The pandemic of H1N1 virus in 1918 infected about one-third of the world’s population, causing at least 50 million deaths, including more than a half-million in the United States. Martha Teichner reports.
The pandemic of H1N1 virus in 1918 infected about one-third of the world’s population, causing at least 50 million deaths, including more than a half-million in the United States. Martha Teichner reports.
On the Mayo Clinic Radio program, Dr. John Kisiel, a Mayo Clinic gastroenterologist, discusses colorectal cancer and the importance of recommended screening tests.
This interview originally aired March 7, 2020. Disclaimer: Mayo Clinic has a financial interest in Exact Sciences.
Among cancers that affect men and women, colorectal cancer is the second leading cause of cancer deaths in the U.S., according to the Centers for Disease Control and Prevention. Most cases of colorectal cancer begin as small, noncancerous (benign) clumps of cells called polyps. Over time, some polyps become colon cancer. Because these polyps may be small and produce few, if any, symptoms, health care providers recommend regular screening tests to prevent colon cancer. These screenings identify and remove polyps before they become cancerous. March is Colorectal Cancer Awareness month, a time to educate the public about the importance of colorectal cancer screening.
From a March 5, 2020 American Academy of Neurology release:
 “These results are exciting, as they suggest that people may potentially prevent brain shrinking and the effects of aging on the brain simply by becoming more active,” said study author Yian Gu, Ph.D., of Columbia University in New York and a member of the American Academy of Neurology.
“These results are exciting, as they suggest that people may potentially prevent brain shrinking and the effects of aging on the brain simply by becoming more active,” said study author Yian Gu, Ph.D., of Columbia University in New York and a member of the American Academy of Neurology.
“Recent studies have shown that as people age, physical activity may reduce the risk of cognitive decline and dementia. Our study used brain scans to measure the brain volumes of a diverse group of people and found that those who engaged in the top third highest level of physical activity had a brain volume the equivalent of four years younger in brain aging than people who were at the bottom third activity level.”
Older people who regularly walk, garden, swim or dance may have bigger brains than their inactive peers, according to a preliminary study to be presented at the American Academy of Neurology’s 72nd Annual Meeting in Toronto, Canada, April 25 to May 1, 2020. The effect of exercise was equal to four fewer years of brain aging. The study used magnetic resonance imaging (MRI) scans to measure the brains of people with a range of activity levels, including those who were inactive to those who were very active. The scans showed less active people had smaller brain volume.

From a BMJ Research study (March 4, 2020):
 Habitual fish oil supplementation is associated with a 13% lower risk of all cause mortality, a 16% lower risk of CVD mortality, and a 7% lower risk of CVD events among the general population
Habitual fish oil supplementation is associated with a 13% lower risk of all cause mortality, a 16% lower risk of CVD mortality, and a 7% lower risk of CVD events among the general population
Fish oil is a rich source of long chain omega 3 fatty acids, a group of polyunsaturated fats that primarily include eicosapentaenoic acid and docosahexaenoic acid. Initially, these compounds were recommended for daily omega 3 fatty acid supplementation for the prevention of cardiovascular disease (CVD). Consequently, the use of fish oil supplements is widespread in the United Kingdom and other developed countries.
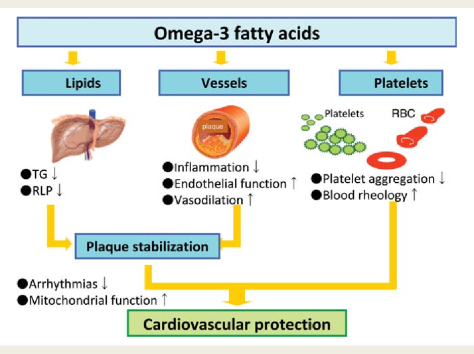
Several mechanisms could explain the benefits for clinical outcome derived from fish oil supplementation. Firstly, the results of several studies have indicated that supplementation with omega 3 fatty acids has beneficial effects on blood pressure, plasma triglycerides, and heart rate, all of which would exert a protective effect against the development of CVD. Secondly, several trials have shown that omega 3 fatty acids can improve flow mediated arterial dilatation, which is a measure of endothelial function and health. Thirdly, omega 3 fatty acids have been shown to possess antiarrhythmic properties that could be clinically beneficial. Finally, studies have reported that fish oil can reduce thrombosis. Additionally, studies have reported that the anti-inflammatory properties of fish oil could have a preventive role in the pathophysiology of CVD outcomes. Other mechanisms could also be involved to explain the effect of fish oil on CVD outcomes.
Hazen and colleagues find that gut bacteria play a central role in the conversion of dietary proteins into a compound, phenylacetylglutamine ( PAGln), which not only is associated with future cardiovascular disease risk in humans but also promotes platelet responsiveness and blood clotting potentially via adrenergic receptors, according to mouse models.
 Rocket scientist-turned-immunology expert Mark Kendall talks about his Nanopatch, which could revolutionise vaccinations and eradicate some diseases.
Rocket scientist-turned-immunology expert Mark Kendall talks about his Nanopatch, which could revolutionise vaccinations and eradicate some diseases.Mark Kendall (born 1972) is an Australian biomedical engineer and innovator. He is an Entrepreneurial Professor of the Australian National University. His field of research is the delivery of immunotherapeutics to the skin without the use of a needle or syringe.
In 2011, he co-founded the development company Vaxxas with an investor syndicate. The company’s technology, called Nanopatch, is intended to serve as a needle-free vaccine delivery device. In 2011, Kendall and his AIBN team received the Australian Research Council Eureka Prize for Excellence in Research by an Interdisciplinary Team. In 2012, he was awarded the Rolex Awards for Enterprise for his “pioneering efforts to expand knowledge and improve human life”.
From an American Heart Assoc. Journal study (Feb 28, 2020):
 Seasonal variation in blood pressure has been known for 40 years, but, to our knowledge, for the first time we show here that this occurs independently of temperature. The reduction in blood pressure is more marked with a rise in UVB than UVA, and in whites than black people. Dermatological concerns about the skin cancer inducing effects of UV radiation need to be balanced against the observed blood pressure lowering effects of sunlight, particularly given the greatly higher burden of disease caused by hypertension.
Seasonal variation in blood pressure has been known for 40 years, but, to our knowledge, for the first time we show here that this occurs independently of temperature. The reduction in blood pressure is more marked with a rise in UVB than UVA, and in whites than black people. Dermatological concerns about the skin cancer inducing effects of UV radiation need to be balanced against the observed blood pressure lowering effects of sunlight, particularly given the greatly higher burden of disease caused by hypertension.
 Sunlight exposure appears to lower blood pressure; insufficient exposure to natural ultraviolet radiation and/or active avoidance of sunlight may be new risk factors for hypertension.
Sunlight exposure appears to lower blood pressure; insufficient exposure to natural ultraviolet radiation and/or active avoidance of sunlight may be new risk factors for hypertension.
Hypertension remains a leading global cause for premature death and disease. Most treatment guidelines emphasize the importance of risk factors, but not all are known, modifiable, or easily avoided. Population blood pressure correlates with latitude and is lower in summer than winter. Seasonal variations in sunlight exposure account for these differences, with temperature believed to be the main contributor. Recent research indicates that UV light enhances nitric oxide availability by mobilizing storage forms in the skin, suggesting incident solar UV radiation may lower blood pressure. We tested this hypothesis by exploring the association between environmental UV exposure and systolic blood pressure (SBP) in a large cohort of chronic hemodialysis patients in whom SBP is determined regularly.
From a BMJ Research online study (March 4, 2020):
 We found no association between egg consumption and risk of cardiovascular disease in three large US cohorts. Results from the updated meta-analysis lend further support to the overall lack of an association between moderate egg consumption (up to one egg per day) and cardiovascular disease risk.
We found no association between egg consumption and risk of cardiovascular disease in three large US cohorts. Results from the updated meta-analysis lend further support to the overall lack of an association between moderate egg consumption (up to one egg per day) and cardiovascular disease risk.
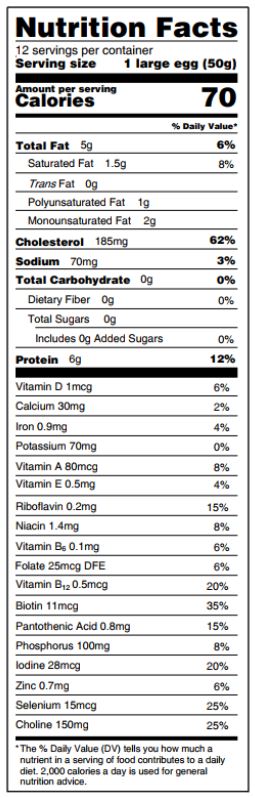 Eggs are a major source of dietary cholesterol, but they are also an affordable source of high quality protein, iron, unsaturated fatty acids, phospholipids, and carotenoids.
Eggs are a major source of dietary cholesterol, but they are also an affordable source of high quality protein, iron, unsaturated fatty acids, phospholipids, and carotenoids.
Introduction: In the United States, cardiovascular disease is the leading cause of death in men and women. Diet and lifestyle undisputedly play a major part in the development of cardiovascular disease. In the past, limiting dietary cholesterol intake to 300 mg per day was widely recommended to prevent cardiovascular disease. However, because of the weak association between dietary cholesterol and blood cholesterol, and considering that dietary cholesterol is no longer a nutrient of concern for overconsumption, the most recent 2015 dietary guidelines for Americans did not carry forward this recommendation.
 What happens when you catch coronavirus? The Telegraph’s Global Health Security Editor Paul Nuki explains all the ways in which you could become infected with COVID-19 and how your body reacts to this virus.
What happens when you catch coronavirus? The Telegraph’s Global Health Security Editor Paul Nuki explains all the ways in which you could become infected with COVID-19 and how your body reacts to this virus.
When the virus enters your body it binds to two cells in the lungs – goblet cells that produce mucus and cilia cells which have hairs on them and normally prevent your lungs filling up with debris and fluid such as virus and bacteria and particles of dust and pollen.
The virus attacks these cells and starts to kill them – so your lungs begin to fill with fluid making it hard for you to breathe. This phase of the disease is thought to last about a week.
At this point your immune system will start to kick in and fight off the invaders. You will develop a fever and your high body temperature will create a hostile environment for the virus. You will start to get rid of the mucus in the form of coughing and a runny nose.
But in some people – particularly the elderly and those with other health conditions – the immune system can go into overdrive. As well as killing the virus it also starts to kill healthy cells.
This heightened immune response can trigger a “cytokine storm” – white blood cells activate a variety of chemicals that can leak into the lungs, which along with the attack on the cells damages them even further. Scans of the lungs show “ground-glass” opacity and then “crazy paving” patterns, as they fill with mucus making it harder and harder to breathe.