World Economic Forum (August 26, 2023) – This week’s top stories of the week include:
0:15 Scientists develop concrete battery – It could one day be built into the foundations of homes or incorporated into a roadway so electric cars can charge contactlessly as they drive. MIT researchers discovered a new ‘supercapacitor’ by combining cement with carbon black. A sooty residue left over when things burn, and mixing them both with water.
1:48 3 farmers tell how heat is affecting their crops – Experts rank the food supply crisis as one of the world’s top 5 currently manifesting risks. This German farmer has started planting lavender. It’s best suited to the sandy soils and sunshine of the Mediterranean but climate change is bringing these conditions to southern Germany. The lavender is used in cosmetics and perfumes. Matthias Tafelmeier planted his first lavender crop in 2019 after what he says was a decade of declining soil quality. Farmers in the region are also trying other crops more suited to warmer climates such as chickpeas and kidney beans.
3:25 Smartwatch detects Parkinson’s 7 years early – By keeping track of our movement, they can help doctors spot who is vulnerable, years before visible symptoms show up. Cardiff University scientists looked at data from 100,000 smartwatch wearers. Tracking their speed of movement over a single week between 2013 and 2016. Using AI, the team could distinguish those who went on to develop Parkinson’s from those who didn’t and detect early signs up to 7 years in advance.
5:04 Cleaning your house can help tidy your mind – “Cleaning is a great practice, which reminds you of the connection with the ground and the Earth and the universe.” To Buddhists, cleaning is not just cleaning. In Zen Buddhism, it’s known as samu, or work practice and it offers the chance to meditate and be present in the midst of daily tasks.
_____________________________________________
The World Economic Forum is the International Organization for Public-Private Cooperation. The Forum engages the foremost political, business, cultural and other leaders of society to shape global, regional and industry agendas. We believe that progress happens by bringing together people from all walks of life who have the drive and the influence to make positive change.







 More than 6 million people worldwide have Parkinson disease. Even though it is classically associated with tremors, the disease has many manifestations and is very treatable for most patients.
More than 6 million people worldwide have Parkinson disease. Even though it is classically associated with tremors, the disease has many manifestations and is very treatable for most patients.



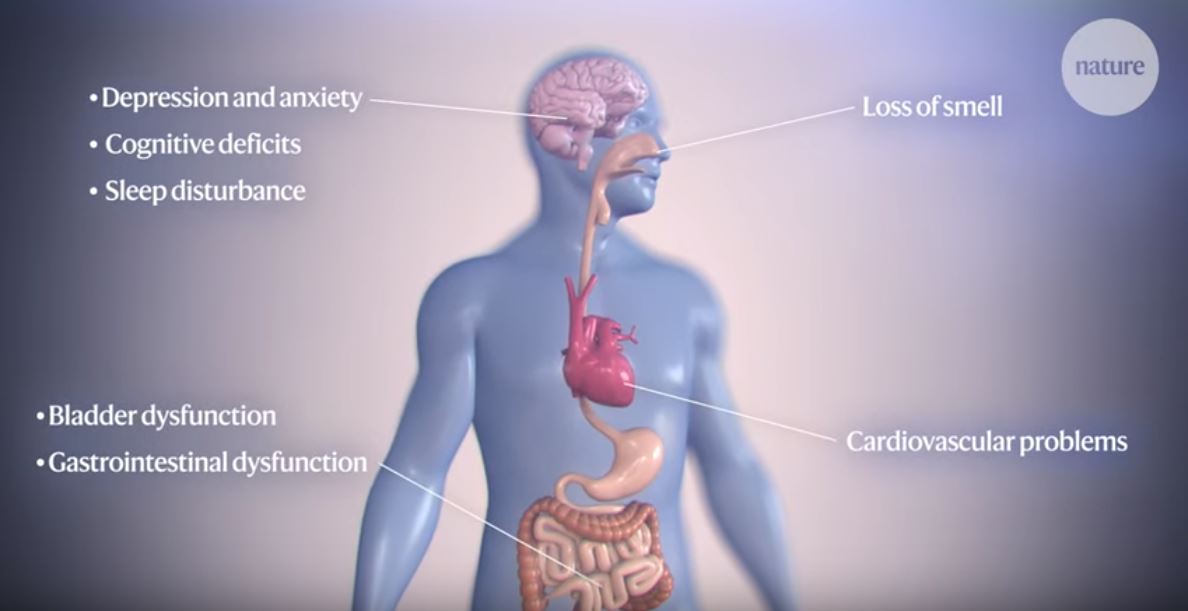

 “The link between antibiotic exposure and Parkinson’s disease fits the current view that in a significant proportion of patients the pathology of Parkinson’s may originate in the gut, possibly related to microbial changes, years before the onset of typical Parkinson motor symptoms such as slowness, muscle stiffness and shaking of the extremities. It was known that the bacterial composition of the intestine in Parkinson’s patients is abnormal, but the cause is unclear. Our results suggest that some commonly used antibiotics, which are known to strongly influence the gut microbiota, could be a predisposing factor,” says research team leader, neurologist Filip Scheperjans MD, Ph.D. from the Department of Neurology of Helsinki University Hospital.
“The link between antibiotic exposure and Parkinson’s disease fits the current view that in a significant proportion of patients the pathology of Parkinson’s may originate in the gut, possibly related to microbial changes, years before the onset of typical Parkinson motor symptoms such as slowness, muscle stiffness and shaking of the extremities. It was known that the bacterial composition of the intestine in Parkinson’s patients is abnormal, but the cause is unclear. Our results suggest that some commonly used antibiotics, which are known to strongly influence the gut microbiota, could be a predisposing factor,” says research team leader, neurologist Filip Scheperjans MD, Ph.D. from the Department of Neurology of Helsinki University Hospital.