From an Innovation In Aging online release:
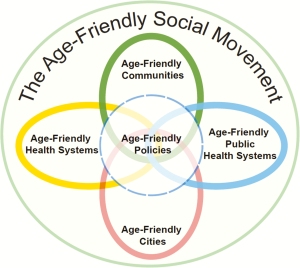 Becoming an Age-Friendly Health System entails reliably acting on a set of four evidence-based elements of high-quality care and services, known as the “4Ms,” for all older adults. When implemented together, the 4Ms represent a broad shift to focus on the needs of older adults:
Becoming an Age-Friendly Health System entails reliably acting on a set of four evidence-based elements of high-quality care and services, known as the “4Ms,” for all older adults. When implemented together, the 4Ms represent a broad shift to focus on the needs of older adults:
- (1) What Matters: Know and align care with each older adult’s specific health outcome goals and care preferences including, but not limited to, end-of-life care and across settings of care;
- (2) Medication: If medication is necessary, use Age-Friendly medication that does not interfere with What Matters to the older adult, Mobility, or Mentation across settings of care;
- (3) Mentation: Prevent, identify, treat, and manage dementia, depression, and delirium across settings of care; and
- (4) Mobility: Ensure that older adults move safely every day to maintain function and do What Matters
The Age-Friendly Health Systems movement, initiated in 2017, recognizes that an all-in, national response is needed to embrace the health and well-being of the growing older adult population. Like public health, health systems, including payers, hospitals, clinics, community-based organizations, nursing homes, and home health care, need to adopt a new way of thinking that replaces unwanted care and services with aligned interventions that respect older adults’ goals and preferences. Becoming an Age-Friendly Health System entails reliably acting on a set of four evidence-based elements of high-quality care and services, known as the “4Ms,” for all older adults.