Runny nose? Fever? Fatigue? Here’s what doctors want you to know about how to tell the difference between illnesses as we head into flu season https://t.co/bMmW87huQt
— The Wall Street Journal (@WSJ) October 4, 2021
Tag Archives: Illness
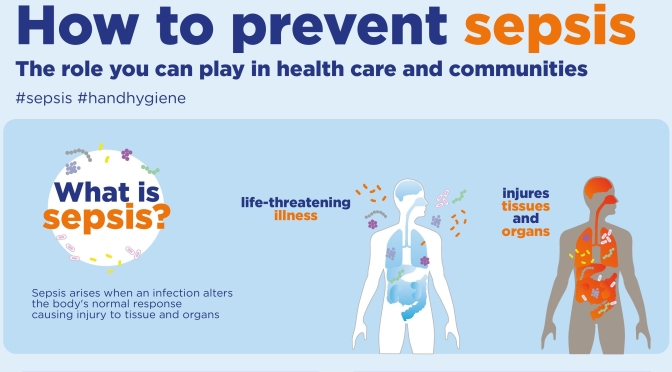
Infographics: “What Is & How To Prevent Sepsis”


Health Update: Ibuprofen Results In “More Severe Illness” For “Coronavirus / Covid-19” Patients (BMJ)
From a BMJ online release (March 17, 2020):
 “The finding in two randomised trials that advice to use ibuprofen results in more severe illness or complications helps confirm that the association seen in observational studies is indeed likely to be causal. Advice to use paracetamol (acetaminophen) is also less likely to result in complications.”
“The finding in two randomised trials that advice to use ibuprofen results in more severe illness or complications helps confirm that the association seen in observational studies is indeed likely to be causal. Advice to use paracetamol (acetaminophen) is also less likely to result in complications.”
Scientists and senior doctors have backed claims by France’s health minister that people showing symptoms of covid-19 should use paracetamol (acetaminophen) rather than ibuprofen, a drug they said might exacerbate the condition.
 Ian Jones, a professor of virology at the University of Reading, said that ibuprofen’s anti-inflammatory properties could “dampen down” the immune system, which could slow the recovery process. He added that it was likely, based on similarities between the new virus (SARS-CoV-2) and SARS I, that covid-19 reduces a key enzyme that part regulates the water and salt concentration in the blood and could contribute to the pneumonia seen in extreme cases. “Ibuprofen aggravates this, while paracetamol does not,” he said.
Ian Jones, a professor of virology at the University of Reading, said that ibuprofen’s anti-inflammatory properties could “dampen down” the immune system, which could slow the recovery process. He added that it was likely, based on similarities between the new virus (SARS-CoV-2) and SARS I, that covid-19 reduces a key enzyme that part regulates the water and salt concentration in the blood and could contribute to the pneumonia seen in extreme cases. “Ibuprofen aggravates this, while paracetamol does not,” he said.
Coronavirus / Covid -19: “What Happens When It Enters Your Body” (Video)
 What happens when you catch coronavirus? The Telegraph’s Global Health Security Editor Paul Nuki explains all the ways in which you could become infected with COVID-19 and how your body reacts to this virus.
What happens when you catch coronavirus? The Telegraph’s Global Health Security Editor Paul Nuki explains all the ways in which you could become infected with COVID-19 and how your body reacts to this virus.
What happens when the virus enters the body?
When the virus enters your body it binds to two cells in the lungs – goblet cells that produce mucus and cilia cells which have hairs on them and normally prevent your lungs filling up with debris and fluid such as virus and bacteria and particles of dust and pollen.
The virus attacks these cells and starts to kill them – so your lungs begin to fill with fluid making it hard for you to breathe. This phase of the disease is thought to last about a week.
At this point your immune system will start to kick in and fight off the invaders. You will develop a fever and your high body temperature will create a hostile environment for the virus. You will start to get rid of the mucus in the form of coughing and a runny nose.
But in some people – particularly the elderly and those with other health conditions – the immune system can go into overdrive. As well as killing the virus it also starts to kill healthy cells.
This heightened immune response can trigger a “cytokine storm” – white blood cells activate a variety of chemicals that can leak into the lungs, which along with the attack on the cells damages them even further. Scans of the lungs show “ground-glass” opacity and then “crazy paving” patterns, as they fill with mucus making it harder and harder to breathe.
Long-Term Care: A Highly Contagious, Drug-Resistant “Fatal Fungus” Spreads In Nursing Homes
From a New York Times online article:
 Scientific research on nursing homes and drug resistance is sparse, but some recent studies offer evidence of the problem. A study published in June in the Journal of Clinical Infectious Diseases found that patients and residents in long-term care settings have alarmingly high rates of drug-resistant colonization, which means they carry the germs on their skin or in their bodies, usually without knowing it, and can pass them invisibly to staff members, relatives or other patients. Elderly or severely ill people with weakened immune systems who carry the germ are at high risk of becoming infected.
Scientific research on nursing homes and drug resistance is sparse, but some recent studies offer evidence of the problem. A study published in June in the Journal of Clinical Infectious Diseases found that patients and residents in long-term care settings have alarmingly high rates of drug-resistant colonization, which means they carry the germs on their skin or in their bodies, usually without knowing it, and can pass them invisibly to staff members, relatives or other patients. Elderly or severely ill people with weakened immune systems who carry the germ are at high risk of becoming infected.
Maria Davila lay mute in a nursing home bed, an anguished expression fixed to her face, as her husband stroked her withered hand. Ms. Davila, 65, suffers from a long list of ailments — respiratory failure, kidney disease, high blood pressure, an irregular heartbeat — and is kept alive by a gently beeping ventilator and a feeding tube.
Doctors recently added another diagnosis to her medical chart: Candida auris, a highly contagious, drug-resistant fungus that has infected nearly 800 people since it arrived in the United States four years ago, with half of patients dying within 90 days.
To read more: www.nytimes.com/2019/09/11/health/nursing-homes-fungus.html?action=click&module=News&pgtype=Homepage