From a Scientic American online article:
 In our own study of more than 7,000 middle-aged to older adults in the U.K., published in 2019 in Brain Imaging and Behavior, we demonstrated that people who spent more time engaged in moderate to vigorous physical activity had larger hippocampal volumes. Although it is not yet possible to say whether these effects in humans are related to neurogenesis or other forms of brain plasticity, such as increasing connections among existing neurons, together the results clearly indicate that exercise can benefit the brain’s hippocampus and its cognitive functions.
In our own study of more than 7,000 middle-aged to older adults in the U.K., published in 2019 in Brain Imaging and Behavior, we demonstrated that people who spent more time engaged in moderate to vigorous physical activity had larger hippocampal volumes. Although it is not yet possible to say whether these effects in humans are related to neurogenesis or other forms of brain plasticity, such as increasing connections among existing neurons, together the results clearly indicate that exercise can benefit the brain’s hippocampus and its cognitive functions.
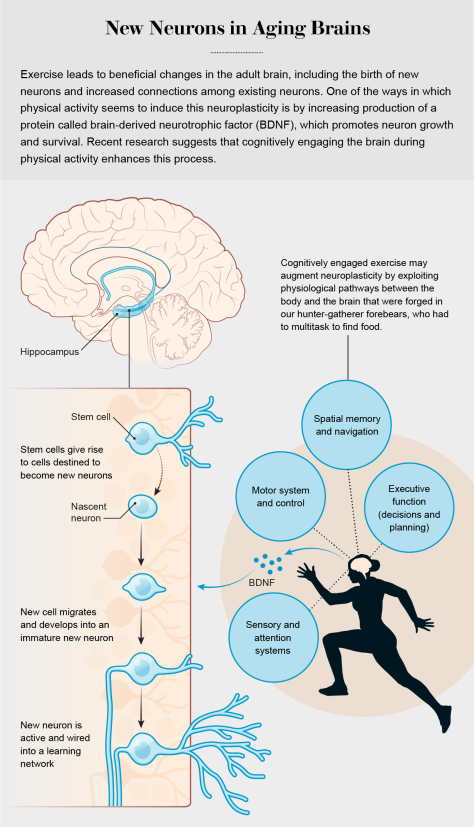
In fact, a growing body of research suggests that exercise that is cognitively stimulating may indeed benefit the brain more than exercise that does not make such cognitive demands. For example, Gerd Kempermann and his colleagues at the Center for Regenerative Therapies Dresden in Germany explored this possibility by comparing the growth and survival of new neurons in the mouse hippocampus after exercise alone or after exercise combined with access to a cognitively enriched environment. They found an additive effect: exercise alone was good for the hippocampus, but combining physical activity with cognitive demands in a stimulating environment was even better, leading to even more new neurons. Using the brain during and after exercise seemed to trigger enhanced neuron survival.
To read more: https://www.scientificamerican.com/article/why-your-brain-needs-exercise/



 In studies of aerobic exercise in patients with knee OA, very few interventions met guideline-recommended dose; there were small to moderate changes in markers of cardiovascular health and no decrease in markers of systemic inflammation. These findings question whether aerobic exercise is being used to its full potential in patients with knee OA.
In studies of aerobic exercise in patients with knee OA, very few interventions met guideline-recommended dose; there were small to moderate changes in markers of cardiovascular health and no decrease in markers of systemic inflammation. These findings question whether aerobic exercise is being used to its full potential in patients with knee OA.

 Produced by WIRED Brand Lab with American Institute of Architects | How can design transform emergency rooms from one of the most stressful and chaotic places into a place of healing? Dr. Bon Ku and architect Billie Faircloth, AIA, break down the science behind designing a better work environment for hospitals.
Produced by WIRED Brand Lab with American Institute of Architects | How can design transform emergency rooms from one of the most stressful and chaotic places into a place of healing? Dr. Bon Ku and architect Billie Faircloth, AIA, break down the science behind designing a better work environment for hospitals.


 In people with Type 1 diabetes, the pancreas can’t make insulin. Those with the condition require several doses of insulin a day and spent $5,705 per person on it in 2016, an increase of $2,841, or 99%, per person since 2012, according to the nonprofit
In people with Type 1 diabetes, the pancreas can’t make insulin. Those with the condition require several doses of insulin a day and spent $5,705 per person on it in 2016, an increase of $2,841, or 99%, per person since 2012, according to the nonprofit  Costs continue to rise, so much so that almost half of people with diabetes have temporarily skipped taking their insulin, according to a 2018 survey by UpWell Health, a Salt Lake City company that provides home delivery of medications and supplies for chronic conditions.
Costs continue to rise, so much so that almost half of people with diabetes have temporarily skipped taking their insulin, according to a 2018 survey by UpWell Health, a Salt Lake City company that provides home delivery of medications and supplies for chronic conditions.
 “Our data indicate that there are no low-risk procedures among patients who are frail,” Dr. Hall and his co-authors concluded in their study.
“Our data indicate that there are no low-risk procedures among patients who are frail,” Dr. Hall and his co-authors concluded in their study.