National Institute on Aging – As 2022 comes to a close, NIA invites you to explore some of the most popular health information topics from this past year:
High Blood Pressure and Older Adults
— High blood pressure, or hypertension, is common in older adults. The good news is that blood pressure can be controlled in most people.
What Is Menopause?
— Menopause is a normal part of aging for women, but it affects every woman differently.
Memory, Forgetfulness, and Aging: What’s Normal and What’s Not?
— As you age, you may wonder about the difference between normal, age-related forgetfulness and a serious memory problem, such as dementia.
Shingles
— Shingles is a disease that triggers a painful skin rash. About one in three people will get shingles, but there is a vaccine for older adults to help prevent the disease.
Vitamins and Minerals for Older Adults
— Vitamins and minerals are types of nutrients that your body needs to survive and stay healthy.






 “Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?”
“Another behavior change is physical exercise,” Pillemer said. “A paradox of pain is that exercise helps reduce it, but it’s difficult for people in pain to think about exercising. So they don’t exercise, they get more sedentary and the pain increases; it’s a vicious circle. So how do you get people to actually change their behavior?”
 First place prize awarded to MapHabit: This mobile software provides behavior prompts with customizable picture and keyword visual maps to assist memory-impaired people with accomplishing activities of daily living. The care management platform employs different interfaces depending on whether the user is a person with impaired memory, caregiver or long-term care community manager. Caregivers can monitor adherence to medication schedules or track other activities.
First place prize awarded to MapHabit: This mobile software provides behavior prompts with customizable picture and keyword visual maps to assist memory-impaired people with accomplishing activities of daily living. The care management platform employs different interfaces depending on whether the user is a person with impaired memory, caregiver or long-term care community manager. Caregivers can monitor adherence to medication schedules or track other activities.
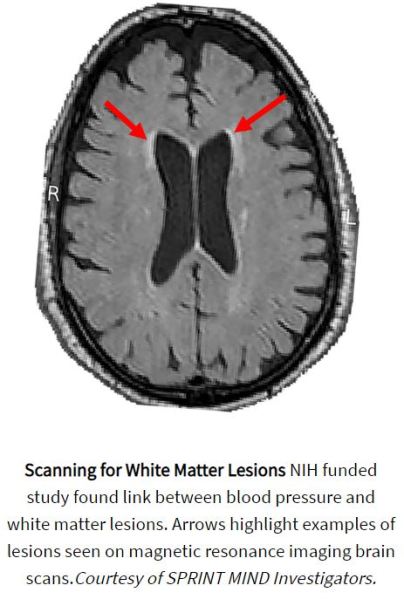 “These initial results support a growing body of evidence suggesting that controlling blood pressure may not only reduce the risk of stroke and heart disease but also of age-related cognitive loss,” said Walter J. Koroshetz, M.D., director of the NIH’s National Institute of Neurological Disorders and Stroke (NINDS). “I strongly urge people to know your blood pressure and discuss with your doctors how to optimize control. It may be a key to your future brain health.”
“These initial results support a growing body of evidence suggesting that controlling blood pressure may not only reduce the risk of stroke and heart disease but also of age-related cognitive loss,” said Walter J. Koroshetz, M.D., director of the NIH’s National Institute of Neurological Disorders and Stroke (NINDS). “I strongly urge people to know your blood pressure and discuss with your doctors how to optimize control. It may be a key to your future brain health.” “A healthy diet and lifestyle are generally recognized as good for health, but this study is the first large randomized controlled trial to look at whether lifestyle changes actually influence Alzheimer’s disease-related brain changes,” said Susan Landau, a research neuroscientist at Berkeley’s Helen Wills Neuroscience Institute, and principal investigator of the add-on study.
“A healthy diet and lifestyle are generally recognized as good for health, but this study is the first large randomized controlled trial to look at whether lifestyle changes actually influence Alzheimer’s disease-related brain changes,” said Susan Landau, a research neuroscientist at Berkeley’s Helen Wills Neuroscience Institute, and principal investigator of the add-on study.