
Adults aged 85 years and older, the “oldest old,” are the fastest-growing age group in the United States, yet relatively little is known about their cancer burden. Combining data from the National Cancer Institute, the North American Association of Central Cancer Registries, and the National Center for Health Statistics, the authors provide comprehensive information on cancer occurrence in adults aged 85 years and older. In 2019, there will be approximately 140,690 cancer cases diag-nosed and 103,250 cancer deaths among the oldest old in the United States. The most common cancers in these individuals (lung, breast, prostate, and colorectum) are the same as those in the general population. Overall cancer incidence rates peaked in the oldest men and women around 1990 and have subsequently declined, with the pace accelerating during the past decade. These trends largely reflect declines in cancers of the prostate and colorectum and, more recently, cancers of the lung among men and the breast among women.

To read entire study click on following link: https://onlinelibrary.wiley.com/doi/epdf/10.3322/caac.21577



 For the study, nearly 8,300 people at risk for heart disease had fasting and nonfasting lipid profile tests done at least four weeks apart. (Fasting means they had nothing to eat or drink except water for at least eight hours before the test.) The differences in their total, LDL, and HDL cholesterol values were negligible. Triglyceride levels were modestly higher in the nonfasting samples.
For the study, nearly 8,300 people at risk for heart disease had fasting and nonfasting lipid profile tests done at least four weeks apart. (Fasting means they had nothing to eat or drink except water for at least eight hours before the test.) The differences in their total, LDL, and HDL cholesterol values were negligible. Triglyceride levels were modestly higher in the nonfasting samples.
 “These initial results support a growing body of evidence suggesting that controlling blood pressure may not only reduce the risk of stroke and heart disease but also of age-related cognitive loss,” said Walter J. Koroshetz, M.D., director of the NIH’s National Institute of Neurological Disorders and Stroke (NINDS). “I strongly urge people to know your blood pressure and discuss with your doctors how to optimize control. It may be a key to your future brain health.”
“These initial results support a growing body of evidence suggesting that controlling blood pressure may not only reduce the risk of stroke and heart disease but also of age-related cognitive loss,” said Walter J. Koroshetz, M.D., director of the NIH’s National Institute of Neurological Disorders and Stroke (NINDS). “I strongly urge people to know your blood pressure and discuss with your doctors how to optimize control. It may be a key to your future brain health.”
 Slower speech, for example, could indicate fatigue or sorrow at one point in time, but over longer periods could signal something more severe, co-founder Jim Harper said.
Slower speech, for example, could indicate fatigue or sorrow at one point in time, but over longer periods could signal something more severe, co-founder Jim Harper said.
 Dr. Grace Dammann, medical director of the Pain Clinic at Laguna Honda Hospital, and seven of her colleagues talk about what does and does not work in the treatment of chronic pain. She talks as both a patient and a provider. There is also a discussion of various non-pharmacologic and complementary medicine modalities to treat pain.
Dr. Grace Dammann, medical director of the Pain Clinic at Laguna Honda Hospital, and seven of her colleagues talk about what does and does not work in the treatment of chronic pain. She talks as both a patient and a provider. There is also a discussion of various non-pharmacologic and complementary medicine modalities to treat pain.

 In people having lack of Vitamin D, the muscle strength of waist, back, neck decreases. Decreased muscle strength can cause herniated disc and cervical discal hernia. All of this is reflected in the patient’s pain. We wanted to pay attention to the necessity of considering the lack of Vitamin D in low back pain (LBP) which is one of the common complaints of our patients.
In people having lack of Vitamin D, the muscle strength of waist, back, neck decreases. Decreased muscle strength can cause herniated disc and cervical discal hernia. All of this is reflected in the patient’s pain. We wanted to pay attention to the necessity of considering the lack of Vitamin D in low back pain (LBP) which is one of the common complaints of our patients.
 Antibiotic resistance is a global threat for public health. It is widely acknowledged that antibiotics at sub-inhibitory concentrations are important in disseminating antibiotic resistance via horizontal gene transfer. While there is high use of non-antibiotic human-targeted pharmaceuticals in our societies, the potential contribution of these on the spread of antibiotic resistance has been overlooked so far. Here, we report that commonly consumed non-antibiotic pharmaceuticals, including nonsteroidal anti-inflammatories (ibuprofen, naproxen, diclofenac), a lipid-lowering drug (gemfibrozil), and a β-blocker (propanolol), at clinically and environmentally relevant concentrations, significantly accelerated the conjugation of plasmid-borne antibiotic resistance genes.
Antibiotic resistance is a global threat for public health. It is widely acknowledged that antibiotics at sub-inhibitory concentrations are important in disseminating antibiotic resistance via horizontal gene transfer. While there is high use of non-antibiotic human-targeted pharmaceuticals in our societies, the potential contribution of these on the spread of antibiotic resistance has been overlooked so far. Here, we report that commonly consumed non-antibiotic pharmaceuticals, including nonsteroidal anti-inflammatories (ibuprofen, naproxen, diclofenac), a lipid-lowering drug (gemfibrozil), and a β-blocker (propanolol), at clinically and environmentally relevant concentrations, significantly accelerated the conjugation of plasmid-borne antibiotic resistance genes.
 The quality scorecard rates health care organizations through a five-star system on more than 30 health measures outlined by an advisory council composed of consumer advocates, providers, community organizations, state agencies, and payers. The range of measures focus on the quality of care provided by primary care providers and span more than 10 areas, including behavioral health, children’s health, women’s health, chronic conditions, and preventative health.
The quality scorecard rates health care organizations through a five-star system on more than 30 health measures outlined by an advisory council composed of consumer advocates, providers, community organizations, state agencies, and payers. The range of measures focus on the quality of care provided by primary care providers and span more than 10 areas, including behavioral health, children’s health, women’s health, chronic conditions, and preventative health.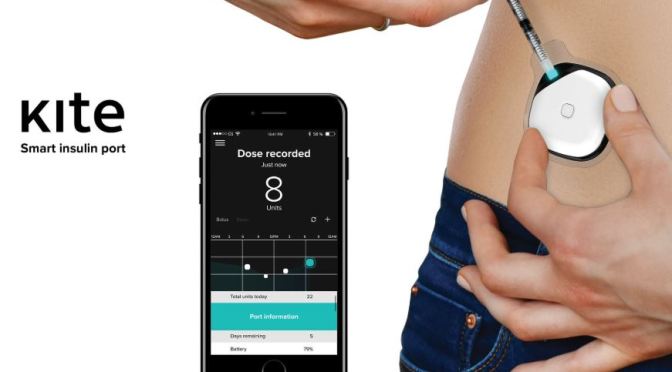
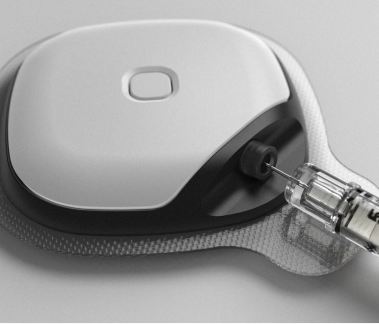 Imagine a smart insulin port attached to your skin, delivering the right dose, and at the right time. At the same moment, getting all information regarding your sugar levels, meds timings and health data, managed and analyzed with the accompanying app.
Imagine a smart insulin port attached to your skin, delivering the right dose, and at the right time. At the same moment, getting all information regarding your sugar levels, meds timings and health data, managed and analyzed with the accompanying app.
 Six factors measured by age 50 were excellent predictors of those who would be in the “happy-well” group–the top quartile of the Harvard men–at age 80: a stable marriage, a mature adaptive style, no smoking, little use of alcohol, regular exercise, and maintenance of normal weight. At age 50, 106 of the men had five or six of these factors going for them, and at 80, half of this group were among the happy-well. Only eight fell into the “sad-sick” category, the bottom quarter of life outcomes. In contrast, of 66 men who had only one to three factors at age 50, not a single one was rated happy-well at 80. In addition, men with three or fewer factors, though still in good physical health at 50, were three times as likely to be dead 30 years later as those with four or more.
Six factors measured by age 50 were excellent predictors of those who would be in the “happy-well” group–the top quartile of the Harvard men–at age 80: a stable marriage, a mature adaptive style, no smoking, little use of alcohol, regular exercise, and maintenance of normal weight. At age 50, 106 of the men had five or six of these factors going for them, and at 80, half of this group were among the happy-well. Only eight fell into the “sad-sick” category, the bottom quarter of life outcomes. In contrast, of 66 men who had only one to three factors at age 50, not a single one was rated happy-well at 80. In addition, men with three or fewer factors, though still in good physical health at 50, were three times as likely to be dead 30 years later as those with four or more.