


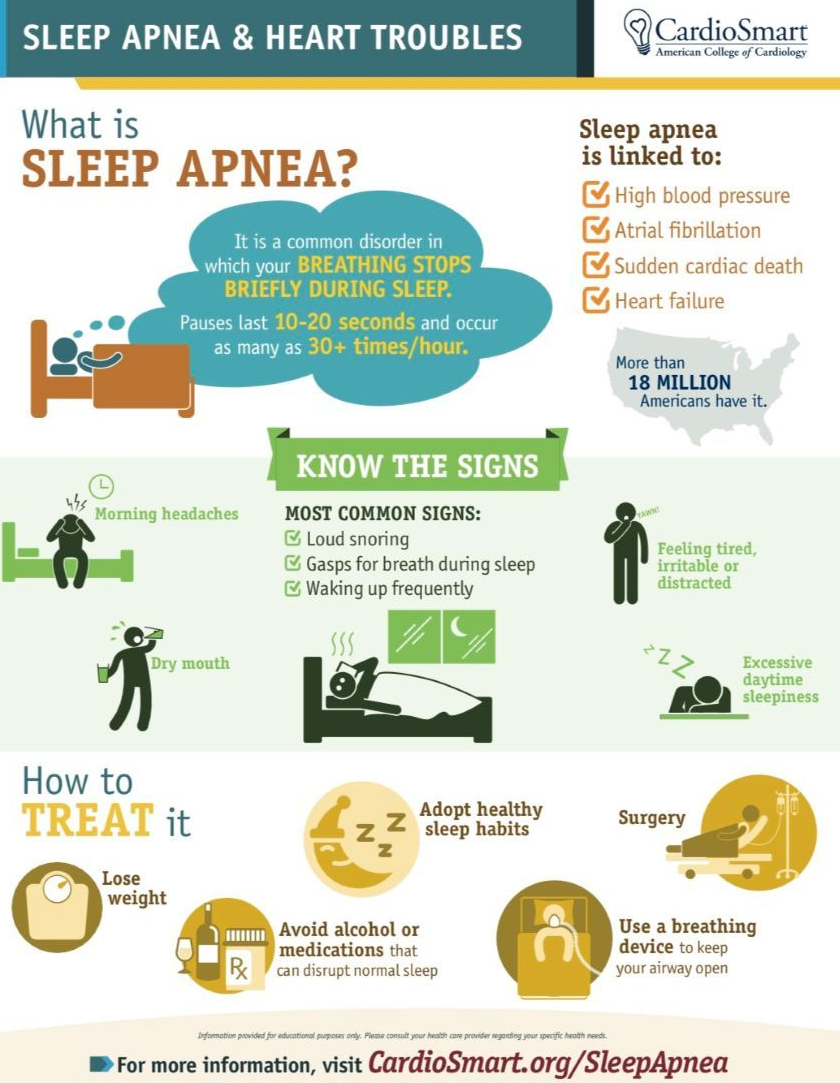

As many as 400,000 Americans die each year because of medical errors, but many of these deaths could be prevented by using electronic sensors and artificial intelligence to help medical professionals monitor and treat vulnerable patients in ways that improve outcomes while respecting privacy.
Haque, who compiled the 170 scientific papers cited in the Nature article, said the field is based largely on the convergence of two technological trends: the availability of infrared sensors that are inexpensive enough to build into high-risk care-giving environments, and the rise of machine learning systems as a way to use sensor input to train specialized AI applications in health care.
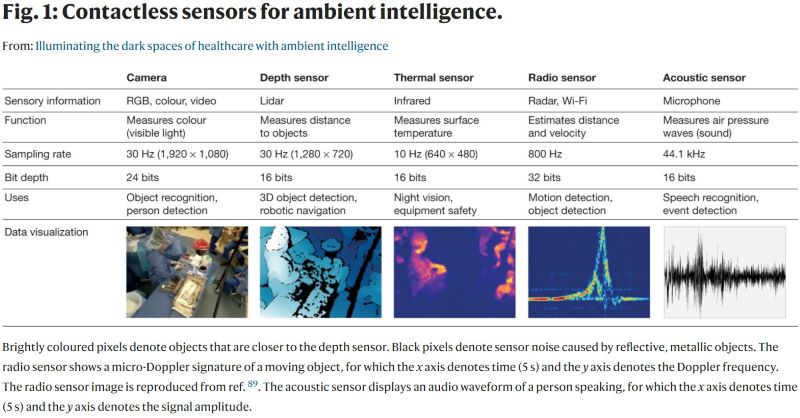
These alert systems are being tested to see if they can reduce the number of ICU patients who get nosocomial infections — potentially deadly illnesses contracted by patients due to failure of other people in the hospital to fully adhere to infection prevention protocols.
Constant monitoring by ambient intelligence systems in a home environment could also be used to detect clues of serious illness or potential accidents, and alert caregivers to make timely interventions. For instance, when frail seniors start moving more slowly or stop eating regularly, such behaviors can presage depression, a greater likelihood of a fall or the rapid onset of a dangerous health crisis. Researchers are developing activity recognition algorithms that can sift through infrared sensing data to detect changes in habitual behaviors, and help caregivers get a more holistic view of patient well-being.

But on its own, “BMI [body mass index] remains a strong independent risk factor” for severe COVID-19, according to several studies that adjusted for age, sex, social class, diabetes, and heart conditions, says Naveed Sattar, an expert in cardiometabolic disease at the University of Glasgow. “And it seems to be a linear line, straight up.”
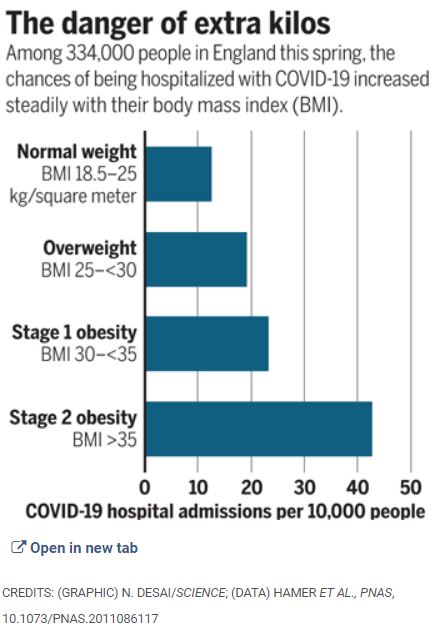
The impact extends to the 32% of people in the United States who are overweight. The largest descriptive study yet of hospitalized U.S. COVID-19 patients, posted as a preprint last month by Genentech researchers, found that 77% of nearly 17,000 patients hospitalized with COVID-19 were overweight (29%) or obese (48%). (The Centers for Disease Control and Prevention defines overweight as having a BMI of 25 to 29.9 kilograms per square meter, and obesity as a BMI of 30 or greater.)

The coronavirus pandemic led to shortages in the blood supply across the U.S. Scientists around the world are working on a potential solution. The Future of Everything looks at the process of making artificial blood.
Illustration: Timothy Wong
CENTERS FOR DISEASE CONTROL & PREVENTION (August 25, 2020) – A CDC study published today that looked at more than 80,000 U.S. adults hospitalized with flu over eight flu seasons (2010-11 through 2017-18) found that sudden, serious heart complications were common and occurred in one out of every eight patients (~12% of patients).

The study looked at a range of sudden heart complications called “acute cardiac events” that resulted in the following:
The most common acute cardiac events reported in the study were acute heart failure and acute ischemic heart disease. Acute heart failure is the sudden inability of the heart to pump enough blood to meet the body’s demands, while acute ischemic heart disease is a term that describes heart problems caused by narrowed or blocked heart arteries.
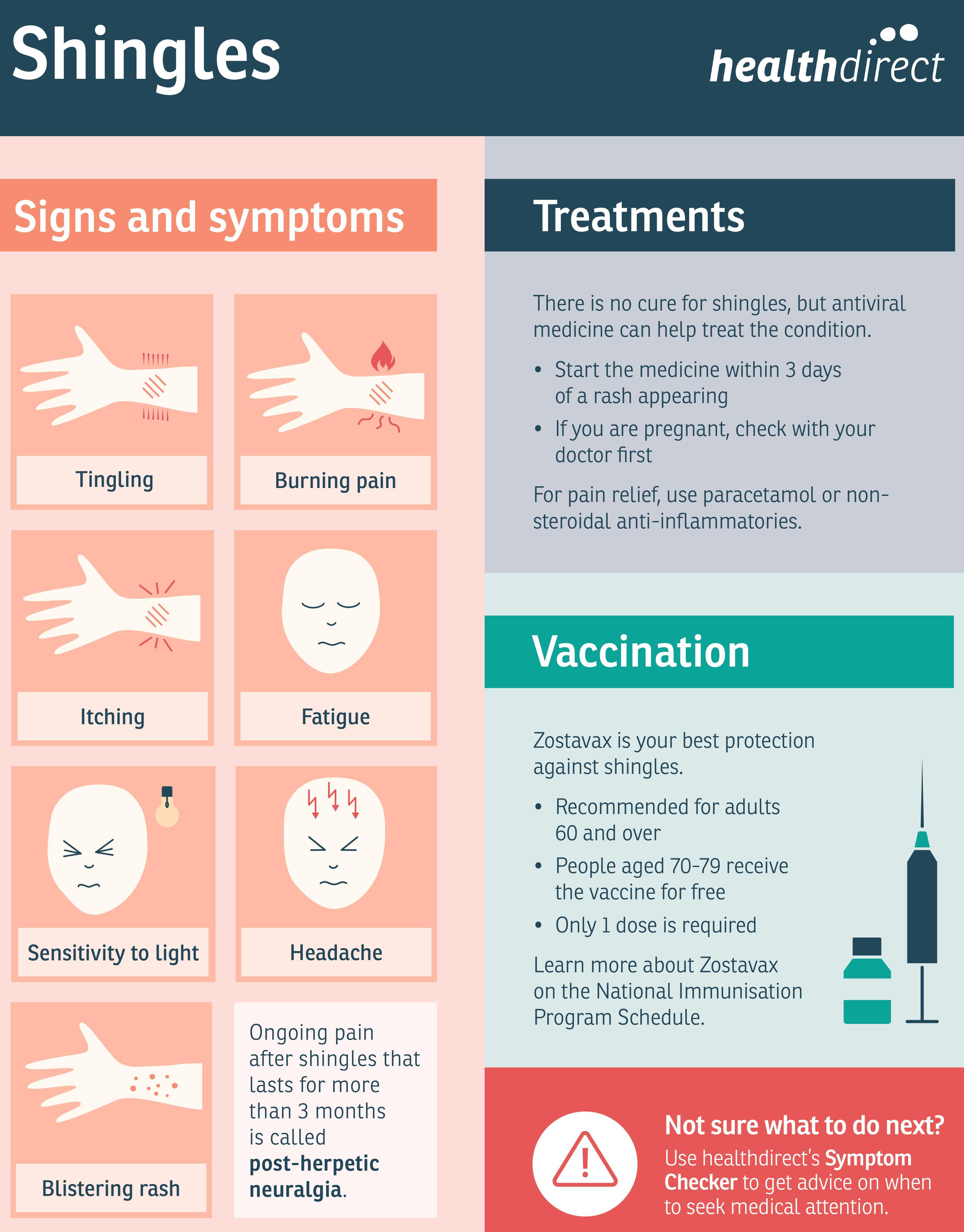
A reactivation of the chickenpox virus in the body, causing a painful rash. Anyone who’s had chickenpox may develop shingles. It isn’t known what reactivates the virus.Shingles causes a painful rash that may appear as a stripe of blisters on the trunk of the body. Pain can persist even after the rash is gone (this is called postherpetic neuralgia).Treatments include pain relief and antiviral medications such as acyclovir or valacyclovir. A chickenpox vaccine in childhood or a shingles vaccine as an adult can minimize the risk of developing shingles.