

Join UCLA nephrologist Anjay Rastogi, MD, for an overview of high blood pressure and ways to manage the condition. We will discuss relevant treatment modalities including medications and lifestyle changes.
From a JAMA Network online article (February 4, 2020):
 High medical prices and billing practices may reduce public trust in the medical profession and can result in the avoidance of care. In a survey of 1000 patients, 64% reported that they delayed or neglected seeking medical care in the past year because of concern about high medical bills. The field of quality science in health care has developed measures of medical complications; however, there are no standardized metrics of billing quality.
High medical prices and billing practices may reduce public trust in the medical profession and can result in the avoidance of care. In a survey of 1000 patients, 64% reported that they delayed or neglected seeking medical care in the past year because of concern about high medical bills. The field of quality science in health care has developed measures of medical complications; however, there are no standardized metrics of billing quality.
 A recent study found that only 53 of 101 hospitals were able to provide a price for standard coronary artery bypass graft surgery. Notably, among the hospitals that provided a price, the price ranged from approximately $44 000 and $448 000 and was not associated with quality of care as measured by risk-adjusted outcomes and the Society of Thoracic Surgeons composite quality score.
A recent study found that only 53 of 101 hospitals were able to provide a price for standard coronary artery bypass graft surgery. Notably, among the hospitals that provided a price, the price ranged from approximately $44 000 and $448 000 and was not associated with quality of care as measured by risk-adjusted outcomes and the Society of Thoracic Surgeons composite quality score.
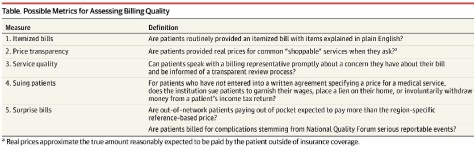
In the same way that there is wide variation in pricing, aggressive collection tactics also can be highly variable by institution. In a recent analysis, 36% (48/135) of hospitals in Virginia garnished wages of patients with unpaid medical bills, and 5 hospitals accounted for 4690 garnishment cases in 2017, representing 51% of all cases.7 In total, 20 054 lawsuits were filed in Virginia against patients for unpaid debt. For many hospitals that sue patients, legal action follows multiple attempts to contact patients through letters and calls, and some hospitals may offer to set up payment plans or even negotiate charges.
We’ve come a long way since the first heartbeat was heard. This American Heart Month, we take a look at the history of cardiac care — and celebrate the leading-edge innovations that make a better future possible.
From a Sleep Medicine online release (January 2020):
 Our findings suggest that LAN (low-level light at night) exposure increases the incidence of diabetes in a general elderly population. Further research involving a large cohort with new-onset diabetes is warranted to elucidate these findings.
Our findings suggest that LAN (low-level light at night) exposure increases the incidence of diabetes in a general elderly population. Further research involving a large cohort with new-onset diabetes is warranted to elucidate these findings.
The circadian timing system, located within the suprachiasmatic nucleus of the hypothalamus, controls fundamental energy homeostasis. Clock gene mutations induce obesity in mice, and the disruption of internal circadian rhythms decreases daily energy expenditures and leptin levels in humans. Light information received by the brain influences human circadian timing and metabolism; low-level light at night (LAN) significantly increased body mass and led to prediabetes in mice. In humans, bedroom LAN affected obesity parameters; however, the association between LAN and the incidence of diabetes in humans has not been studied.

Cardiovascular disease remains the leading cause of death worldwide among middle-aged adults. However, deaths from cancer are catching up in high-income countries according to a study recently published in the medical journal The Lancet. Researchers calculated that cancer kills about twice as many people as cardiovascular disease in more developed countries. Globally, cancer could become the leading cause of death in just a few decades, the study said.
Nationally, there are approximately 18,000 patients on the liver transplant list. Annually, about 6,000 patients receive a liver transplant. Because of the organ shortage, many patients waiting for liver transplants die on the list or become too sick to undergo transplant. Dr. John Roberts offers these solutions: expanded criteria donors, split livers and living donors. Recorded on 10/30/2019.
More from: Organ Failure and Replacement: Why Organs Fail and What Therapies are Available for Organ Replacement (https://www.uctv.tv/organ-failure-rep…)
From a JAMA Network Open online release (Jan 31, 2020):
 Steep incidence increases between 49 and 50 years of age are consistent with previously undetected colorectal cancers diagnosed via screening uptake at 50 years. These cancers are not reflected in observed rates of colorectal cancer in the SEER registries among individuals younger than 50 years. Hence, using observed incidence rates from 45 to 49 years of age alone to assess potential outcomes of earlier screening may underestimate cancer prevention benefits.
Steep incidence increases between 49 and 50 years of age are consistent with previously undetected colorectal cancers diagnosed via screening uptake at 50 years. These cancers are not reflected in observed rates of colorectal cancer in the SEER registries among individuals younger than 50 years. Hence, using observed incidence rates from 45 to 49 years of age alone to assess potential outcomes of earlier screening may underestimate cancer prevention benefits.
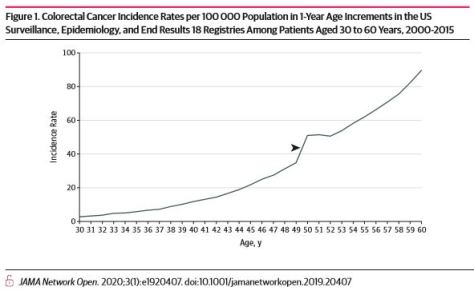
Early-onset colorectal cancer (EOCRC) incidence rates are increasing, and controversy exists regarding whether average-risk screening should begin at 45 or 50 years of age.1 In 2018, the American Cancer Society recommended that average-risk screening start at 45 years of age.2 Others recommend screening at 50 years of age, although the US Multi-Society Task Force on Colorectal Cancer recommends screening African American individuals at age 45 years of age owing to higher incidence, mortality, and earlier-onset disease.3–6 The American Cancer Society decision incorporated modeling studies that used updated incidence and mortality data encompassing time periods of increasing EOCRC incidence rates; modeling compared life-years gained by initiating screening at 45 vs 50 years.
Think of a hernia like a bulge in a damaged tire. The inner tube or soft tissue is normally contained by the abdominal wall, and if there is a leak or weak spot the soft tissue like fat or intestines can protrude through. Having a hernia will eventually require surgery to repair, and there are several different ways surgeons go about it.
From a Technology Networks online article:
 By comparing the pancreatic cells of type 2 diabetic human donors with those of healthy people, researchers at the University of Geneva (UNIGE) and at the University Hospitals of Geneva (HUG), Switzerland, were able to demonstrate, for the first time, that the pancreatic islet cells derived from the Type 2 Diabetic human donors bear compromised circadian oscillators.
By comparing the pancreatic cells of type 2 diabetic human donors with those of healthy people, researchers at the University of Geneva (UNIGE) and at the University Hospitals of Geneva (HUG), Switzerland, were able to demonstrate, for the first time, that the pancreatic islet cells derived from the Type 2 Diabetic human donors bear compromised circadian oscillators.
The disruption of the circadian clocks was concomitant with the perturbation of hormone secretion. Moreover, using clock modulator molecule dubbed Nobiletin, extracted from lemon peel, the researchers succeeded in “repairing” the disrupted cellular clocks and in partial restoring of the islet cell function. These results, published in the Proceedings of the National Academy of Sciences of the United States, provide a first insight into innovative approach for diabetes care.

The circadian clock system (from Latin “circa diem”, about a day) allows the organisms to anticipate periodical changes of geophysical time, and to adjust to these changes. Nearly all the cells in our body comprise molecular clocks that regulate and synchronize metabolic functions to a 24-hour cycle of day-night changes.
Today, increasing evidence show that disturbances in our internal clocks stemming from frequent time zone changes, irregular working schedules or ageing, have a significant impact on the development of metabolic diseases in human beings, including type-2 diabetes. Such disturbances seem to prevent the proper functioning of the cells in the pancreatic islet that secrete insulin and glucagon, the hormones that regulate blood sugar levels.