uptick in adoption. The COVID-19 pandemic is pushing against structural barriers that had previously slowed health system investment in integrated virtual health applications.

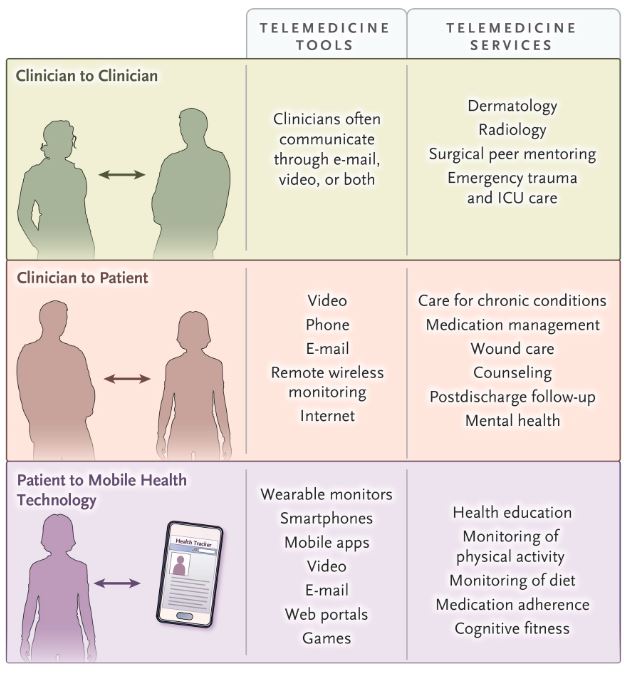
From a New England Journal of Medicine article (March 11, 2020):
 A central strategy for health care surge control is “forward triage” — the sorting of patients before they arrive in the emergency department (ED). Direct-to-consumer (or on-demand) telemedicine, a 21st-century approach to forward triage that allows patients to be efficiently screened, is both patient-centered and conducive to self-quarantine, and it protects patients, clinicians, and the community from exposure.
A central strategy for health care surge control is “forward triage” — the sorting of patients before they arrive in the emergency department (ED). Direct-to-consumer (or on-demand) telemedicine, a 21st-century approach to forward triage that allows patients to be efficiently screened, is both patient-centered and conducive to self-quarantine, and it protects patients, clinicians, and the community from exposure.
It can allow physicians and patients to communicate 24/7, using smartphones or webcam-enabled computers. Respiratory symptoms — which may be early signs of Covid-19 — are among the conditions most commonly evaluated with this approach. Health care providers can easily obtain detailed travel and exposure histories. Automated screening algorithms can be built into the intake process, and local epidemiologic information can be used to standardize screening and practice patterns across providers.
More than 50 U.S. health systems already have such programs. Jefferson Health, Mount Sinai, Kaiser Permanente, Cleveland Clinic, and Providence, for example, all leverage telehealth technology to allow clinicians to see patients who are at home. Systems lacking such programs can outsource similar services to physicians and support staff provided by Teladoc Health or American Well. At present, the major barrier to large-scale telemedical screening for SARS-CoV-2, the novel coronavirus causing Covid-19, is coordination of testing. As the availability of testing sites expands, local systems that can test appropriate patients while minimizing exposure — using dedicated office space, tents, or in-car testing — will need to be developed and integrated into telemedicine workflows.
From a Becker’s Hospital Review online release:
 The VillageMD primary care clinic, called Village Medical at Walgreens, is the first of five sites to open in Houston. Four more clinics are slated to open by the end of the year. The Village Medical clinics are located next to Walgreens stores and offer services including annual preventive care, women’s health services, vaccinations, diagnostic testing, smoking cessation, chronic care management and some specialty care. The clinics offer same-day, walk-in appointments, as well as house calls and virtual visits. The clinics are staffed by primary care physicians, nurses, pharmacists and social workers.
The VillageMD primary care clinic, called Village Medical at Walgreens, is the first of five sites to open in Houston. Four more clinics are slated to open by the end of the year. The Village Medical clinics are located next to Walgreens stores and offer services including annual preventive care, women’s health services, vaccinations, diagnostic testing, smoking cessation, chronic care management and some specialty care. The clinics offer same-day, walk-in appointments, as well as house calls and virtual visits. The clinics are staffed by primary care physicians, nurses, pharmacists and social workers.
Chicago-based primary care company VillageMD is celebrating the opening Nov. 20 of its first primary care clinic at a Walgreens store in Houston, the company announced on Twitter. The Village Medical at Walgreens opening comes just weeks after Walgreens announced plans in October to shutter nearly 160 in-store health clinics.
“Virtual care has great potential for the routine treatment of chronic conditions, as well as minor acute illnesses like rashes and ear infections. Digital sensors already make it possible to monitor blood glucose, heart rhythm, blood pressure, temperature, and sleep.”
 From time immemorial, an invariable feature of doctor–patient interaction has been that it takes place in person. But the status quo is changing. A large portion of patient care might eventually be delivered via telemedicine by virtualists, physicians who treat patients they may never meet.
From time immemorial, an invariable feature of doctor–patient interaction has been that it takes place in person. But the status quo is changing. A large portion of patient care might eventually be delivered via telemedicine by virtualists, physicians who treat patients they may never meet.
The burden of disease has changed dramatically in the past century, shifting from acute infectious illnesses to chronic diseases. Clinic visits are poorly suited for the treatment of chronic diseases, yielding only single-point measurements of labile, continuous variables like blood pressure. Within the time constraints of an office visit, it can be difficult for the physician to make an accurate diagnosis, much less educate the patient about treatment and self-care. And after the patient leaves the doctor’s office, only limited monitoring of the condition is usually possible, without a return visit.
