#England: Positive effects of #Covid-19 vaccinations have been emphasised in new Office for National Statistics data.
— Statista (@StatistaCharts) September 14, 2021
Of all Covid-related deaths in the country from Jan 2nd to July 2nd, 37.4% were people that had not yet been vaccinated to any degree.https://t.co/VGzSTbPCFg pic.twitter.com/wmiOnTPbls
Tag Archives: Death Rates
Obesity & Covid-19: Death Rates 10X Higher In ‘50%+ Overweight Nations’
The majority of global COVID-19 deaths have been in countries where many people are obese, with coronavirus fatality rates 10 times higher in nations where at least 50% of adults are overweight, a global study found.
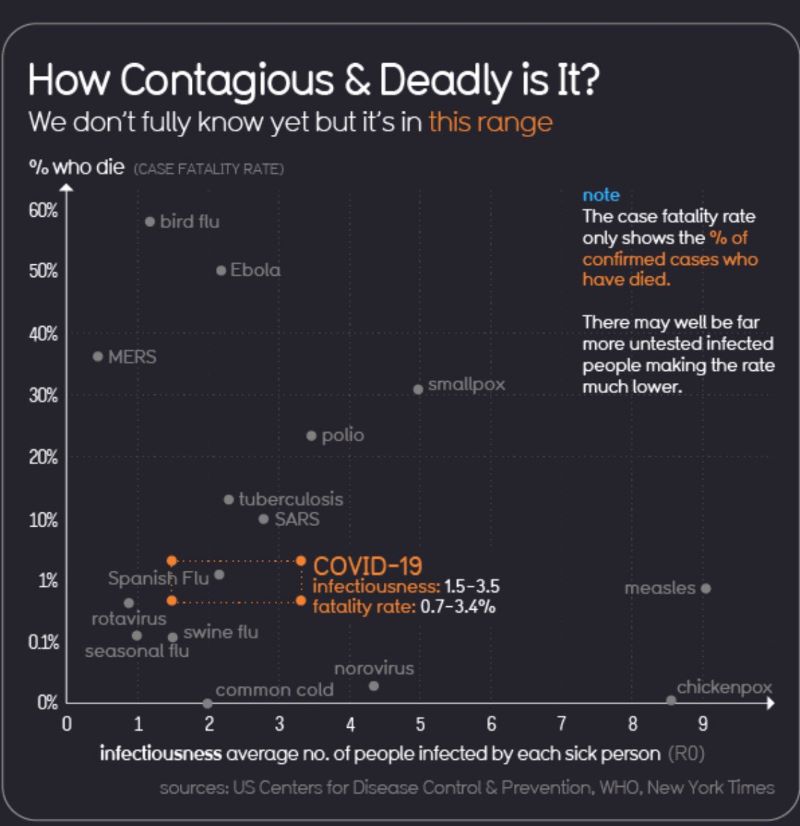
Covid-19 Infographics: “Riskiest Activities, How Contagious & Deadly It Is”

Health Studies: Declining “REM Sleep” Linked To Increasing Death Rates
From U.S. News (July 7, 2020):
“Numerous studies have linked insufficient sleep with significant health consequences. Yet, many people ignore the signs of sleep problems or don’t allow enough time to get adequate sleep,” said lead researcher Eileen Leary. She is a senior manager of clinical research at Stanford University in Palo Alto, Calif.

“REM sleep appears to be a reliable predictor of mortality and may have other predictive health values,” Leary said. “Strategies to preserve REM may influence clinical therapies and reduce mortality risk, particularly for adults with less than 15% of REM sleep.”
REM (rapid eye movement) sleep is when dreams occur and the body repairs itself from the ravages of the day. For every 5% reduction in REM sleep, mortality rates increase 13% to 17% among older and middle-aged adults, researchers report.
For the study, Leary and her colleagues included more than 2,600 men, average age 76, who were followed for a median of 12 years. They also collected data on nearly 1,400 men and women, average age 52, who were part of another study and were followed for a median of 21 years.
Poor REM sleep was tied to early death from any cause as well as death from cardiovascular and other diseases, the researchers found.
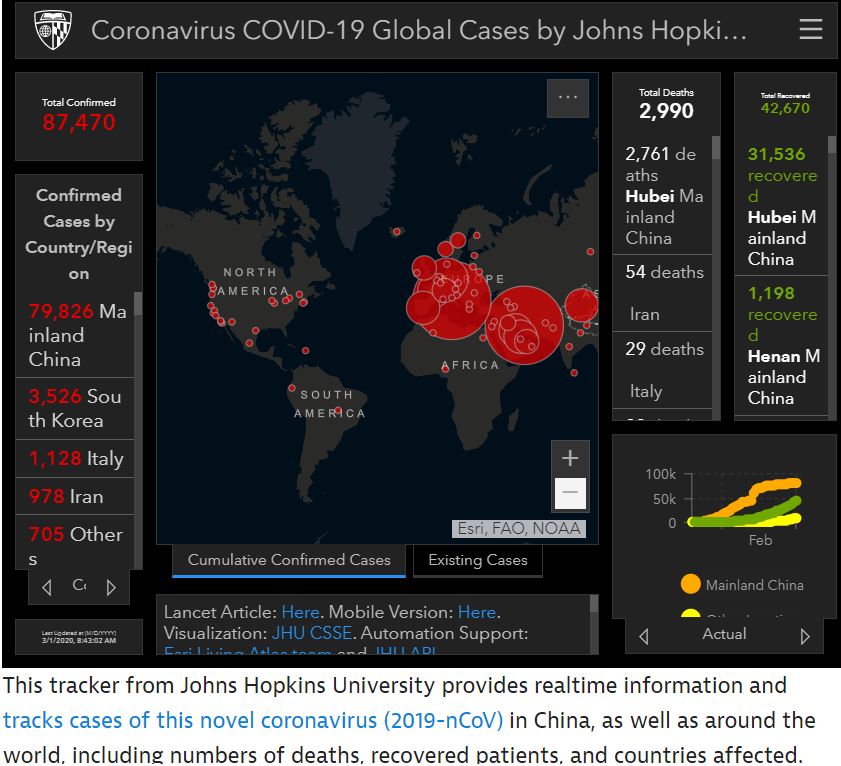
Health: 24/7 Real-Time “Coronavirus / Covid-19” Global Cases & Deaths
Mayo Clinic Health Video: Dangers Of “Sepsis” Now Require Response Teams In Intensive Care Units
Our bodies are very good at fighting infection. The immune system reacts and attacks bacteria and viruses that make us sick. But sometimes the immune reaction is so strong that it damages the body. This is called a septic reaction or sepsis, and the mortality rate associated with it can be high.
In fact, a new study suggests that sepsis is responsible for 20 percent of all deaths worldwide. That’s more deaths than are estimated to be attributable to cancer. At Mayo Clinic, doctors like Kannan Ramar, M.B.B.S., M.D., are trying to change that with a sepsis response team in intensive care units. Their goal: to stop sepsis and save lives.
More health and medical news on the Mayo Clinic News Network. https://newsnetwork.mayoclinic.org/
Health: Heart Disease, Stroke Deaths Are Rising, Even In Healthy States
From a Wall Street Journal online article (01/14/20):
Americans are dying of heart disease and strokes at a rising rate in middle age, normally considered the prime years of life. An analysis of U.S. mortality statistics by The Wall Street Journal shows the problem is geographically widespread.
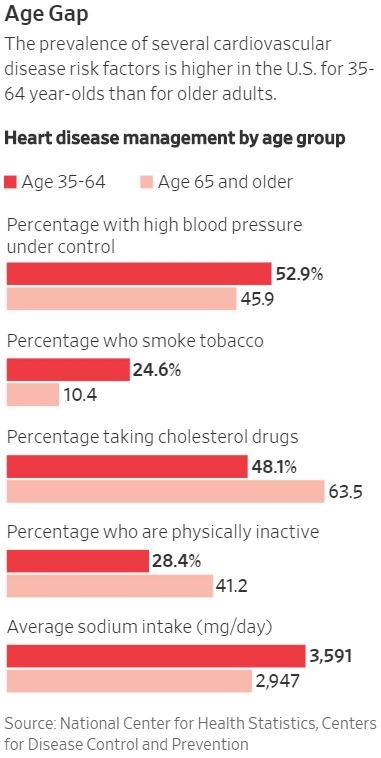 Death rates from cardiovascular disease among people between the ages of 45 and 64 are rising in cities all across the country, including in some of the most unlikely places.
Death rates from cardiovascular disease among people between the ages of 45 and 64 are rising in cities all across the country, including in some of the most unlikely places.
In the Journal’s analysis, three metro areas east of Colorado’s Rocky Mountains—Colorado Springs, Fort Collins and Greeley—recorded some of the biggest increases. Death rates in each rose almost 25%. The three cities boast robust access to exercise and health care. There are bike trails, good heart-disease treatment-and-prevention programs and nearby skiing and hiking.
![]()
Health Study: Death From Heart Disease Four Times Higher In Women With “Poor Exercise Capacity”
From a European Society of Cardiology online release:
 The annual rate of death from cardiovascular disease was nearly four times higher in women with poor, compared to good, exercise capacity (2.2% versus 0.6%). Annual cancer deaths were doubled in patients with poor, compared to good, exercise capacity (0.9% versus 0.4%). The annual rate of death from other causes was more than four times higher in those with poor, compared to good, exercise capacity (1.4% vs. 0.3%).
The annual rate of death from cardiovascular disease was nearly four times higher in women with poor, compared to good, exercise capacity (2.2% versus 0.6%). Annual cancer deaths were doubled in patients with poor, compared to good, exercise capacity (0.9% versus 0.4%). The annual rate of death from other causes was more than four times higher in those with poor, compared to good, exercise capacity (1.4% vs. 0.3%).
Women who can exercise vigorously are at significantly lower risk of dying from heart disease, cancer and other causes. The research is presented today at EuroEcho 2019, a scientific congress of the European Society of Cardiology (ESC).1
During a median follow-up of 4.6 years there were 345 cardiovascular deaths, 164 cancer deaths, and 203 deaths from other causes. After adjusting for factors that could influence the relationship, METs were significantly associated with lower risk of death from cardiovascular disease, cancer, and other causes.
To read more: https://www.escardio.org/The-ESC/Press-Office/Press-releases/Women-exercise-and-longevity
Health Reports: CDC Finds That 35,000 Americans Die Of Antibiotic-Resistant Infections Each Year
 More than 2.8 million antibiotic-resistant infections occur in the United States each year, and more than 35,000 people die as a result. In addition, nearly 223,900 people in the United States required hospital care for C. difficile and at least 12,800 people died in 2017.
More than 2.8 million antibiotic-resistant infections occur in the United States each year, and more than 35,000 people die as a result. In addition, nearly 223,900 people in the United States required hospital care for C. difficile and at least 12,800 people died in 2017.
Germs continue to spread and develop new types of resistance, and progress may be undermined by some community-associated infections that are on the rise. More action is needed to address antibiotic resistance. While the development of new treatments is one of these key actions, such investments must be coupled with dedicated efforts toward preventing infections in the first place, slowing the development of resistance through better antibiotic use, and stopping the spread of resistance when it does develop to protect American lives now and in the future.
CDC’s Antibiotic Resistance Threats in the United States, 2019 (2019 AR Threats Report) includes updated national death and infection estimates that underscore the continued threat of antibiotic resistance in the United States. New CDC data show that while the burden of antibiotic-resistance threats in the United States was greater than initially understood, deaths are decreasing since the 2013 report. This suggests that U.S. efforts—preventing infections, stopping spread of bacteria and fungi, and improving use of antibiotics in humans, animals, and the environment—are working, especially in hospitals. Vaccination, where possible, has also shown to be an effective tool of preventing infections, including those that can be resistant, in the community.
To read the report: https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-report-508.pdf
Exercise Studies: Older Adults’ “Fragmented Physical Exercise” Linked To Higher Death Rates
From a National Institute On Aging release:

Fragmented physical activity, but not total daily activity, was significantly associated with death, the researchers found. For each 10% higher degree of activity fragmentation, mortality risk was 49% greater. The duration of physical activity also mattered: Participants who frequently engaged in short bouts of activity of less than five minutes were more likely to die than those whose activity bouts lasted five minutes or longer. These associations held after adjusting for age, sex, body mass index and other factors.
Daily physical activity, which benefits health and quality of life, typically decreases in older adults. A new study shows that higher fragmentation of that activity — more transitions from activity to sedentariness — may be a better indicator of risk of death than a person’s overall level of physical activity.
Researchers from the Johns Hopkins Bloomberg School of Public Health, Baltimore, analyzed data from the NIA-supported Baltimore Longitudinal Study of Aging (BLSA), looking at a week’s worth of minute-by-minute physical activity for 548 healthy participants age 65 and older (average age, 76).
To read more: https://www.nia.nih.gov/news/fragmented-physical-activity-linked-higher-risk-death-older-adults