Cremation diamonds: Here's how science can give you an afterlife in the form of shiny compressed carbon. https://t.co/bI6fIY5e5i
— Discover Magazine (@DiscoverMag) October 4, 2021
Tag Archives: Death
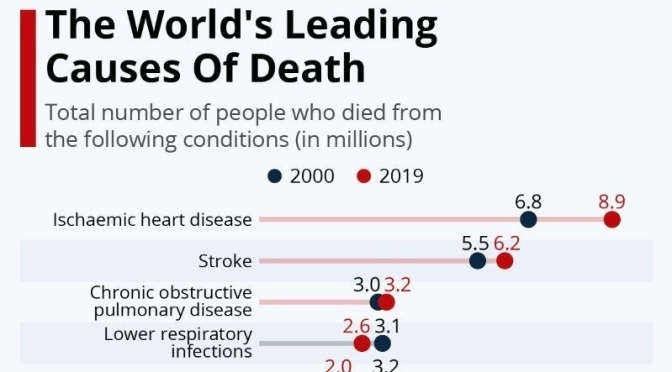
Infographics: ‘Leading Causes Of Death (2000-19)

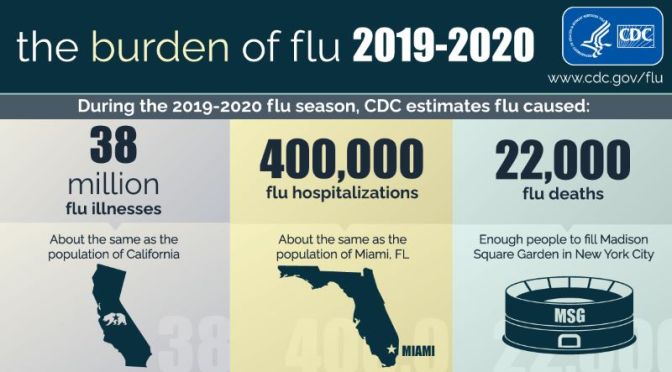
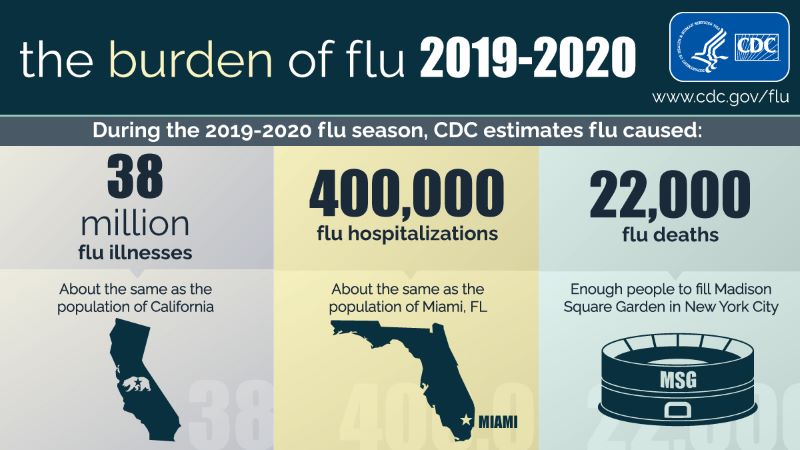
Infographics: ‘The Burden Of Flu & Benefits Of Flu Vaccination’ (2019-2020)

Health Studies: Declining “REM Sleep” Linked To Increasing Death Rates
From U.S. News (July 7, 2020):
“Numerous studies have linked insufficient sleep with significant health consequences. Yet, many people ignore the signs of sleep problems or don’t allow enough time to get adequate sleep,” said lead researcher Eileen Leary. She is a senior manager of clinical research at Stanford University in Palo Alto, Calif.

“REM sleep appears to be a reliable predictor of mortality and may have other predictive health values,” Leary said. “Strategies to preserve REM may influence clinical therapies and reduce mortality risk, particularly for adults with less than 15% of REM sleep.”
REM (rapid eye movement) sleep is when dreams occur and the body repairs itself from the ravages of the day. For every 5% reduction in REM sleep, mortality rates increase 13% to 17% among older and middle-aged adults, researchers report.
For the study, Leary and her colleagues included more than 2,600 men, average age 76, who were followed for a median of 12 years. They also collected data on nearly 1,400 men and women, average age 52, who were part of another study and were followed for a median of 21 years.
Poor REM sleep was tied to early death from any cause as well as death from cardiovascular and other diseases, the researchers found.
Studies: Chronic Sleep Deprivation Causes Toxic Changes In Gut Health, Increased Early Mortality
From Harvard Medical School (June 4, 2020):
“We took an unbiased approach and searched throughout the body for indicators of damage from sleep deprivation. We were surprised to find it was the gut that plays a key role in causing death,” said senior study author Dragana Rogulja, assistant professor of neurobiology in the Blavatnik Institute at HMS.
 The first signs of insufficient sleep are universally familiar. There’s tiredness and fatigue, difficulty concentrating, perhaps irritability or even tired giggles. Far fewer people have experienced the effects of prolonged sleep deprivation, including disorientation, paranoia, and hallucinations.
The first signs of insufficient sleep are universally familiar. There’s tiredness and fatigue, difficulty concentrating, perhaps irritability or even tired giggles. Far fewer people have experienced the effects of prolonged sleep deprivation, including disorientation, paranoia, and hallucinations.
Total, prolonged sleep deprivation, however, can be fatal. While it has been reported in humans only anecdotally, a widely cited study in rats conducted by Chicago-based researchers in 1989 showed that a total lack of sleep inevitably leads to death. Yet, despite decades of study, a central question has remained unsolved: Why do animals die when they don’t sleep?
Now, Harvard Medical School (HMS) neuroscientists have identified an unexpected, causal link between sleep deprivation and premature death.
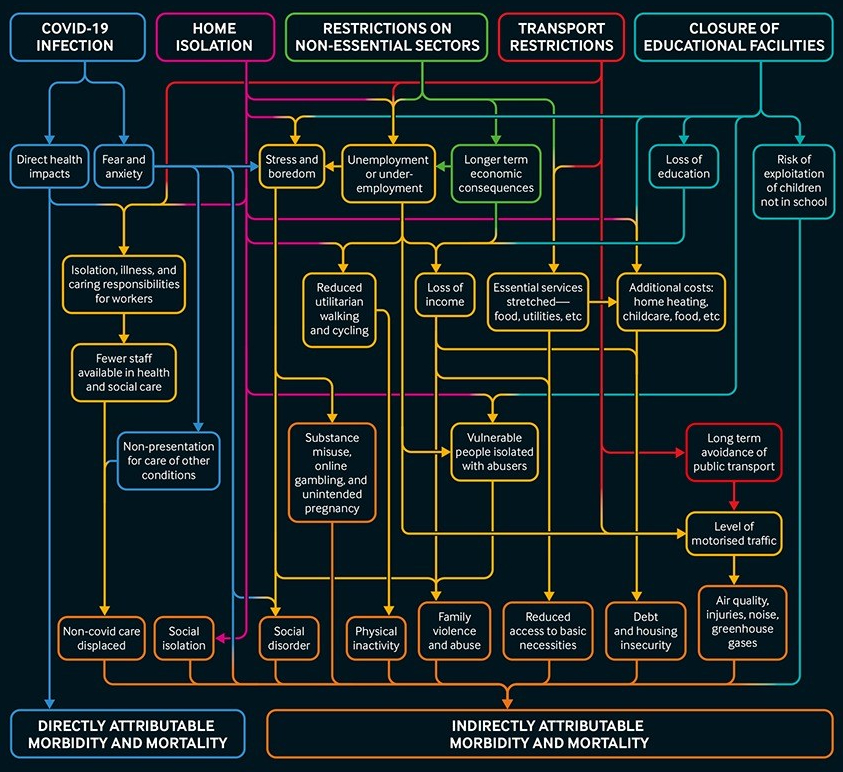
Health Infographic: “The Wide Impact Of The Covid-19 Lockdown” (BMJ)

New Science Podcasts: How Coronavirus Kills People, Quantum Diamond Microscopes & Magnetism
 Coronavirus affects far more than just the lungs, and doctors and researchers in the midst of the pandemic are trying to catalog—and understand—the virus’ impact on our bodies. Staff Writer Meredith Wadman joins host Sarah Crespi to discuss what we know about how COVID-19 kills. See all of our News coverage of the pandemic here, and all of our Research and Editorials here.
Coronavirus affects far more than just the lungs, and doctors and researchers in the midst of the pandemic are trying to catalog—and understand—the virus’ impact on our bodies. Staff Writer Meredith Wadman joins host Sarah Crespi to discuss what we know about how COVID-19 kills. See all of our News coverage of the pandemic here, and all of our Research and Editorials here.
Also this week, Staff Writer Paul Voosen talks with Sarah about quantum diamond microscopes. These new devices are able to detect minute traces of magnetism, giving insight into the earliest movements of Earth’s tectonic plates and even ancient paleomagnetic events in space.
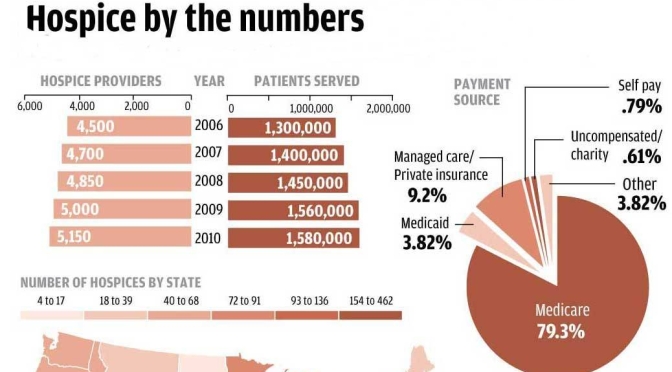
Heathcare Podcasts: An Inside Look At Benefits & Costs Of Hospice (NPR)
 According to a recent Kaiser Family Foundation poll, seven in 10 Americans say they would prefer to die at home. And that’s the direction the health care system is moving, too, hoping to avoid unnecessary and expensive treatment at the end of life.
According to a recent Kaiser Family Foundation poll, seven in 10 Americans say they would prefer to die at home. And that’s the direction the health care system is moving, too, hoping to avoid unnecessary and expensive treatment at the end of life.
Hospice allows a patient deemed to have fewer than six months to live to change the focus of their medical care — from the goal of curing disease to a new goal of using treatments and medicines to maintain comfort and quality of life. It is a form of palliative care, which also focuses on pain management, but can be provided while a patient continues to seek a cure or receive treatments to prolong life.
Interviews: Director Martin Scorsese On Filmmaking & Death (NYT)
From a New York Times online article (01/02/20):

In ways both subtle and substantial, Scorsese sees the world changing and becoming less familiar to him. He gratefully accepted a deal with Netflix, which covered the reported $160 million budget for “The Irishman.” But the bargain meant that, after the movie received a limited theatrical release, it would be shown on the company’s streaming platform.
Scorsese has other aspirations but they have nothing to do with moviemaking. “I would love to just take a year and read,” he said. “Listen to music when it’s needed. Be with some friends. Because we’re all going. Friends are dying. Family’s going.”
Martin Scorsese is the most alive he’s been in his work in a long time, brimming with renewed passion for filmmaking and invigorated by the reception that has greeted his latest gangland magnum opus, “The Irishman.”
And what he wants to talk about is death.
Just to be clear, he’s not talking about the deaths in his movies or anyone else’s. “You just have to let go, especially at this vantage point of age,” he said one Saturday afternoon last month.
Health Reports: CDC Finds That 35,000 Americans Die Of Antibiotic-Resistant Infections Each Year
 More than 2.8 million antibiotic-resistant infections occur in the United States each year, and more than 35,000 people die as a result. In addition, nearly 223,900 people in the United States required hospital care for C. difficile and at least 12,800 people died in 2017.
More than 2.8 million antibiotic-resistant infections occur in the United States each year, and more than 35,000 people die as a result. In addition, nearly 223,900 people in the United States required hospital care for C. difficile and at least 12,800 people died in 2017.
Germs continue to spread and develop new types of resistance, and progress may be undermined by some community-associated infections that are on the rise. More action is needed to address antibiotic resistance. While the development of new treatments is one of these key actions, such investments must be coupled with dedicated efforts toward preventing infections in the first place, slowing the development of resistance through better antibiotic use, and stopping the spread of resistance when it does develop to protect American lives now and in the future.
CDC’s Antibiotic Resistance Threats in the United States, 2019 (2019 AR Threats Report) includes updated national death and infection estimates that underscore the continued threat of antibiotic resistance in the United States. New CDC data show that while the burden of antibiotic-resistance threats in the United States was greater than initially understood, deaths are decreasing since the 2013 report. This suggests that U.S. efforts—preventing infections, stopping spread of bacteria and fungi, and improving use of antibiotics in humans, animals, and the environment—are working, especially in hospitals. Vaccination, where possible, has also shown to be an effective tool of preventing infections, including those that can be resistant, in the community.
To read the report: https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-report-508.pdf