From a Psychology Today online article:
For those with insomnia, however, the stressor appears to be the lack of sleep, and the desire for sleep becomes a stressor in itself. In other words, the fixation on getting sleep leads to feelings of stress over not falling asleep, which begins a vicious loop. According to a model first proposed by Kales et al. in 1976, patients  can develop a conditioned fear of not being able to sleep, which puts them in a state of hyperarousal when they attempt to fall asleep. This makes their inability to sleep a self-fulfilling prophecy.
can develop a conditioned fear of not being able to sleep, which puts them in a state of hyperarousal when they attempt to fall asleep. This makes their inability to sleep a self-fulfilling prophecy.
Insomnia is the most common sleep condition in the world, with half of adults globally reporting occasional episodes. Chronic insomnia, though far less prevalent, affects as many as 10 to 15 percent of the adult population.
Though these sleep problems are extremely common, the neurobiological mechanisms behind insomnia are not entirely understood. Research suggests that emotional stressors do play an outsized role in contributing to sleep problems, and it is well documented that mood and anxiety disorders are common comorbidities with insomnia. This seems like common sense. Emotional arousal, whether due to a state of anxiety or because of intrusive thoughts, makes it difficult to relax, thereby inhibiting one’s ability to either initiate sleep or get back to sleep after waking.
To read more






 can develop a conditioned fear of not being able to sleep, which puts them in a state of hyperarousal when they attempt to fall asleep. This makes their inability to sleep a self-fulfilling prophecy.
can develop a conditioned fear of not being able to sleep, which puts them in a state of hyperarousal when they attempt to fall asleep. This makes their inability to sleep a self-fulfilling prophecy.
 In 2016, Samantha Harvey began to lose sleep. She tried everything to appease her wakefulness: from medication to therapy, changes in her diet to changes in her living arrangements. Nothing seemed to help.
In 2016, Samantha Harvey began to lose sleep. She tried everything to appease her wakefulness: from medication to therapy, changes in her diet to changes in her living arrangements. Nothing seemed to help.
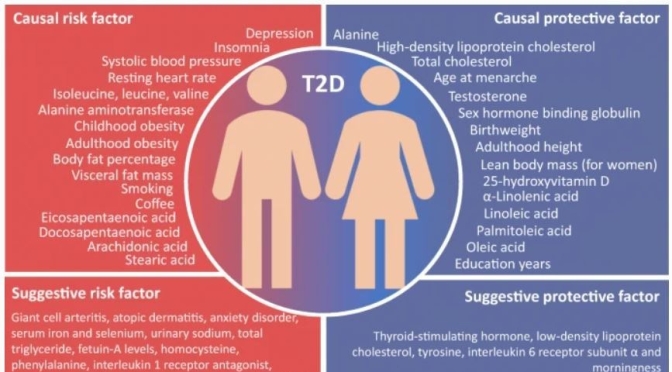
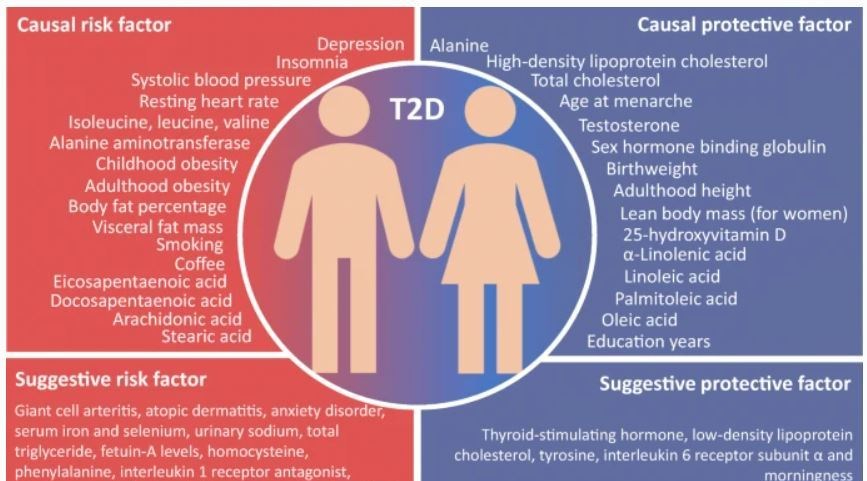
 When the five sleep factors were collapsed into binary categories of low risk vs. high risk (reference group), early chronotype, adequate sleep duration, free of insomnia, and no frequent daytime sleepiness were each independently associated with incident CVD, with a 7%, 12%, 8%, and 15% lower risk, respectively (Table
When the five sleep factors were collapsed into binary categories of low risk vs. high risk (reference group), early chronotype, adequate sleep duration, free of insomnia, and no frequent daytime sleepiness were each independently associated with incident CVD, with a 7%, 12%, 8%, and 15% lower risk, respectively (Table  Cardiovascular disease (CVD), including coronary heart disease (CHD) and stroke, is among the leading causes of mortality globally.
Cardiovascular disease (CVD), including coronary heart disease (CHD) and stroke, is among the leading causes of mortality globally.

 Sleep problems may decrease the likelihood of recovery from chronic low
Sleep problems may decrease the likelihood of recovery from chronic low 
 Beyond the constant tossing and turning of a sleepless night, it might surprise you to know that insomnia is affecting a fair hunk of the Australian population. A recent study released by the Sleep Health Foundation found that 15 per cent of us suffer from chronic insomnia disorder, and very few people are choosing to access help.
Beyond the constant tossing and turning of a sleepless night, it might surprise you to know that insomnia is affecting a fair hunk of the Australian population. A recent study released by the Sleep Health Foundation found that 15 per cent of us suffer from chronic insomnia disorder, and very few people are choosing to access help.