From a MD Magazine online release:
 The investigators discovered that patients with a higher genetic risk for depression were more likely to be diagnosed with depression over the next 2 years. However, more physically active patients at baseline were less likely to depression, even after they accounted for genetic risks.
The investigators discovered that patients with a higher genetic risk for depression were more likely to be diagnosed with depression over the next 2 years. However, more physically active patients at baseline were less likely to depression, even after they accounted for genetic risks.
Increasing physical activity could pay dividends for people with a high risk of developing depression.
A team from Massachusetts General Hospital (MGH) recently discovered that several hours of weekly exercise result in a decreased chance to be diagnosed with a new episode of depression, even in patients with a higher genetic risk of developing Major Depressive Disorder (MDD).
The team examined the genomic and electronic health record (EHR) data of approximately 8000 patients in the Partners Healthcare Biobank, which represents the first study to show how physical activity influences depression despite genetic risk.



 “The results we saw were stunning and suggest that holistically addressing aging via gene therapy could be more effective than the piecemeal approach that currently exists,” said first author Noah Davidsohn, a former research scientist at the Wyss Institute and HMS who is now chief technology officer of Rejuvenate Bio. “Everyone wants to stay as healthy as possible for as long as possible, and this study is a first step toward reducing the suffering caused by debilitating diseases.”
“The results we saw were stunning and suggest that holistically addressing aging via gene therapy could be more effective than the piecemeal approach that currently exists,” said first author Noah Davidsohn, a former research scientist at the Wyss Institute and HMS who is now chief technology officer of Rejuvenate Bio. “Everyone wants to stay as healthy as possible for as long as possible, and this study is a first step toward reducing the suffering caused by debilitating diseases.”

 For new patients, whose visits entail more work than those of established patients,
For new patients, whose visits entail more work than those of established patients, 

 The plot line of The Farewell is familiar to me. Like Billi’s Nai Nai, my aunt was diagnosed with metatastic lung cancer. Nobody in the family told her – nor did the doctors when she later underwent surgery to remove a tumour. The last time I saw her was in north-eastern China a few years ago. Her once-plump figure had shrunk to a wiry frame. She was in her early 70s, in good spirits, but a far cry from the feisty matriarch who used to dominate conversations.
The plot line of The Farewell is familiar to me. Like Billi’s Nai Nai, my aunt was diagnosed with metatastic lung cancer. Nobody in the family told her – nor did the doctors when she later underwent surgery to remove a tumour. The last time I saw her was in north-eastern China a few years ago. Her once-plump figure had shrunk to a wiry frame. She was in her early 70s, in good spirits, but a far cry from the feisty matriarch who used to dominate conversations.


 The tool is simply called Preventive Health, and is now available to Facebook users in the United States. It takes a user’s age and sex from their Facebook profile and provides them with a list of recommended screenings based on those two data points.
The tool is simply called Preventive Health, and is now available to Facebook users in the United States. It takes a user’s age and sex from their Facebook profile and provides them with a list of recommended screenings based on those two data points.
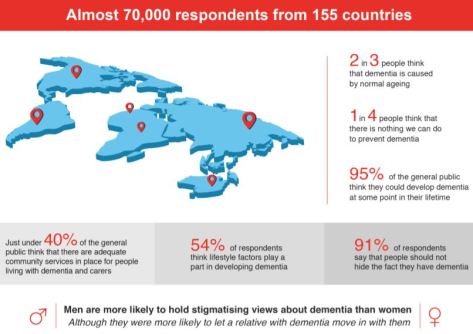
 LSE developed the survey to target four key groups:
LSE developed the survey to target four key groups: In the survey analysis we highlight the behavioural element first, giving prominence to the voices and experiences of people living with dementia as direct assessment of actual behaviour is central to discrimination and is the closest representation of the true impact of stigma on people living with dementia.
In the survey analysis we highlight the behavioural element first, giving prominence to the voices and experiences of people living with dementia as direct assessment of actual behaviour is central to discrimination and is the closest representation of the true impact of stigma on people living with dementia.
 The current study points to the role of norepinephrine, a neurotransmitter that signals arousal and stress in the central nervous system. This chemical is present in low levels in the brain while we sleep, but when production ramps up it arouses our nerve cells, causing us to wake up and become alert. The study showed that norepinephrine also acts on a specific receptor, the beta2 adrenergic receptor, which is expressed at high levels in microglia. When this chemical is present in the brain, the microglia slip into a sort of hibernation.
The current study points to the role of norepinephrine, a neurotransmitter that signals arousal and stress in the central nervous system. This chemical is present in low levels in the brain while we sleep, but when production ramps up it arouses our nerve cells, causing us to wake up and become alert. The study showed that norepinephrine also acts on a specific receptor, the beta2 adrenergic receptor, which is expressed at high levels in microglia. When this chemical is present in the brain, the microglia slip into a sort of hibernation.